Scabies
Schizophrenia: Causes, Symptoms, Types, Diagnosis, and Natural Treatment Guide
- Home
- Scabies
Scabies
Effective Homeopathic Treatment for Scabies
Scabies is a highly contagious skin condition caused by the microscopic itch mite (Sarcoptes scabiei). It leads to intense itching, especially at night, along with small red bumps, rashes, or blisters on the skin. The mites burrow into the skin to lay eggs, triggering an allergic reaction. Scabies spreads easily through close physical contact or sharing personal items. Early diagnosis and treatment with prescribed creams or oral medication are essential for effective relief and prevention.
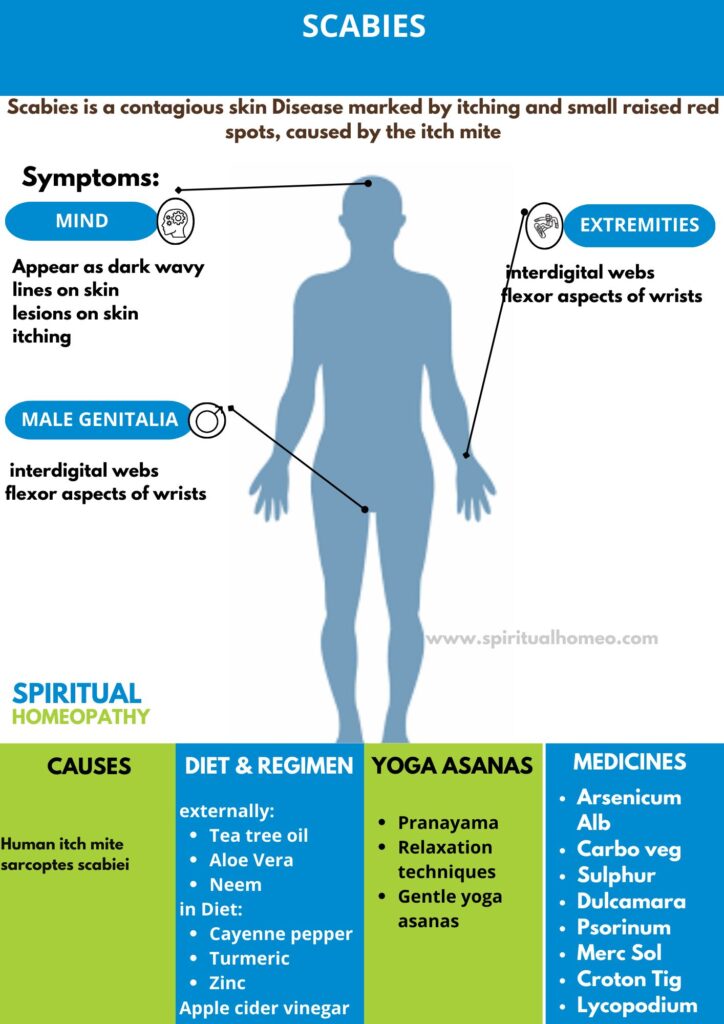
Everything You Need to Know
Overview
Scabies is a highly contagious skin condition caused by a microscopic mite known as Sarcoptes scabiei. This tiny parasite burrows into the skin, leading to intense itching—often worse at night—and a rash of small red bumps or blisters. Scabies spreads rapidly through close physical contact, making it common in families, schools, daycare centers, nursing homes, and other crowded settings.
While highly irritating, scabies is a treatable condition when diagnosed early and managed appropriately. Even after treatment, mild itching may persist for a few weeks as the skin gradually heals. Because of its contagious nature, healthcare providers often advise evaluation and care for close contacts to help prevent reinfestation. Early diagnosis and proper medical guidance are important to control symptoms and limit spread.
At Spiritual Homeopathy Clinic, consultations for skin conditions such as scabies are available across multiple branches in Hyderabad, as well as through online and international consultation options for added convenience.
Causes of Scabies: A Clear, Medical Overview
Scabies is a highly contagious skin infestation caused by the microscopic human itch mite, Sarcoptes scabiei. These tiny, eight-legged parasites burrow into the upper layer of the skin, where the female mite forms tunnels to lay eggs. After hatching, the larvae move to the skin surface, mature, and may spread to other body areas or to other individuals through close contact.
