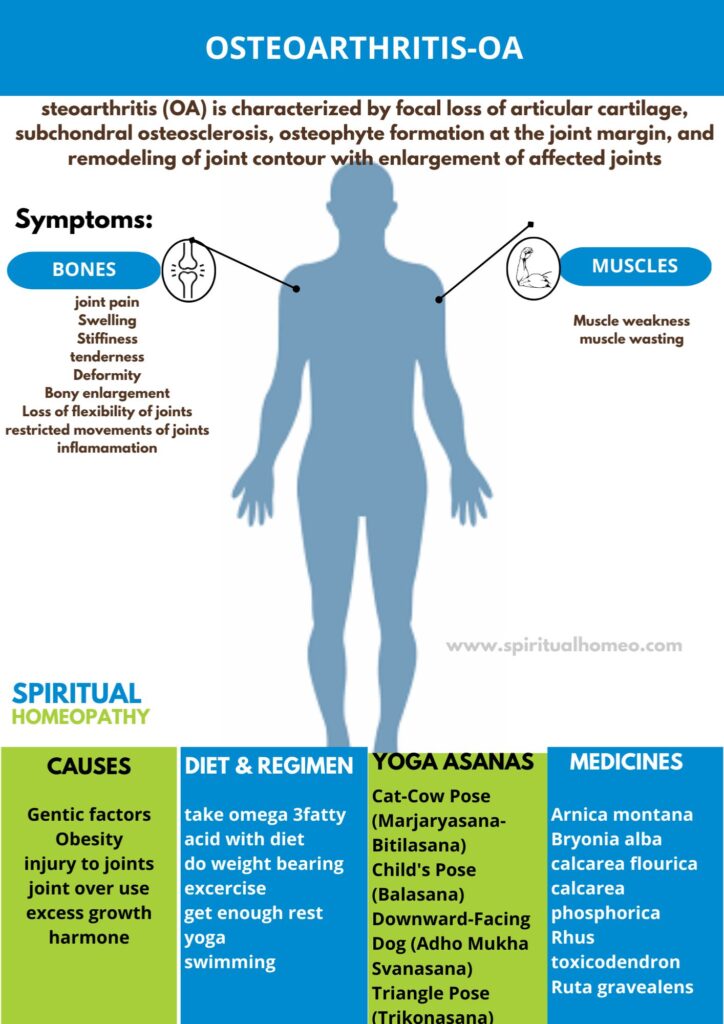
Osteoarthritis-OA
Osteoarthritis (OA) Guide: Relief, Remedies & Joint Care
- Home
- Osteoarthritis-OA
Osteoarthritis-OA
Effective Homeopathic Treatment for Osteoarthritis-OA
Osteoarthritis (OA) is a degenerative joint condition marked by the breakdown of articular cartilage, thickening of the underlying bone (subchondral sclerosis), bone spur formation (osteophytes), and changes in joint shape that often lead to joint enlargement and stiffness. This progressive wear-and-tear disease commonly affects the knees, hips, hands, and spine, causing pain, reduced mobility, and joint discomfort over time.
Everything You Need to Know
Overview
Osteoarthritis (OA) is a chronic degenerative joint disease that develops when the protective cartilage cushioning the ends of bones gradually wears away over time. This process can lead to joint pain, stiffness, swelling, and reduced mobility. OA most commonly affects weight-bearing joints such as the knees, hips, and spine. Aging, previous joint injuries, excess body weight, and genetic factors are known contributors to its onset and progression.
Causes of Osteoarthritis
The causes of osteoarthritis (OA) are multifactorial and usually develop gradually over time. Key contributing factors include:
Aging – Natural cartilage degeneration occurs with age, increasing the risk of osteoarthritis.
Joint Injuries – Previous injuries such as fractures, ligament tears, or joint trauma can damage cartilage and contribute to OA development.
Genetics – A family history of osteoarthritis may increase an individual’s susceptibility.
Obesity – Excess body weight places additional stress on weight-bearing joints, particularly the knees and hips.
Repetitive Joint Use – Long-term overuse from physical labor, repetitive movements, or certain sports can gradually wear down joint cartilage.
Gender – Women, especially after menopause, have a higher risk of developing osteoarthritis.
Joint Abnormalities – Congenital or structural joint variations may lead to early cartilage breakdown.
🦴 Types of Osteoarthritis (OA)
Osteoarthritis can affect different joints and may develop due to various causes. It is commonly classified into primary and secondary types, along with classification based on the specific joints involved.
