Piles and haemorrhoid
Get Relief from Piles & Haemorrhoids – Trusted Treatments & Advice
- Home
- Piles and haemorrhoid
Piles and haemorrhoid
Homeopathy treatment for Piles and haemorrnoid
What Are Piles or Haemorrhoids?
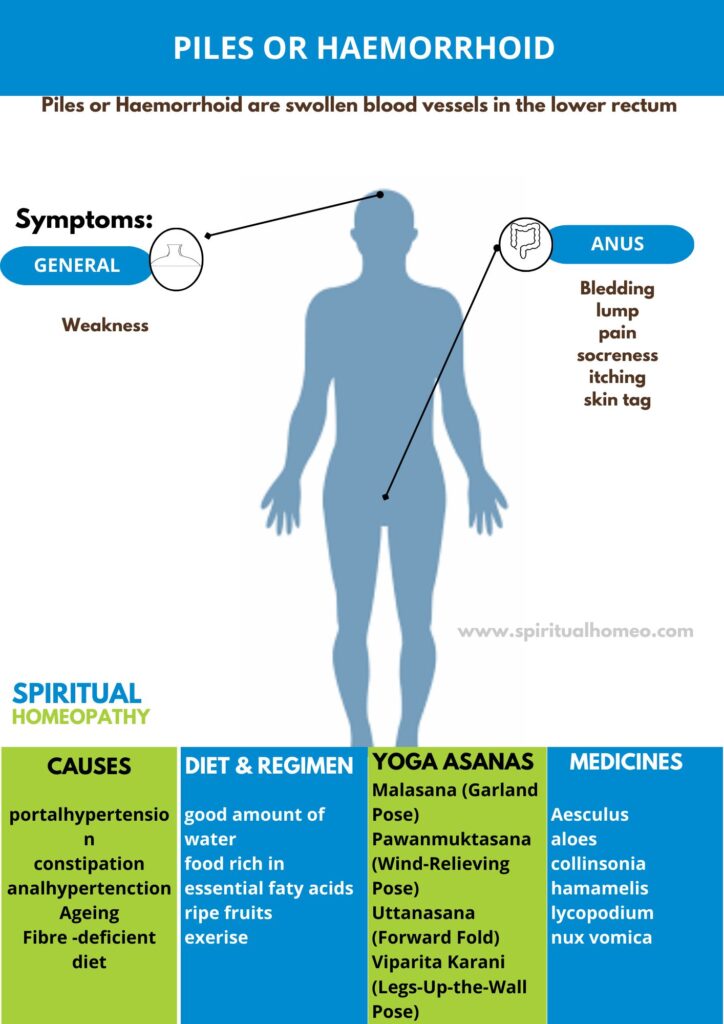
Piles, also known as haemorrhoids (or hemorrhoids in American English), are swollen blood vessels located in the lower rectum and anus. Normally, these vascular structures act as cushions that help control bowel movements. However, when they become enlarged, swollen, or inflamed, they lead to discomfort and are referred to as haemorrhoidal disease. Common symptoms include pain, itching, bleeding, and difficulty during stool passage.
Everything You Need to Know
Overview
Hemorrhoids: Prevalence, Risk Factors, and Dietary Impact
Symptomatic hemorrhoids affect over one million people each year in the Western world. While hemorrhoidal disease can occur in individuals of any age or gender, increasing age is considered a significant risk factor. The condition is reported less frequently in underdeveloped countries, which is thought to be related to differences in dietary patterns and lifestyle habits.
One major contributor to the higher prevalence in developed nations is the typical Western diet, which is often low in dietary fiber and high in fat. Such dietary patterns are commonly associated with constipation and straining during bowel movements—two important factors that increase the likelihood of developing symptomatic hemorrhoids.
Best Homeopathy Doctor for Piles in Hyderabad
Our clinic provides effective homeopathy treatment for piles using safe and natural medicines. Our experienced team of homeopathy doctors focuses on treating the root cause of piles and preventing recurrence. Patients can consult our doctors for piles treatment at our clinics in Hyderabad, including Dilsukhnagar, KPHB, Chandanagar, and Nallagandla. We aim to provide long-term relief without surgery through personalized treatment plans.
Consult Our Doctor for Piles Treatment
If you are experiencing symptoms of piles such as pain, bleeding, or discomfort, our experienced homeopathy doctors can help. Early treatment can prevent complications and improve recovery.
Understanding the Causes of Haemorrhoids: Myths, Facts, and Modern Insights
For centuries, misconceptions about the vascular anatomy of the anal canal led to various outdated theories about the development of primary internal haemorrhoids. Early beliefs linked haemorrhoids to upright posture, the absence of valves in the portal venous system, and increased abdominal pressure—suggesting these factors caused anal varicosities.
