Comprehensive Guide to Female Sexual Dysfunction: Causes, Symptoms, and Solutions
Sexual Dysfunction in Female
- Home
- Sexual Dysfunction in Female
Sexual Dysfunction in Female
Effective Homeopathic Treatment for Sexual Dysfunction in Female
Female sexual dysfunction refers to a variety of issues that impact a woman’s ability to engage in or enjoy sexual activity. This condition can affect sexual desire, arousal, orgasm, and cause pain during intercourse, often leading to emotional distress and relationship challenges. The causes of sexual dysfunction in women are diverse, including physical, emotional, psychological, hormonal, and relationship factors. It can be either temporary or chronic, affecting a woman’s overall well-being and sexual health..
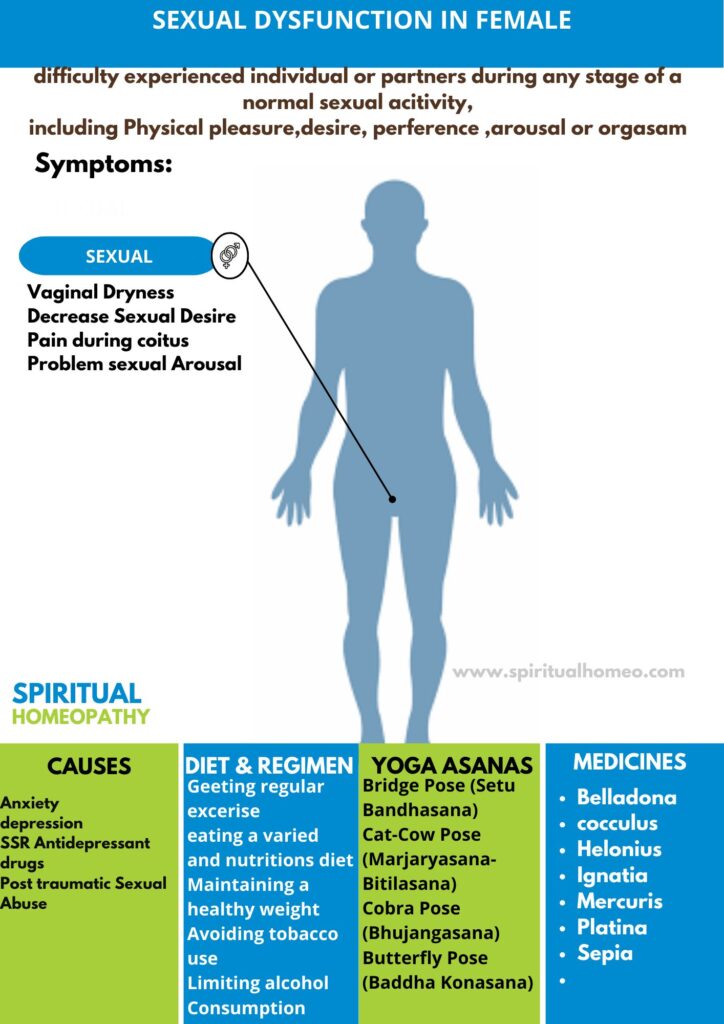
Everything You Need to Know
Overview
Female sexual dysfunction (FSD) encompasses a range of issues, including problems with sexual desire, arousal, pain during intercourse, and difficulty achieving orgasm. Similar to males, risk factors for FSD include cardiovascular disease, endocrine disorders, hypertension, neurological issues, and smoking.
While data on FSD is limited, estimates suggest that up to 43% of women experience at least one form of sexual problem. Despite growing interest in the organic causes of FSD, disorders related to desire and arousal continue to be the most common issues reported in community-based surveys.
Evaluation and guidance for FSD may benefit from a comprehensive, individualized approach. Spiritual Homeopathy Clinic, with multiple branches in Hyderabad, offers in-clinic, online, and international consultations for women seeking professional assessment and supportive long-term management.
Types of Female Sexual Dysfunction
1. Sexual Desire Disorder (Hypoactive Sexual Desire Disorder)
Sexual desire disorder, also known as hypoactive sexual desire disorder (HSDD), is characterized by a significant decrease or absence of sexual desire or libido, including a lack of sexual fantasies or thoughts.
Causes of Sexual Desire Disorder in Women
Low estrogen levels
Aging
Pregnancy
Certain long-term medications
Psychiatric conditions such as depression and anxiety
Understanding these contributing factors helps guide individualized care based on a woman’s physical, emotional, and lifestyle context.