The intense itching seen in scabies is primarily an allergic reaction to the mites, their eggs, and their waste products. This itching typically becomes more noticeable at night and is considered a key symptom of the condition.
How Scabies Spreads
Direct Skin Contact: Prolonged skin-to-skin contact is the most common mode of transmission. This explains why scabies spreads easily among family members and in settings such as daycare centers, schools, nursing homes, and other crowded environments.
Indirect Contact: Less commonly, scabies may spread through shared clothing, towels, or bedding that has been used by an affected person.
Not from Animals: Animal mites may cause short-term skin irritation in humans but do not result in true human scabies, as these mites are host-specific and cannot survive long on human skin.
Mite Life Cycle
Female mites lay eggs beneath the skin surface.
Eggs hatch into larvae, which migrate to the skin surface.
Larvae mature into adult mites and continue the infestation cycle.
Mites and eggs are transmitted through close contact, allowing the cycle to persist.
Understanding the causes, transmission patterns, and life cycle of scabies helps guide individualized care and preventive measures, which may vary depending on exposure risk, symptoms, and household contacts.
Types of Scabies: SEO-Optimized, Medical Overview
Scabies is a highly contagious skin infestation caused by the Sarcoptes scabiei mite. While the condition often presents in a typical way, several types of scabies are recognized, each differing in severity, presentation, and risk factors. Understanding these forms supports accurate identification and timely care.
1. Classic Scabies
Classic scabies is the most common form and results from mite infestation beneath the skin.
Symptoms: Intense itching, especially at night, along with red bumps, blisters, or scaly patches.
Common Areas Affected: Wrists, elbows, armpits, buttocks, waistline, and genitals.
Transmission: Primarily through prolonged skin-to-skin contact, commonly among family members or people in close living environments.
2. Norwegian Scabies (Crusted Scabies)
Also known as crusted scabies, this is a more severe and highly contagious form, usually seen in individuals with weakened immune systems.
Symptoms: Thick, crusted skin lesions containing a very high number of mites; itching may be mild or absent.
Common Areas Affected: Scalp, hands, feet, and nails.
Transmission: Highly contagious due to the heavy mite load; may spread even with brief contact or via contaminated bedding or clothing.
3. Crusted Scabies
Often used interchangeably with Norwegian scabies, this form is characterized by extensive scaling and crust formation.
Symptoms: Dry, cracked crusts that may shed easily, revealing inflamed skin underneath.
Common Areas Affected: Scalp, palms, soles, and beneath fingernails.
Transmission: Extremely contagious because of the large number of mites present and requires prompt medical attention.
4. Infantile Scabies (Scabies in Babies and Children)
Infants and young children are particularly vulnerable due to sensitive skin and close contact with caregivers.
Symptoms: Severe itching, irritability, disturbed sleep, red rashes, and small blisters or pimples.
Common Areas Affected: Face, scalp, palms, and soles—areas less commonly involved in adults.
Transmission: Usually spreads through close skin contact with an infected caregiver or household member.
5. Pustular Scabies
A less common variant marked by pustules due to an inflammatory response of the skin.
Symptoms: Painful, pus-filled bumps that may resemble bacterial skin infections.
Common Areas Affected: Torso, arms, and legs.
Transmission: Similar to classic scabies, mainly through direct skin contact.
Signs and Symptoms of Scabies
Scabies typically causes intense itching (pruritus), which often worsens at night or after a hot shower. One of the hallmark signs is burrows, seen mainly in the webs between the fingers, wrists, elbows, and genital area. These burrows appear as dark, wavy lines ending in a small blister (pearly bleb) that contains the female mite.
Other key symptoms include:
Rash or red bumps in areas such as the volar wrists, elbows, penis, and buttocks
Secondary bacterial infection due to repeated scratching
Involvement of the scalp, face, neck, palms, and soles (more common in infants and young children)
Nodular scabies, frequently affecting the scrotal area
Norwegian (crusted) scabies, a severe form with thick crusts and a high mite load, typically seen in immunocompromised individuals, including those on long-term steroids or with HIV/AIDS
If itching or skin lesions are persistent, widespread, or worsening, medical evaluation is advised to confirm the diagnosis and guide appropriate care. Early diagnosis and timely management help reduce complications and limit transmission to close contacts.
