Understanding Paralysis: Causes, Symptoms, Treatment, and Management"
Paralysis
- Home
- Paralysis
Paralysis
Effective Homeopathic Treatment for Paralysis
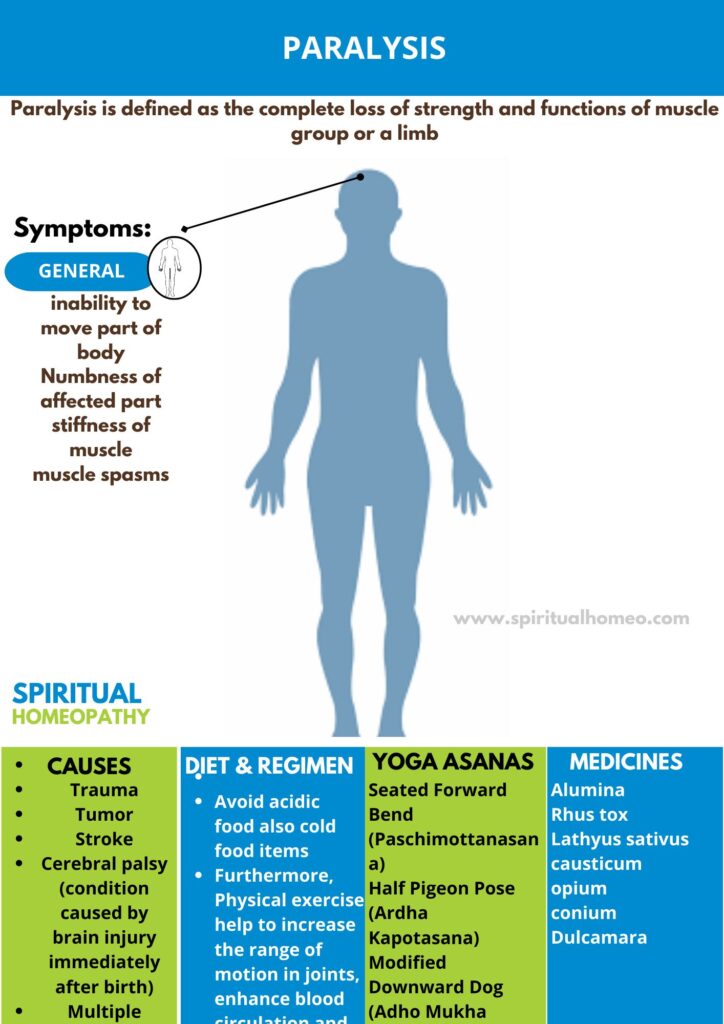
Paralysis is the loss of ability to move or feel in part or most of the body, typically caused by damage to the nervous system. It can result from various factors, including stroke, spinal cord injury, neurological disorders, or infections. Paralysis may affect a specific area, like one limb (partial paralysis), or the entire body (total paralysis). Symptoms vary depending on the severity and location of the damage and may also include loss of sensation and function in the affected areas.
Everything You Need to Know
Overview
Paralysis refers to the loss of muscle function in one or more parts of the body, often resulting from nerve damage, stroke, spinal cord injury, or certain neurological conditions. It may be temporary or long-term, depending on the underlying cause and the extent of nerve involvement. Paralysis can be categorized into different forms, including partial paralysis, complete paralysis, localized paralysis (affecting specific areas), and generalized paralysis (affecting larger areas or the entire body).
Causes of Paralysis
Common causes of paralysis include:
Trauma:
Physical injuries such as road accidents, falls, or sports injuries can damage the brain, spinal cord, or peripheral nerves, leading to partial or complete loss of muscle function.
Tumors:
Abnormal growths in the brain or spinal cord may compress nerves or neural pathways, disrupting normal signal transmission and movement.
Stroke:
An interruption of blood flow to specific areas of the brain can result in sudden loss of motor control, often affecting one side of the body.
Cerebral Palsy:
A neurological condition caused by brain injury during pregnancy, birth, or early infancy, leading to long-term movement and muscle coordination difficulties.