2. Sexual Arousal Disorder
Sexual arousal disorder, formerly referred to as frigidity, includes a range of issues related to sexual arousal, such as lack of excitement and pleasure during sexual activity. It affects people of all genders and may manifest as aversion to or avoidance of sexual contact with a partner.
Common causes include:
Insufficient vaginal lubrication
Reduced blood flow
Chronic diseases
Relationship or emotional concerns
3. Orgasm Disorder
Anorgasmia:
This disorder is characterized by persistent difficulty or inability to reach orgasm despite adequate sexual stimulation, occurring in at least 75% of sexual encounters. Anorgasmia can have physical, psychological, or treatment-related origins.
Causes of Anorgasmia
Certain antidepressant therapies that may affect sexual response
Menopause (a significant number of women report changes in orgasm after menopause)
Premature Ejaculation:
In men, premature ejaculation occurs when ejaculation happens before the partner achieves orgasm or after a short duration (usually within two minutes). This condition is now understood to have neurobiological components and is not solely attributed to psychological causes.
Post-Orgasmic Illness Syndrome (POIS):
Symptoms such as rapid breathing, headaches, muscle pain, and emotional discomfort may occur shortly after orgasm. This rare condition may be mistaken for performance-related anxiety, and management typically focuses on careful evaluation and supportive care.
4. Sexual Pain Disorders
Dyspareunia (Painful Intercourse):
Pain during or after sex can result from insufficient lubrication, often related to hormonal changes, reduced arousal, or anxiety.
Vaginismus:
This condition involves involuntary muscle contractions around the vaginal area, making penetration difficult or painful. It may be associated with past trauma or fear related to sexual activity.
Vulvodynia:
Characterized by burning pain during intercourse, vulvodynia is linked to heightened sensitivity or skin-related issues in the vulvar area. The exact cause remains unclear.
Types of Female Sexual Dysfunction
Female sexual dysfunction (FSD) can be classified into four main categories, each representing different aspects of sexual health and function. These categories include:
Hypoactive Sexual Desire Disorder (HSDD)
This condition is characterized by a significant reduction or absence of sexual desire, leading to a lack of interest in sexual activity or sexual fantasies. It can be caused by various factors, including hormonal imbalances, stress, emotional concerns, or underlying health conditions. Identifying these factors is important for planning individualized care.
Sexual Arousal Disorder
Sexual arousal disorder involves difficulty achieving or maintaining sexual excitement or arousal. It may be associated with insufficient lubrication, hormonal changes such as menopause, or emotional and psychological factors. Individuals may experience reduced sexual pleasure and enjoyment during intimacy.
Orgasm Disorder (Anorgasmia)
Anorgasmia refers to the persistent inability to reach orgasm despite adequate sexual stimulation. This condition may have physical, psychological, or treatment-related causes, including menopausal changes that can affect sexual response.
Sexual Pain Disorder
Sexual pain disorders include conditions such as dyspareunia (pain during intercourse), vaginismus (involuntary muscle contractions causing pain during penetration), and vulvodynia (burning pain in the vulvar area). These disorders can significantly affect a woman’s sexual experience and overall quality of life.