1. Primary Osteoarthritis
This is the most common form of osteoarthritis and develops due to the natural aging process and gradual wear-and-tear of cartilage over time. It usually affects weight-bearing and frequently used joints such as:
Knees
Hips
Spine
Hands
2. Secondary Osteoarthritis
This form develops as a result of an underlying condition or external contributing factor. Possible causes include:
Previous joint injuries or trauma
Obesity
Genetic disorders
Inflammatory conditions such as rheumatoid arthritis
Metabolic disorders (e.g., hemochromatosis)
Joint-Specific Types of Osteoarthritis
3. Knee Osteoarthritis
One of the most common forms
Causes pain, stiffness, and swelling in one or both knees
Symptoms often worsen with activity or prolonged standing
4. Hip Osteoarthritis
Affects joint movement and overall mobility
Pain may radiate to the groin, thigh, or buttocks
May result in limping or difficulty walking
5. Spine Osteoarthritis (Spondylosis)
Involves the cervical or lumbar spine
Causes back pain, stiffness, and possible nerve irritation
In some cases, may contribute to spinal stenosis
6. Hand and Finger Osteoarthritis
Common in women, particularly after menopause
Affects finger joints and the base of the thumb
May cause stiffness, pain, and visible bony enlargements
7. Foot and Ankle Osteoarthritis
Often develops due to injury or long-term wear and tear
Commonly affects the big toe, midfoot, or ankle
May lead to swelling and difficulty while walking
🔍 Common Signs and Symptoms of Osteoarthritis (OA)
Osteoarthritis is a progressive joint disease that can affect daily activities and overall quality of life. Recognizing symptoms early may help with timely evaluation and appropriate management. The common signs and symptoms include:
1. Joint Pain
Persistent or aching pain in the affected joint, especially during or after physical activity. Pain may reduce with rest but often returns with continued use.
2. Joint Stiffness
Stiffness is commonly noticed in the morning or after long periods of inactivity and usually improves with gentle movement.
3. Swelling and Inflammation
The soft tissues around the joint may become swollen, leading to tenderness and discomfort.
4. Reduced Range of Motion
Difficulty moving the joint fully, which can affect daily activities such as walking, bending, or gripping objects.
5. Crepitus (Grinding Sensation)
A crackling, popping, or grating sensation during joint movement due to roughened cartilage surfaces.
6. Joint Deformities
In advanced stages, joints may appear enlarged or misshapen due to cartilage loss and bone spur formation.
7. Tenderness
The affected joint may feel sore or painful to touch, particularly during flare-ups.
Anti-Inflammatory Diet for Osteoarthritis
A diet rich in anti-inflammatory foods can play a supportive role in managing osteoarthritis (OA) symptoms. Below is an overview of beneficial food groups:
1. Omega-3 Fatty Acids
These healthy fats help support the body’s natural inflammatory balance.
Fatty Fish: Salmon, mackerel, sardines, and tuna
Plant-Based Options: Flaxseeds, chia seeds, and walnuts for vegetarian and vegan diets
2. Antioxidant-Rich Foods
Antioxidants help counter oxidative stress associated with joint discomfort.
Berries: Blueberries, strawberries, and raspberries
Leafy Greens: Kale, spinach, and Swiss chard
Cruciferous Vegetables: Broccoli, Brussels sprouts, and cabbage, which contain compounds linked to cartilage support
3. Whole Grains and Fiber
Fiber-rich foods may help with weight management and overall metabolic health.
Whole Grains: Brown rice, quinoa, and oats
Legumes: Beans, lentils, and peas for fiber and plant protein
4. Bone Health Nutrients
Important for maintaining bone and joint strength.
Calcium and Vitamin D: Dairy products, fortified plant-based milks, and eggs
Magnesium: Nuts, seeds, and leafy greens support bone health
5. Anti-Inflammatory Spices
Certain spices are traditionally used for their supportive properties.
Turmeric: Contains curcumin, studied for its role in inflammation modulation
Ginger: Commonly used as a natural anti-inflammatory ingredient in foods and teas
6. Healthy Fats
Including healthy fats may support joint and cardiovascular health.
Olive Oil: Contains oleocanthal, associated with anti-inflammatory activity
Nuts and Seeds: Almonds, walnuts, and flaxseeds provide beneficial fats and antioxidants
7. Hydration
Adequate hydration supports joint lubrication and overall health.
Water: Aim for regular intake throughout the day to maintain joint function
🏃♀️ Exercise Regimen for Osteoarthritis
Regular, appropriate physical activity is important for maintaining joint mobility and muscle strength in OA.
1. Weight-Bearing Exercises
These exercises help maintain bone density and strengthen supporting muscles.