Multiple Sclerosis:
An autoimmune disorder in which the protective covering of nerves is damaged, interfering with communication between the brain and muscles.
Neurodegenerative Diseases:
Conditions such as Parkinson’s disease and ALS involve progressive degeneration of nerve cells, which can gradually impair movement and muscle control.
Understanding the underlying cause is essential, as it helps guide an individualized care approach focused on long-term management and overall neurological health.
Classification of Paralysis
Partial Paralysis:
Affects only specific muscle groups, resulting in limited movement or reduced strength in the affected area.
Complete Paralysis:
Results in total loss of voluntary muscle movement, which may involve a limb, one side of the body, or multiple body regions.
Temporary Paralysis:
Caused by external or reversible factors such as neurotoxins, venom from snake bites, or jellyfish stings, and may improve with timely medical care.
Permanent Paralysis:
A long-term or irreversible condition, usually resulting from significant damage to the brain, spinal cord, or major nerves.
Types of Paralysis Based on Muscle Tone
Flaccid Paralysis:
Muscles become soft, limp, and weak, often accompanied by muscle wasting due to reduced nerve stimulation.
Spastic Paralysis:
Muscles remain stiff and tight, with involuntary jerking or spasms caused by disrupted nerve signals.
Types of Paralysis Based on Affected Areas
Monoplegia:
Paralysis affecting one limb, such as a single arm or leg.
Hemiplegia:
Paralysis affecting one side of the body, commonly seen after a stroke.
Diplegia:
Paralysis affecting the same body parts on both sides, such as both arms or both legs.
Paraplegia:
Paralysis affecting both legs, while the upper body typically remains unaffected.
Quadriplegia (Tetraplegia):
Paralysis affecting both arms and both legs, and sometimes the torso; internal organs are usually not directly affected.
Secondary Conditions Related to Paralysis
Paralysis can lead to additional health concerns, particularly when mobility is limited and long-term care is required:
Bedsores:
Individuals confined to bed or a wheelchair may develop pressure ulcers, which can progress to infections if not managed properly.
Loss of Sensation:
Reduced or absent sensation may prevent early detection of injuries, burns, skin infections, or irritation.
Bone Fragility:
Extended immobility can weaken bones over time, increasing the risk of fractures and joint stiffness.
Early identification of the type and extent of paralysis supports an individualized care plan focused on long-term management and prevention of complications.
Common Symptoms of Paralysis
Loss of Muscle Function:
Sudden or gradual loss of the ability to move certain parts of the body due to impaired nerve or muscle function.
Inability to Move:
Partial or complete immobility in the affected area, depending on the extent of nerve involvement.
Numbness or Tingling:
Abnormal sensations such as numbness, tingling, or pins-and-needles in the affected region.
Loss of Sensation:
Reduced or absent ability to feel touch, temperature, or pain in the paralyzed area.
Muscle Weakness:
Decreased strength and endurance in affected muscles, which may worsen over time without appropriate care.
Muscle Stiffness or Floppiness:
Muscles may become stiff and tight (spastic) or loose and floppy (flaccid), depending on nerve damage.
Loss of Bladder or Bowel Control:
In more severe cases, paralysis may interfere with bladder or bowel regulation.
Difficulty Speaking or Swallowing:
Certain forms of paralysis can affect facial, throat, or tongue muscles, leading to speech or swallowing difficulties.
Additional Symptoms Based on Type or Cause
Facial Drooping:
Commonly observed in stroke-related paralysis or facial nerve involvement.
Slurred Speech:
May occur due to weakened or poorly coordinated speech muscles.
Loss of Coordination:
Difficulty maintaining balance or coordinating body movements.
One-Sided Weakness:
Frequently seen in hemiplegia, affecting one side of the body.
Full-Body Immobility:
Quadriplegia can result in loss of movement in all four limbs and, in some cases, the torso.
If these symptoms are sudden, progressive, or significantly affecting daily activities, timely medical evaluation is advised to identify the cause and guide appropriate management.