Signs and Symptoms of Female Sexual Dysfunction
Female sexual dysfunction (FSD) can manifest in various ways, affecting different aspects of a woman’s sexual health, including desire, arousal, orgasm, and pain. Symptoms may involve physical, psychological, and relational factors. Below are some of the commonly reported signs and symptoms associated with female sexual dysfunction:
1. Low Sexual Desire (Hypoactive Sexual Desire Disorder)
A noticeable decline in sexual interest or desire
Absence of spontaneous sexual thoughts or fantasies
Reluctance or avoidance of sexual activity, even within a committed relationship
Feelings of frustration or distress related to reduced sexual interest
2. Sexual Arousal Problems (Female Sexual Arousal Disorder)
Difficulty becoming physically aroused or reduced vaginal lubrication during sexual activity
Limited genital response, such as reduced blood flow to the genital area
Inability to sustain sexual arousal throughout intercourse
Reduced sexual pleasure or excitement during intimacy
3. Anorgasmia (Difficulty Reaching Orgasm)
Difficulty achieving orgasm despite adequate sexual stimulation
Inconsistent or absent orgasms even with sufficient arousal
Frustration or disappointment related to difficulty reaching climax
Reduced satisfaction with sexual experiences
4. Painful Intercourse (Dyspareunia)
Pain or discomfort during vaginal intercourse or other sexual activity
Burning, stinging, or aching sensations in the genital or pelvic area during or after sex
Vaginal dryness leading to irritation or discomfort during penetration
Anxiety or fear of pain that may lead to avoidance of intimacy
5. Vaginismus
Involuntary tightening or spasms of vaginal muscles, making penetration painful or difficult
Anxiety related to anticipated pain during intercourse
Difficulty with penetration during sexual activity or gynecological examinations
6. Decreased Sexual Satisfaction
General dissatisfaction with sexual experiences
Reduced pleasure or fulfillment during intimacy
Emotional disconnection from a partner affecting sexual well-being
7. Psychological or Emotional Symptoms
Anxiety, stress, or body image concerns related to sexual performance
Low mood or emotional distress influencing sexual desire and enjoyment
Feelings of guilt, shame, or embarrassment surrounding sexual concerns
8. Relationship Issues
Difficulty communicating sexual needs or concerns with a partner
Ongoing conflicts or emotional stress affecting intimacy
Avoidance of sexual closeness due to relationship-related factors
9. Hormonal and Physical Changes
Decreased libido linked to hormonal fluctuations, including menopause or postpartum changes
Vaginal dryness or irritation associated with reduced estrogen levels
Changes in sexual response during pregnancy or after childbirth
10. Fatigue and Associated Health Conditions
Persistent fatigue reducing energy and interest in sexual activity
Chronic health conditions such as diabetes or thyroid disorders affecting sexual function
Reduced sexual desire or arousal associated with ongoing medical concerns
11. Physical Sensitivity Changes
Reduced responsiveness to touch or sexual stimulation
Difficulty maintaining arousal due to physical or hormonal changes
Altered vaginal lubrication or genital sensitivity affecting comfort and enjoyment
Diet and Lifestyle Support for Female Sexual Health: Boost Libido, Hormone Balance & Well-Being Naturally
Sexual dysfunction in females can result from physical, hormonal, emotional, and psychological factors. A holistic approach—including the right diet, regular physical activity, stress management, and healthy daily habits—may help support libido, arousal, and overall sexual well-being. Along with medical consultation, these measures can play a supportive role in long-term sexual health management.
1. Improve Blood Flow and Circulation for Enhanced Arousal
Healthy circulation plays a key role in sexual sensitivity and arousal. Including foods that support vascular health may help improve sexual response:
Nitrate-rich vegetables: Beets, spinach, arugula
Omega-3 fatty acids: Salmon, flaxseeds, chia seeds, walnuts
Flavonoid-rich fruits: Citrus fruits (oranges, grapefruit), berries (blueberries, strawberries)
2. Support Hormonal Balance Naturally
Fluctuations in estrogen, testosterone, and progesterone can influence libido and arousal. Nutrient-dense foods may help support hormonal balance:
Phytoestrogens: Soybeans, flaxseeds, chickpeas, lentils
Healthy fats: Avocados, extra virgin olive oil, nuts
Zinc and B-complex vitamins: Eggs, pumpkin seeds, quinoa, whole grains
3. Boost Libido and Enhance Mood Naturally
Certain natural foods and botanicals are traditionally associated with mood and energy support, which may indirectly influence sexual desire:
Dark chocolate: Contains compounds linked with mood regulation
Maca root: Traditionally used to support energy and vitality
Ginseng: Studied for its potential role in sexual function support
4. Hydration and Vaginal Health
Adequate hydration and gut health are important for overall comfort and well-being:
Drinking sufficient water daily may help reduce vaginal dryness and fatigue
Probiotic-rich foods such as yogurt, kefir, or sauerkraut may support vaginal and gut microbiome balance
Lifestyle and Daily Regimen for Female Sexual Wellness
1. Regular Exercise
Engaging in moderate physical activity for about 30 minutes a day, five times a week (such as brisk walking, strength training, or yoga) can help improve circulation, support hormonal balance, and reduce stress levels.
2. Stress Management
Chronic stress is commonly associated with reduced sexual desire. Practices such as meditation, deep breathing, journaling, or gentle yoga may help regulate the nervous system. Limiting excess caffeine and alcohol intake may also support hormonal stability.