However, modern studies have clarified many of these assumptions. If raised portal pressure were a direct cause, haemorrhoids would be significantly more common in individuals with portal hypertension. While such patients may develop anorectal varices, these are clinically and anatomically distinct from haemorrhoids and do not occur more frequently than in the general population.
Historical Vascular Theories and Infection Myths
In the past, haemorrhoids were also compared to vascular growths such as hemangiomas or attributed to changes in erectile tissue involved in continence, including hyperplasia of the so-called corpus cavernosum recti. Some theories proposed that repeated infections or trauma during bowel movements weakened venous walls. Current understanding shows that the anal canal is highly resistant to infection, and its mucosa demonstrates strong healing capacity, even with constant bacterial exposure.
Diet, Constipation, and Straining
Chronic constipation and associated straining are now recognized as important contributing factors. Diets low in fiber can slow intestinal transit, leading to hard stools that require increased effort to pass. Prolonged straining, extended time spent on the toilet, and relaxation of the perineum may interfere with venous return, resulting in engorgement of anal veins. However, constipation alone does not explain all cases. Haemorrhoids are also observed in individuals with diarrhoeal conditions, indicating that both extremes of bowel habits may contribute.
Anal Muscle Tone and Pressure
Anal hypertonia, or increased resting pressure in the anal canal, has also been associated with haemorrhoids. It remains unclear whether this elevated tone is a cause or a consequence of the condition. While normalization of anal pressure is sometimes observed after surgical intervention, this does not establish a direct causal relationship. Conversely, some individuals present with a lax anal canal and mucosal prolapse, occasionally linked to perineal descent or pudendal nerve involvement.
The Role of Ageing
Age-related changes play a significant role. In younger individuals, anal cushions are supported by strong, elastic connective tissue. With ageing, these tissues may fragment and lose elasticity, often due to repeated straining during defaecation. Although more common with advancing age, similar changes can also be seen in younger patients with severe haemorrhoids.
Current Understanding of Haemorrhoid Development
The prevailing view is that repeated mechanical shearing forces during bowel movements lead to downward displacement of the anal cushions. Ongoing pressure and trauma weaken the supporting structures, limiting their ability to retract after defaecation and resulting in the typical symptoms of haemorrhoidal disease.
Common Risk Factors for Piles
Several lifestyle and health factors can increase the risk of developing piles. These include chronic constipation, prolonged sitting, low fiber intake, obesity, pregnancy, and lack of physical activity. Identifying these risk factors early and seeking timely treatment can help prevent the condition from worsening.
Classification of Piles (Haemorrhoids): Internal and External Types Explained
Haemorrhoids, commonly known as piles, are classified into two main types based on their location in relation to the dentate (pectinate) line of the anal canal: external haemorrhoids and internal haemorrhoids. This classification helps in understanding symptoms and guiding appropriate management.
1. External Haemorrhoids
External haemorrhoids develop below the dentate line and are covered by squamous epithelium, similar to the skin outside the body. These haemorrhoids may coexist with an internal component but are more likely to cause discomfort. Pain, swelling, and tenderness are especially noticeable when thrombosis occurs, which means a blood clot forms within the haemorrhoid, leading to acute symptoms.
2. Internal Haemorrhoids
Internal haemorrhoids arise above the dentate line and are covered by mucosa and transitional epithelium. Due to the absence of pain-sensitive nerve endings in this area, they are usually painless, even when bleeding occurs. Internal haemorrhoids account for most cases and form the basis of standard clinical grading systems.
Haemorrhoid Grading Based on Severity
Internal haemorrhoids are further classified according to the degree of prolapse:
Grade I – No prolapse; haemorrhoids are visible only during examination or endoscopy.
Grade II – Prolapse occurs during straining but reduces spontaneously.
Grade III – Prolapse during defaecation and requires manual reduction.
Grade IV – Permanently prolapsed and cannot be manually reduced.
External and Internal Haemorrhoids: Symptoms, Diagnosis, and Severity
External Haemorrhoids
External haemorrhoids form below the dentate line and are covered by skin-like tissue. In many cases, they cause few or no symptoms unless they become thrombosed (develop a blood clot). When thrombosed, they can become very painful, with swelling and tenderness around the anus.
Pain and Swelling: The pain is typically sudden and intense but often subsides within 2–3 days, although swelling may persist for a few weeks.
Skin Tags: After healing, a residual skin tag may remain.
Irritation and Itching: Large external haemorrhoids can make personal hygiene difficult, leading to local irritation and itching.