Paralysis Recovery-Friendly Diet Plan
Morning (Upon Waking)
Start with a glass of warm water with lemon or soaked fenugreek seeds to support digestion.
Optional: 5 soaked almonds and 1 walnut as a source of healthy fats.
Breakfast
Oats porridge with milk or plant-based milk, topped with chopped banana or berries.
Alternatively, 2 boiled eggs with whole-grain toast and fruit for balanced nutrition.
Herbal tea or green tea; excessive caffeine intake is best avoided.
Mid-Morning Snack
A small bowl of fresh fruit such as papaya, apple, or orange.
Alternatively, a glass of coconut water for hydration.
Lunch
Brown rice or whole-wheat chapati as a carbohydrate source.
Dal or lentils, or lean protein such as chicken, fish, or tofu.
Cooked vegetables like spinach, carrots, beetroot, and broccoli for micronutrient support.
Fresh salad with moderate use of olive oil.
Optional: Buttermilk or curd to support digestion, if tolerated.
Evening Snack
A handful of nuts or roasted chickpeas.
Green tea or warm milk with turmeric as part of an evening routine.
Alternatively, one slice of multigrain toast with peanut butter.
Dinner (Light and Nourishing)
Vegetable soup with lentils or a light protein source such as tofu or chicken.
Alternatively, 1–2 chapatis with lightly sautéed vegetables.
A small serving of quinoa or brown rice, based on appetite and activity level.
Optional: Warm milk before bedtime, if suitable.
Note: Dietary recommendations may vary based on the individual’s overall health status, mobility level, and associated medical conditions.
Daily Regimen for Paralysis Recovery
Morning
Wake up between 6:30–7:30 AM to maintain a consistent routine.
Gentle stretching or physiotherapy-guided exercises to support mobility.
Sun exposure for 10–15 minutes, as appropriate.
Meditation or deep-breathing exercises to promote relaxation and focus.
Daytime
Follow a balanced diet and maintain regular hydration.
Continue physiotherapy or guided movement exercises as advised.
Aim for approximately 2–2.5 liters of fluids daily, unless otherwise advised.
Engage in cognitive activities such as reading, listening to audiobooks, or simple puzzles.
Night
Keep dinner light and allow adequate time before sleep.
Maintain a regular sleep schedule to support overall recovery and well-being.
This diet and regimen are intended as supportive measures and should be adapted under professional guidance as part of an individualized care plan.
Yoga and Supportive Lifestyle Practices for Paralysis
These yoga practices are intended to provide supportive physical and mental benefits and should be performed only under guidance, based on individual mobility and medical condition. Yoga is not a replacement for medical or rehabilitative care, but may complement an overall recovery plan.
1. Tadasana (Mountain Pose)
Benefits: Improves posture, strengthens the legs, and supports balance.
How to Perform: Stand with feet together and arms at your sides. Lift the chest, engage the legs, and raise the arms overhead with palms facing each other. Hold for about 30 seconds with steady breathing.
Modifications: If standing is difficult, this pose may be performed seated on a chair, focusing on spinal alignment and gentle arm movement.
2. Setu Bandhasana (Bridge Pose)
Benefits: Strengthens the lower back, gluteal muscles, and legs, and supports circulation.
How to Perform: Lie on your back with knees bent and feet flat on the floor. Press the feet down and lift the hips gently. Hold for 15–30 seconds, then lower slowly.
Modifications: A cushion or block may be placed under the hips for additional support.
3. Baddha Konasana (Bound Angle Pose)
Benefits: Helps open the hips and groin, improves circulation, and stretches inner thighs.
How to Perform: Sit with legs extended, then bring the soles of the feet together and allow the knees to fall outward. Sit upright and hold for about 30 seconds with calm breathing.
Modifications: Cushions under the knees or back support against a wall may be used for comfort.
4. Viparita Karani (Legs-Up-The-Wall Pose)
Benefits: A restorative posture that supports circulation, reduces swelling, and relaxes the nervous system.