Diet and Regimen for Managing Scabies: Supporting Healing and Comfort
While medical management prescribed by a qualified doctor is essential for treating scabies, a supportive diet and daily regimen can help promote skin healing, reduce irritation, and improve overall comfort during recovery.
🥗 Dietary Recommendations for Scabies
A balanced, nutrient-rich diet supports immune function and skin repair while managing scabies.
1. Immune-Boosting Nutrients
Vitamin C: Supports immune response and skin healing.
Sources: Citrus fruits, berries, bell peppers, kale, broccoli, kiwi.
Zinc: Helps with immune balance and tissue repair.
Sources: Pumpkin seeds, lentils, chickpeas, beans, whole grains.
Vitamin A: Important for skin integrity and immune support.
Sources: Carrots, sweet potatoes, dark leafy greens, eggs.
Omega-3 Fatty Acids: Help reduce inflammation and support skin health.
Sources: Fatty fish, flaxseeds, chia seeds, walnuts.
2. Anti-Inflammatory Foods
Turmeric: Known for its anti-inflammatory properties; can be added to meals.
Ginger: May help reduce inflammation when included in food or beverages.
Green Tea: Rich in antioxidants that support overall skin health.
Leafy Greens and Cruciferous Vegetables: Spinach, kale, broccoli, Brussels sprouts.
3. Hydration
Adequate fluid intake supports skin hydration and recovery.
Aim for 8–10 cups of water daily. Herbal teas such as chamomile or peppermint may also be helpful.
4. Probiotics
A healthy gut microbiome supports immune balance.
Sources: Yogurt with live cultures, kefir, fermented foods like sauerkraut or kimchi.
5. Foods to Limit or Avoid
Processed sugars and refined carbohydrates
Fried or heavily processed foods
Dairy products, if they worsen itching or skin irritation (varies by individual)
🧼 Regimen for Scabies Care
Along with dietary support, maintaining a consistent daily routine can help reduce discomfort and prevent reinfestation.
1. Follow Medical Advice
Always follow the treatment plan and hygiene instructions provided by your healthcare professional. Do not self-modify treatment without guidance.
2. Maintain Hygiene
Bathe regularly using mild cleansers; avoid harsh scrubbing.
Wash clothing, towels, and bedding regularly using appropriate cleaning methods.
Items that cannot be washed should be kept aside for a few days as advised by a doctor.
Avoid scratching to reduce the risk of secondary skin infection.
3. Skin Comfort Measures
Use gentle, fragrance-free skincare products.
Cool compresses may help soothe irritated areas.
Keep nails trimmed to minimize skin injury from scratching.
4. Rest and Stress Management
Ensure adequate sleep (7–8 hours daily).
Gentle relaxation practices such as breathing exercises or meditation may support recovery.
🧘♂️ Yoga Asanas to Support Scabies Recovery
Yoga may help support relaxation, circulation, and overall well-being during scabies recovery. These practices are supportive in nature and should be followed alongside medical care, not as a replacement.
Balasana (Child’s Pose)
Calms the nervous system and helps reduce stress, which may worsen itching.
Supports emotional comfort during skin-related discomfort.
Viparita Karani (Legs Up the Wall Pose)
Encourages gentle blood circulation and relaxation.
May help ease restlessness and nighttime discomfort.
Bhujangasana (Cobra Pose)
Supports circulation and overall vitality.
May indirectly aid skin recovery through improved blood flow.
Setu Bandhasana (Bridge Pose)
Enhances circulation and relieves physical tension.
Supports balanced metabolic and immune function.
Ardha Matsyendrasana (Seated Spinal Twist)
Aids digestion and supports internal balance.
May contribute to overall immune resilience.
Savasana (Corpse Pose)
Deeply restorative and calming.
Helps reduce stress-related inflammation and promotes relaxation.
🧴 Additional Tips During Practice:
Avoid hot yoga or excessive sweating, as heat may aggravate itching.
Wear loose, breathable clothing and use a clean yoga mat to reduce skin irritation.
Maintain hygiene before and after practice to help prevent reinfestation.
Discontinue practice and seek medical advice if symptoms worsen.
Yoga should be practiced gently and adapted to individual comfort levels, especially during active skin symptoms.
🌿 Why Choose Homeopathy?