Internal Haemorrhoids
Internal haemorrhoids develop above the dentate line and are usually painless, even when bleeding occurs, due to the lack of pain-sensitive nerve endings in this area.
Bleeding: The most common and earliest symptom is bright red bleeding during or after bowel movements. Blood may be noticed on toilet paper, on the surface of the stool, or dripping into the toilet.
Prolapse: Internal haemorrhoids may protrude outside the anus, appearing as a perianal lump. They may reduce on their own or require manual assistance.
Other Symptoms: These can include mucus discharge, itching, anal irritation, and occasionally mild fecal leakage.
Pain: Pain is uncommon and, when present along with bleeding, may indicate thrombosis or another anorectal condition that requires evaluation.
Grading of Internal Haemorrhoids
Internal haemorrhoids are graded according to the extent of prolapse:
Grade I: No prolapse; bleeding may be the only symptom.
Grade II: Prolapse during defecation but retracts spontaneously.
Grade III: Prolapse requires manual reduction.
Grade IV: Permanently prolapsed and cannot be reduced.
As haemorrhoids progress, the pile masses may enlarge and become edematous, leading to increased discomfort and the development of cutaneous (skin) components.
Additional Symptoms and Complications
In more advanced cases, patients may experience:
Persistent irritation and itching due to mucus secretion from prolapsed rectal mucosa
Difficulty maintaining hygiene because of an irregular anal margin
Minor leakage due to reduced effectiveness of the anal seal
Rarely, chronic blood loss that may contribute to anemia
Diagnosis of Haemorrhoids
Accurate diagnosis involves a combination of visual and physical assessment:
External haemorrhoids: Often visible during routine physical examination
Digital Rectal Examination (DRE): A gloved, lubricated finger is used to assess for masses or other abnormalities
Anoscopy or Proctoscopy: As internal haemorrhoids are usually soft and not easily felt, instruments such as an anoscope, proctoscope, or sigmoidoscope may be used for direct visualization
When to Consult a Doctor for Piles
You should consult a homeopathy doctor for piles if you notice symptoms such as bleeding during bowel movements, pain while passing stool, itching around the anus, or swelling near the rectal area. Early treatment helps prevent complications and improves recovery. Our doctors provide treatment for piles at our clinics across Hyderabad.
Diet and Lifestyle Tips to Manage and Prevent Haemorrhoids (Piles)
A healthy diet and balanced lifestyle play an important role in managing haemorrhoids and reducing the likelihood of recurrence. Simple, consistent changes in eating habits and daily routines can help ease symptoms such as pain, swelling, itching, and bleeding, while supporting overall digestive health.
Best Diet for Haemorrhoids: What to Eat and Avoid
✅ Increase Fiber Intake
Why: A high-fiber diet helps soften stools and promotes smoother bowel movements, reducing straining—a key contributing factor in haemorrhoids.
What to Eat:
Whole grains (oats, brown rice, whole wheat bread)
Fruits (apples, pears, bananas, berries)
Vegetables (carrots, spinach, broccoli, kale)
Legumes (lentils, chickpeas, black beans)
Nuts and seeds (flaxseeds, chia seeds, almonds)
💧 Stay Hydrated
Why: Adequate fluid intake supports soft stool consistency and helps prevent constipation.
Tip: Aim for about 8–10 glasses (2–2.5 liters) of water daily. Herbal teas and clear broths may also contribute to hydration.
🚫 Avoid Low-Fiber and Processed Foods
Why: Refined and processed foods can contribute to hard stools and constipation, which may worsen symptoms.
What to Limit:
White bread and refined grains
Sugary snacks
Fast food and packaged meals
🥑 Include Healthy Fats
Why: Healthy fats can support smoother digestion and regular bowel movements.
Sources:
Avocados
Olive oil
Fatty fish
Nuts and seeds
🦠 Add Probiotics for Gut Health
Why: Probiotics support a balanced gut microbiome and regular digestion.
Probiotic-Rich Foods:
Yogurt
Kefir
Kimchi
Sauerkraut
☕ Limit Caffeine and Alcohol
Why: Excess caffeine and alcohol may contribute to dehydration and harder stools.
Tip: Moderate intake and increase water consumption if these beverages are consumed.
🧂 Reduce Salt Intake
Why: High salt intake can lead to water retention and swelling, potentially aggravating haemorrhoids.
Avoid: Salty snacks, processed meats, and high-sodium packaged foods.
Daily Habits to Help Manage Haemorrhoids
🏃 Exercise Regularly
Why: Physical activity supports healthy bowel movements and improves circulation.