How to Perform: Lie on your back with legs placed gently against a wall and arms relaxed at the sides. Remain for 5–10 minutes.
Modifications: Legs may be elevated on cushions or bolsters if wall support is not possible.
5. Marjaryasana–Bitilasana (Cat–Cow Pose)
Benefits: Supports spinal flexibility, gentle strengthening, and coordination with breath.
How to Perform: Begin on all fours. Inhale to arch the back (cow pose) and exhale to round the spine (cat pose). Continue for 5–10 slow rounds.
Modifications: Can be adapted to a seated or lying position if weight-bearing is difficult.
6. Adho Mukha Svanasana (Downward-Facing Dog Pose)
Benefits: Encourages stretching of the legs, arms, and spine while supporting circulation.
How to Perform: From all fours, lift the hips upward, keeping the arms extended and spine lengthened. Hold for 15–30 seconds, then release gently.
Modifications: A chair-supported version may be used to reduce pressure and improve stability.
7. Savasana (Corpse Pose)
Benefits: Promotes deep relaxation, stress reduction, and mental calmness.
How to Perform: Lie comfortably on your back with arms relaxed and palms facing upward. Focus on slow, natural breathing for 5–10 minutes.
Modifications: Cushions may be placed under the head, knees, or back for support.
8. Trikonasana (Triangle Pose)
Benefits: Helps stretch the legs, hips, and spine, and supports balance.
How to Perform: Stand with legs apart, turn one foot outward, extend the arms, and gently lean to the side. Hold for 15–30 seconds, then repeat on the other side.
Modifications: A block or chair may be used for hand support.
9. Uttanasana (Standing Forward Bend Pose)
Benefits: Gently stretches the hamstrings and back and supports flexibility.
How to Perform: Stand with feet hip-width apart, bend forward from the hips, and allow the head and neck to relax. Hold briefly and return slowly.
Modifications: A seated forward bend may be performed instead.
10. Supta Baddha Konasana (Reclining Bound Angle Pose)
Benefits: Encourages hip opening and deep relaxation.
How to Perform: Lie on your back, bring the soles of the feet together, and allow the knees to fall outward. Remain for 5–10 minutes with relaxed breathing.
Modifications: Pillows or blankets may be placed under the knees for comfort.
Homeopathic Treatment Approach for Paralysis
Why Homeopathy?
Homeopathy is a system of care that focuses on understanding the underlying factors contributing to illness, rather than addressing symptoms alone. The approach aims to work with the body’s natural regulatory mechanisms and is generally considered well-tolerated when guided by a qualified professional. Care is tailored according to the individual’s physical condition, medical history, and overall health status.
Homeopathic care may be considered as part of a long-term management plan, especially in chronic or recovery-related conditions, alongside appropriate medical supervision.
Spiritual Homeopathy Clinic: Treatment Perspective
At Spiritual Homeopathy Clinic, care is centered on a detailed understanding of each patient’s condition. Paralysis is approached by considering factors such as the cause, duration, extent of nerve involvement, associated symptoms, and overall constitution. The focus remains on individualized care rather than a uniform treatment model.
Consultations are available across multiple branches in Hyderabad, as well as through online and international consultation options, making follow-up and continuity of care accessible for patients unable to attend in person.
Treatment Planning and Follow-Up
1. Comprehensive Case Evaluation
Each consultation includes a structured assessment of symptoms, functional limitations, medical history, and lifestyle factors. This helps in identifying contributing factors that may influence recovery and daily functioning.
2. Individualized Care Strategy
The homeopathic approach emphasizes personalization. Care plans are adapted over time based on response, changes in symptoms, and overall progress, supporting a gradual and monitored management process.
3. Ongoing Monitoring
Regular follow-ups are used to observe functional changes, address emerging concerns, and adjust the care plan as needed. This supports continuity and safe long-term management.
When to Consult a Doctor
You should consult a healthcare professional if you notice sudden weakness, loss of movement, or numbness in any part of your body. Early evaluation helps identify the underlying cause and supports timely management to prevent complications.