Homeopathy is a natural system of care that focuses on understanding the underlying factors contributing to illness, rather than addressing symptoms alone. It works in alignment with the body’s self-regulatory processes and is tailored to individual needs. When followed under professional guidance, homeopathy may support long-term health and overall well-being.
It can be considered for both chronic conditions and acute health concerns, using a holistic and personalized approach to care.
🌟 Spiritual Homeopathy: Our Approach to Care
At Spiritual Homeopathy Clinic, care is centered on a comprehensive understanding of physical, emotional, and lifestyle factors that influence health. Our approach combines classical homeopathic principles with structured clinical assessment to support balanced well-being.
Rather than symptom-focused care alone, attention is given to identifying possible underlying imbalances that may contribute to recurring or persistent health issues.
💫 Why Spiritual Homeopathy Clinic
Our clinical approach emphasizes thoughtful evaluation and individualized care:
Individualized Assessment: Care plans are developed based on a person’s health history, lifestyle patterns, and presenting concerns.
Personalized Care Plans: Management strategies are tailored to individual needs and may evolve over time.
Qualified Clinical Team: Consultations are provided by trained homeopathy practitioners across multiple branches in Hyderabad, with options for online and international consultations.
Well-Tolerated Care Approach: Homeopathy is generally well-tolerated when followed under professional supervision.
Mind–Body Consideration: Emotional and psychological factors are considered as part of a holistic clinical evaluation.
🔍 Our Care Process
🩺 1. Detailed Consultation
Each consultation involves a structured discussion of symptoms, medical history, lifestyle factors, and emotional well-being to understand the overall health picture.
⚖️ 2. Individualized Management Approach
Care is planned based on the individual profile, addressing contributing factors and supporting long-term management rather than short-term symptom relief.
🔄 3. Follow-Up and Review
Periodic follow-ups allow monitoring of progress and adjustments to the care approach, as needed, under professional guidance.
When to Consult
You should consult a healthcare professional if scabies symptoms become persistent, spread rapidly, or start interfering with daily activities or sleep. Early evaluation helps confirm the diagnosis, manage symptoms effectively, and reduce the risk of transmission to others.
Seek consultation if you experience:
Intense itching, especially at night
Persistent itching that does not improve over time
Red rashes, bumps, or small blisters on the skin
Burrow-like lines on the skin, commonly between fingers, wrists, elbows, waist, or genitals
Skin sores or infections caused by repeated scratching
Similar itching or skin symptoms in family members or close contacts
At Spiritual Homeopathy Clinic, consultations for scabies are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients who are unable to visit the clinic in person. A professional assessment helps support an individualized care approach based on symptoms, skin condition, and overall health status.
For appointments or guidance, contact 9069 176 176.
FAQs About Scabies
1. What is scabies?
Scabies is a highly contagious skin condition caused by a microscopic mite (Sarcoptes scabiei). It leads to intense itching, often worse at night, and a pimple-like rash due to mites burrowing under the skin.
2. How do you get scabies?
Scabies spreads mainly through prolonged skin-to-skin contact with an infected person. Less commonly, it may spread through shared bedding, clothing, or towels.
3. What are the first signs of scabies?
Early signs usually include intense itching and a rash with small red bumps, commonly seen between the fingers, wrists, elbows, armpits, waistline, and genital area.
4. Is scabies contagious?
Yes, scabies is highly contagious and can spread quickly in households, schools, nursing homes, and other close-contact settings.
5. How is scabies diagnosed?
Diagnosis is usually based on clinical examination of the skin, including rash patterns and burrow marks. In some cases, additional tests may be used to support the diagnosis.
6. How is scabies managed medically?
Management typically involves medical treatment aimed at eliminating mites and reducing symptoms. Early diagnosis and adherence to medical advice are important for effective control.
7. Can scabies be managed with natural or supportive care alone?
Supportive measures may help relieve discomfort but are not sufficient to eliminate mites. Medical guidance is essential for appropriate management.
8. How long does it take for symptoms to improve?
After appropriate treatment, mites are usually controlled within a short period, but itching may continue for a few weeks as the skin recovers.
9. Should family members be evaluated if one person has scabies?
Yes. Close contacts are often advised to seek medical evaluation, even if symptoms are not present, to help prevent reinfestation.
10. How can scabies recurrence be reduced?
Maintaining hygiene, cleaning clothing and bedding properly, and following medical guidance can help reduce the risk of recurrence.