How: Aim for around 30 minutes of moderate activity, such as walking, swimming, or yoga, on most days.
🪑 Avoid Prolonged Sitting
Why: Long periods of sitting increase pressure on anal veins.
Tip: Take short movement breaks every 30–60 minutes, and avoid spending extended time on the toilet.
🚽 Practice Healthy Toilet Habits
Why: Proper bowel habits reduce strain and irritation.
Best Practices:
Respond promptly to the urge to pass stools
Avoid straining or sitting too long
Use a footstool to support better posture during bowel movements
🛁 Take Warm Sitz Baths
Why: Warm water can help soothe pain, itching, and local discomfort.
How: Sit in warm water for 10–15 minutes, especially after bowel movements, once or twice daily.
🧻 Maintain Good Hygiene
Why: Gentle hygiene helps prevent irritation.
Tips:
Use soft, unscented cleansing options
Gently pat the area dry after washing
Avoid harsh or fragranced products
❄️ Apply Cold Compresses
Why: Cold application may help reduce swelling and discomfort.
How: Apply a cold pack wrapped in a cloth for short intervals as needed.
🧱 Avoid Heavy Lifting
Why: Heavy lifting increases abdominal pressure and may worsen symptoms.
How: Avoid unnecessary lifting and use proper technique when lifting is unavoidable
✅ Best Yoga Asanas for Piles (Haemorrhoids)
Yoga practices can play a supportive role in managing haemorrhoids by improving digestion, circulation, and bowel regularity. These practices are meant to complement medical care and lifestyle measures, not replace professional evaluation.
1. Malasana (Garland Pose)
Benefits: Opens the hips, stretches the lower back, and supports smoother bowel movements.
How to do:
Squat with your feet flat on the floor.
Bring your palms together in a prayer position at chest level.
Use your elbows to gently press the knees outward.
Hold for 30 seconds to 1 minute while breathing steadily.
2. Pawanmuktasana (Wind-Relieving Pose)
Benefits: Helps relieve gas and bloating, improves digestion, and supports intestinal function.
How to do:
Lie on your back and bring one or both knees toward the chest.
Hold the shins and gently pull the knees in.
Keep the head relaxed on the floor or gently raise it toward the knees.
Hold for 20–30 seconds and repeat.
3. Viparita Karani (Legs Up the Wall Pose)
Benefits: Enhances blood circulation, reduces pressure in the rectal area, and promotes relaxation.
How to do:
Lie on your back with legs extended vertically against a wall.
Relax your arms alongside the body.
Hold the position for 5–10 minutes.
4. Balasana (Child’s Pose)
Benefits: Relieves stress and tension, gently stretches the lower back, and supports digestive comfort.
How to do:
Sit on your heels, bend forward, and stretch the arms ahead.
Rest the forehead on the mat.
Hold for 1–2 minutes with slow, deep breathing.
5. Bhujangasana (Cobra Pose)
Benefits: Stimulates abdominal organs, supports digestion, and may ease constipation.
How to do:
Lie on your stomach with hands under the shoulders.
Inhale and gently lift the chest, keeping elbows slightly bent.
Hold for 15–30 seconds without strain.
6. Sarvangasana (Shoulder Stand)
Benefits: Supports circulation and may help with bowel regularity.
Note: This posture should be practiced under guidance, especially for beginners or individuals with neck issues or high blood pressure.
How to do:
Lie on your back and lift the legs upward, supporting the hips with the hands.
Keep the body aligned and steady.
Hold for 30 seconds to 1 minute.
7. Ashwini Mudra (Horse Gesture)
Benefits: Helps tone pelvic floor muscles and supports blood flow in the anal region.
How to do:
Sit in a comfortable meditative posture.
Gently contract and relax the anal sphincter muscles.
Perform 10–15 repetitions.
🌿 Why Choose Homeopathy?
Homeopathy is a system of care that focuses on understanding the underlying factors of illness, not only the outward symptoms. It works alongside the body’s natural regulatory processes and follows an individualized approach based on a person’s physical, emotional, and lifestyle profile. When used under professional guidance, homeopathy is generally well-tolerated and suitable for long-term management of various health conditions.
This approach may be considered for both chronic conditions and acute concerns, with care plans tailored to individual needs rather than a one-size-fits-all model.
🌟 Spiritual Homeopathy Clinic: Approach to Care
At Spiritual Homeopathy Clinic, the focus is on providing structured, individualized homeopathic care using classical principles supported by clinical assessment. The emphasis remains on understanding the full health picture—physical symptoms, emotional factors, and lifestyle influences—to support balanced care over time.