Seek consultation if you experience:
Sudden or progressive weakness in one or more limbs
Loss of coordination, balance, or difficulty walking
Numbness, tingling, or loss of sensation in any body part
Difficulty speaking, swallowing, or controlling bladder or bowel function
Muscle stiffness, spasms, or floppiness affecting daily activities
Symptoms that interfere with your independence or quality of life
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also offered for patients who cannot visit in person. A professional assessment allows for an individualized care plan tailored to your symptoms, mobility, and overall health.
For appointments or guidance, contact 9069 176 176.
Frequently Asked Questions (FAQ)
1. What is paralysis?
Paralysis is the loss of muscle function in part or all of the body, usually caused by nerve damage, spinal injury, or neurological disorders. It may affect movement, sensation, or both, and can be temporary or long-term depending on the underlying cause.
2. What are the main causes of paralysis?
Common causes include stroke, spinal cord injury, cerebral palsy, multiple sclerosis, tumors, neurodegenerative diseases (such as ALS), infections, and trauma to the brain or spinal cord.
3. What are the different types of paralysis?
Paralysis is classified into several types, including:
Monoplegia: Paralysis of one limb
Hemiplegia: Paralysis affecting one side of the body
Diplegia: Paralysis affecting similar parts on both sides of the body
Paraplegia: Paralysis of the lower half of the body, usually the legs
Quadriplegia: Paralysis affecting both arms and legs, and sometimes the torso
4. What are the symptoms of paralysis?
Symptoms vary based on severity and location and may include muscle weakness, inability to move or feel a body part, numbness, loss of coordination, difficulty breathing, or loss of bladder or bowel control. Medical consultation is advised if symptoms progress or interfere with daily function.
5. Can paralysis be treated?
Treatment focuses on management and supportive care. This may include physical therapy, occupational therapy, rehabilitation programs, medical interventions, and assistive devices. The approach depends on the cause and extent of nerve involvement.
6. Is paralysis reversible?
Reversibility depends on the underlying cause. Paralysis due to temporary nerve compression may improve, while paralysis caused by spinal cord injury or progressive neurological conditions may be long-term. Early evaluation and rehabilitation can support functional outcomes.
7. What is the difference between flaccid and spastic paralysis?
Flaccid paralysis: Characterized by limp muscles and reduced muscle tone, often due to damage to lower motor neurons
Spastic paralysis: Involves stiff or tight muscles with increased tone, commonly associated with brain or upper motor neuron involvement
8. Can paralysis affect the brain?
Yes. Paralysis may result from brain injuries, strokes, or neurological diseases. Depending on the affected area, it can influence movement, speech, coordination, or cognitive functions.
9. How can one cope with paralysis?
Coping may involve structured rehabilitation, physical and occupational therapy, adaptive equipment, psychological support, and social support systems. Emotional well-being is an important aspect of long-term management.
10. Is there a way to prevent paralysis?
Not all cases are preventable. However, reducing risk factors—such as practicing road safety, using protective gear, managing chronic conditions, and addressing stroke risk factors—may help lower the likelihood of certain causes.
11. What is the prognosis for someone with paralysis?
Prognosis varies depending on cause, severity, and location. Some individuals may experience partial improvement, while others may require long-term support. Ongoing rehabilitation and adaptive strategies play an important role in daily functioning.
12. Can people with paralysis lead normal lives?
Many individuals with paralysis lead active and meaningful lives with appropriate medical care, rehabilitation, adaptive tools, and social support tailored to their needs.
13. What role does physical therapy play in paralysis management?
Physical therapy supports mobility, muscle strength, flexibility, and prevention of secondary complications. It also helps improve independence and quality of life.
14. Can paralysis affect mental health?
Yes. Emotional challenges such as anxiety, depression, or stress may occur. Psychological counseling and support can be beneficial alongside physical rehabilitation.
15. Can yoga help with paralysis management?
Yoga may serve as a supportive practice to promote relaxation, flexibility, and circulation when adapted appropriately. It should be performed under guidance and does not replace medical or rehabilitative care.