3. Prioritize Sleep
Consistent, restorative sleep (7–9 hours per night) supports hormonal rhythms, emotional health, and energy levels. Poor sleep quality can negatively affect mood, libido, and overall well-being.
4. Emotional Intimacy and Connection
Emotional health plays a significant role in sexual satisfaction. Open communication with a partner regarding concerns and expectations can be helpful. In some cases, individual or couples counseling may support emotional and relationship well-being.
🧘♀️ Yoga Asanas to Enhance Female Sexual Health
Yoga can play a supportive role in female sexual health by improving flexibility, circulation, stress regulation, and mind–body awareness. These practices are not a replacement for medical care but may complement a comprehensive treatment plan when practiced regularly and under guidance.
1. Bridge Pose (Setu Bandhasana)
Benefits:
Strengthens the pelvic floor, gluteal muscles, and lower back, while supporting healthy blood flow to the pelvic region.
How to Practice:
Lie on your back with knees bent and feet flat on the floor. Gently lift your hips toward the ceiling, engaging the core and glute muscles. Hold for 30 seconds to 1 minute, breathing steadily.
2. Happy Baby Pose (Ananda Balasana)
Benefits:
Opens the hips, releases lower back tension, and promotes relaxation, which may help reduce stress-related sexual concerns.
How to Practice:
Lie on your back, bring your knees toward your chest, and hold the outer edges of your feet. Gently draw the knees downward while keeping the spine relaxed. Hold for 1–2 minutes.
3. Cat–Cow Pose (Marjaryasana–Bitilasana)
Benefits:
Improves spinal flexibility, supports pelvic awareness, and gently stimulates abdominal and pelvic organs.
How to Practice:
Begin on all fours. Inhale while arching the back (cow pose), then exhale while rounding the spine (cat pose). Continue the movement slowly for 1–2 minutes.
4. Bound Angle Pose (Baddha Konasana)
Benefits:
Stretches the hips and groin, supports pelvic circulation, and may help relieve pelvic stiffness.
How to Practice:
Sit upright with the soles of the feet together. Allow the knees to gently fall outward while keeping the spine straight. Hold for 1–2 minutes without forcing the stretch.
5. Frog Pose (Bhekasana)
Benefits:
Provides a deep stretch to the inner thighs and groin, supporting flexibility and pelvic mobility.
How to Practice:
Start on all fours and slowly widen the knees while keeping the feet inward. Lower the hips gently toward the floor. Hold for 30 seconds to 1 minute within a comfortable range.
6. One-Legged Pigeon Pose (Eka Pada Rajakapotasana)
Benefits:
Opens the hips, releases stored tension, and supports flexibility in the pelvic and lower back regions.
How to Practice:
From an all-fours position, bring one knee forward and extend the opposite leg back. Lower the hips gradually and hold for 1–2 minutes on each side.
🌬️ Breathing Techniques to Support Sexual Health
Kapalbhati Pranayama (Energizing Breath)
Benefits:
May help improve energy levels, reduce stress, and support core and pelvic muscle engagement when practiced appropriately.
How to Practice:
Sit comfortably with an upright spine. Perform gentle, rhythmic exhalations by contracting the abdomen, allowing inhalation to occur naturally. Begin with short durations and progress gradually under guidance.
🌿 Why Choose Homeopathy?
Homeopathy is a natural system of care that focuses on understanding the underlying factors contributing to illness, rather than addressing symptoms alone. It works by supporting the body’s natural regulatory mechanisms and is designed to be individualized based on a person’s physical, emotional, and lifestyle profile.
Homeopathic care is commonly used for both acute and chronic conditions as part of a holistic health approach. Management plans are tailored to individual needs and are generally well-tolerated when guided by a qualified professional.
🌟 Spiritual Homeopathy Clinic: Care with a Holistic Perspective
At Spiritual Homeopathy Clinic, care is centered on a comprehensive understanding of physical health along with emotional and lifestyle influences. The clinical approach emphasizes detailed case assessment and long-term health support, in line with established homeopathic principles.
Consultations are available at multiple branches across Reid, as well as through online and international consultation services, allowing access to care based on individual preference and location.
💫 Approach to Care at Spiritual Homeopathy Clinic
The clinic follows an individualized model of care that respects the interconnected nature of body and mind. Key aspects of the approach include:
Focus on contributing factors: Assessment goes beyond visible symptoms to understand underlying influences.
Individualized care plans: Guidance is adapted to each person’s health history, lifestyle, and concerns.