Consultations are available at multiple branches in Hyderabad, as well as through online and international consultation options for patients who are unable to visit in person.
💫 What Guides the Homeopathic Approach Here?
The care approach is shaped by the following principles:
Individualized Care: Each case is assessed on its own merits, considering symptoms, triggers, and overall health status.
Addresses Contributing Factors: Attention is given to possible physical, emotional, and lifestyle contributors to illness.
Long-Term Management Focus: Suitable for conditions that require ongoing monitoring and gradual improvement.
Professional Guidance: Care is provided under qualified supervision, with regular reviews as needed.
🔍 Treatment Process
Key Benefits of Our Treatment
- Non-surgical piles treatment
- Experienced homeopathy doctors
- Individualized treatment plans
- Multiple clinic locations in Hyderabad
- Safe and natural medicines
- Long-term relief approach
1. In-Depth Consultation
The consultation involves a detailed discussion of medical history, current concerns, lifestyle patterns, and emotional well-being to support an individualized care plan.
2. Individualized Homeopathic Care
Care strategies are selected based on the complete clinical picture and adjusted as required during follow-ups. The focus remains on supporting the body’s balance rather than symptom suppression alone.
3. Follow-Up and Monitoring
Periodic follow-ups help assess response, note changes, and refine the care approach when necessary. This ongoing review supports safe and responsible management.
❤️ Care and Responsibility
Homeopathy is used as a complementary system of care and does not replace emergency or specialized medical treatment when required. Patients are advised to seek prompt medical attention for severe, rapidly worsening, or unclear symptoms.
When to Consult
You should consult a healthcare professional if piles (haemorrhoids) symptoms become frequent, persistent, or start affecting your daily activities and comfort. Early evaluation helps identify contributing factors and supports timely, appropriate care.
Seek consultation if you experience:
Recurrent or ongoing rectal bleeding
Pain, swelling, or discomfort around the anus
Itching, irritation, or mucus discharge that does not settle
Prolapse (lump coming out of the anus) that does not reduce easily
Symptoms that worsen over time or interfere with daily routine
No improvement despite dietary and lifestyle measures
At Spiritual Homeopathy Clinic, consultations are available across multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients unable to visit in person. A professional assessment helps plan individualized care based on symptoms, severity, and overall health.
For appointments or guidance, contact 9069 176 176.
FAQS
1. What are piles or haemorrhoids?
Piles, or haemorrhoids, are swollen blood vessels in the rectum or anus. They may be internal (inside the rectum) or external (under the skin around the anus) and can cause discomfort, itching, bleeding, or pain during bowel movements.
2. What causes haemorrhoids?
Common causes include chronic constipation, straining during bowel movements, a low-fiber diet, prolonged sitting, obesity, pregnancy, and ageing. Poor bowel habits and lifestyle factors may also contribute. Understanding these causes helps guide individualized care.
3. What are the symptoms of piles?
Symptoms may include:
Bright red rectal bleeding
Pain or discomfort during bowel movements
Itching or irritation near the anus
Swelling or lumps around the anus
Mucous discharge
Prolapse (lumps that come out during straining)
If symptoms are frequent, persistent, or severe, medical consultation is advised.
4. Are piles dangerous?
Haemorrhoids are usually not life-threatening, but they can cause significant discomfort. In some cases, complications such as thrombosis, persistent bleeding, or infection may occur. Rarely, long-term bleeding can lead to anaemia.
5. Can piles go away on their own?
Mild haemorrhoids may improve with dietary and lifestyle changes. However, ongoing or worsening symptoms should be evaluated by a healthcare professional.
6. How are haemorrhoids diagnosed?
Diagnosis may include:
Physical examination (for external haemorrhoids)
Digital rectal examination
Anoscopy, proctoscopy, or sigmoidoscopy for internal haemorrhoids
7. What are the treatment options for piles?
Treatment depends on severity and may involve:
Dietary and lifestyle measures
Local supportive care
Minimally invasive procedures
Surgical options in advanced cases
The choice of management is based on individual assessment and clinical findings.
8. Can diet help prevent or manage piles?
Yes. A diet rich in fiber (fruits, vegetables, whole grains, legumes) along with adequate fluid intake helps reduce constipation and straining, which may lower symptom frequency.
9. Are piles the same as anal fissures or fistulas?
No. These are different conditions:
Piles are swollen veins
Fissures are small tears in the anal lining
Fistulas are abnormal connections between the rectum and nearby skin
10. When should I see a doctor for haemorrhoids?
Medical evaluation is recommended if:
Bleeding is frequent or heavy
Pain or swelling is severe
Symptoms do not improve with basic measures
A lump persists or signs of infection appear