Experienced clinical guidance: Consultations are provided by qualified homeopathy practitioners.
Supportive and non-invasive approach: Homeopathy is used as part of a broader, patient-centered care plan.
Mind–body awareness: Emotional and psychological aspects are considered where relevant.
🔍 Our Consultation Process
🩺 1. Detailed Clinical Consultation
During the initial consultation, time is taken to understand medical history, current concerns, lifestyle patterns, and emotional factors. This comprehensive evaluation supports individualized planning and informed care decisions.
🔄 2. Ongoing Review and Follow-Up
Follow-up consultations allow for monitoring progress and adjusting guidance as needed. This step supports continuity of care and long-term management, particularly for chronic or recurring concerns.
❤️ Patient Care and Guidance
Care at Spiritual Homeopathy Clinic is guided by professional responsibility, clinical assessment, and patient safety. Homeopathy may be used as a complementary approach and does not replace emergency or specialist medical care when required.
When to Consult
You should consult a healthcare professional if female sexual dysfunction symptoms are persistent, cause personal distress, or begin to affect emotional well-being, relationships, or quality of life. Early evaluation helps identify physical, hormonal, psychological, or lifestyle-related contributing factors and supports appropriate care planning.
Seek consultation if you experience:
Reduced sexual desire or lack of interest over a prolonged period
Difficulty with arousal or maintaining sexual excitement
Vaginal dryness or discomfort during intimacy
Pain during or after sexual activity
Difficulty achieving satisfaction or orgasm
Sexual concerns associated with stress, anxiety, hormonal changes, or medical conditions
At Spiritual Homeopathy Clinic, consultations for female sexual dysfunction are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients who prefer privacy or are unable to visit in person. A professional assessment supports an individualized care approach based on symptoms, overall health, and personal concerns.
For appointments or guidance, contact 9069 176 176.
FAQ
1. What is female sexual dysfunction?
Female sexual dysfunction (FSD) refers to persistent problems with sexual desire, arousal, orgasm, or pain during intercourse that cause distress or relationship concerns. It can involve physical, hormonal, emotional, or psychological factors.
2. What are the common types of female sexual dysfunction?
The main types include:
Low sexual desire (Hypoactive Sexual Desire Disorder)
Sexual arousal disorder
Orgasmic disorder (Anorgasmia)
Sexual pain disorders such as dyspareunia and vaginismus
3. What causes sexual dysfunction in women?
Common contributing factors include:
Hormonal changes (such as menopause or pregnancy)
Chronic health conditions (for example, diabetes or thyroid disorders)
Psychological factors (including anxiety, depression, or past trauma)
Relationship-related concerns
Certain long-term medications
Lifestyle factors such as stress, smoking, or alcohol use
Identifying the underlying causes helps guide individualized care planning.
4. How is female sexual dysfunction diagnosed?
A healthcare professional may:
Take a detailed medical, sexual, and psychological history
Perform a physical or pelvic examination when required
Assess hormonal balance and related health conditions
Consider mental and emotional well-being as part of evaluation
5. Is female sexual dysfunction treatable?
Management depends on the underlying cause and may involve:
Counseling or supportive therapy
Lifestyle and stress-management measures
Addressing hormonal or medical factors when appropriate
Use of supportive measures such as lubricants for comfort
Treatment approaches are usually tailored to individual needs.
6. Can menopause cause sexual dysfunction?
Yes. Reduced estrogen levels during menopause may contribute to vaginal dryness, discomfort during intercourse, lowered libido, and changes in arousal or orgasm.
7. Does stress affect sexual function in women?
Yes. Ongoing stress and anxiety can influence desire, arousal, and orgasm. Stress management is often an important part of overall sexual health support.
8. What lifestyle changes can support female sexual health?
Helpful measures may include:
Regular physical activity
Balanced nutrition
Adequate sleep
Limiting alcohol and avoiding smoking
Yoga, relaxation practices, or mindfulness
Open communication within relationships
Individual recommendations may vary.
9. Are natural approaches used for female sexual dysfunction?
Some individuals explore natural or complementary approaches as part of overall care. It is advisable to discuss any such options with a qualified healthcare professional before use.
10. When should I consult a doctor?
Medical advice should be sought if:
Sexual concerns cause ongoing distress or affect relationships
Symptoms persist or worsen over time
Pain occurs during sexual activity or there is a significant change in desire