Walking: Around 30 minutes, most days of the week
Cycling: Gentle on joints while improving leg strength
Hiking: Adds variety and functional strength
2. Strength Training
Strengthening muscles helps reduce stress on joints.
Resistance Bands: For major muscle groups
Light Weightlifting: Focus on controlled movements
Bodyweight Exercises: Modified exercises as tolerated
3. Low-Impact Cardio
Supports cardiovascular fitness with minimal joint strain.
Swimming: Full-body, joint-friendly exercise
Water Aerobics: Provides resistance with joint support
Elliptical Training: A low-impact alternative to running
4. Flexibility and Balance Exercises
Improve joint mobility and reduce fall risk.
Yoga: Gentle poses to enhance flexibility
Tai Chi: Slow, controlled movements for balance
Stretching: Regular stretches to support joint range of motion
5. Rest and Recovery
Adequate rest is essential to avoid joint overuse.
Avoid Overexertion: Modify activity based on symptoms
Cold and Heat Therapy: Cold for inflammation; heat for muscle relaxation
Sleep: Aim for 7–9 hours of quality sleep nightly
🧘♀️ Yoga and Lifestyle Support for Osteoarthritis
Yoga practices may help support flexibility, posture, and overall joint comfort in individuals with osteoarthritis. These practices are intended as supportive measures and should be adapted based on comfort and joint involvement.
1. Sukhasana (Easy Pose)
A simple seated posture that helps improve posture, reduce stress, and enhance hip flexibility.
How to do it:
Sit on the floor with legs crossed comfortably
Keep your back straight and shoulders relaxed
Place your hands on your knees, palms facing up
Close your eyes and focus on slow, steady breathing
Benefits:
Gently stretches the hips and lower back
Promotes relaxation and stress reduction
2. Bhujangasana (Cobra Pose)
A gentle backbend that supports spinal strength and chest opening, often used to ease lower back stiffness.
How to do it:
Lie face down with palms under your shoulders
Inhale and slowly lift your chest, using your arms for support
Keep elbows slightly bent and shoulders relaxed
Hold for 15–30 seconds and release gently
Benefits:
Supports spinal strength
Helps reduce lower back stiffness
3. Adho Mukha Svanasana (Downward-Facing Dog)
This pose stretches and strengthens multiple muscle groups, supporting overall joint mobility.
How to do it:
Begin on hands and knees, wrists under shoulders, knees under hips
Lift hips toward the ceiling, forming an inverted “V”
Keep knees slightly bent if needed and press heels gently downward
Benefits:
Improves flexibility in hips, legs, and spine
Reduces tension in the back and shoulders
4. Setu Bandhasana (Bridge Pose)
A strengthening and stretching posture that supports the hips, legs, and lower back.
How to do it:
Lie on your back with knees bent and feet hip-width apart
Press feet into the floor and lift hips upward
Keep shoulders grounded and hold for 15–30 seconds
Benefits:
Strengthens glutes, hamstrings, and lower back
Helps reduce hip and back stiffness
5. Virabhadrasana II (Warrior II Pose)
A standing pose that strengthens the lower body and improves balance.
How to do it:
Stand with legs wide apart
Turn one foot outward and bend that knee
Extend arms parallel to the floor and hold for 30 seconds
Benefits:
Strengthens legs and hips
Improves balance and joint stability
6. Anjaneyasana (Low Lunge Pose)
This pose targets the hips, thighs, and lower back.
How to do it:
Step one foot back and lower the knee to the floor
Keep front knee aligned over the ankle
Lift the torso and extend arms overhead
Benefits:
Stretches hips and thighs
Supports flexibility and leg strength
7. Marjaryasana / Bitilasana (Cat–Cow Pose)
A gentle flowing sequence that supports spinal mobility.
How to do it:
Begin on hands and knees
Inhale into Cow Pose, exhale into Cat Pose
Continue for 5–10 slow rounds
Benefits:
Improves spinal flexibility
Relieves tension in the back, neck, and shoulders
8. Viparita Karani (Legs Up the Wall Pose)
A restorative posture that promotes relaxation and circulation.
How to do it:
Lie on your back with legs extended up against a wall
Relax arms by your sides and breathe deeply
Stay for 5–10 minutes
Benefits:
Helps reduce lower body stiffness
Supports circulation in the legs
9. Balasana (Child’s Pose)
A gentle resting pose that supports relaxation.
How to do it:
Kneel and sit back on your heels
Extend arms forward and lower forehead toward the floor
Breathe deeply and relax
Benefits:
Gently stretches the back and hips
Calms the mind and reduces tension
10. Savasana (Corpse Pose)
A relaxation pose used to promote rest and mindfulness.
How to do it:
Lie flat on your back with arms at your sides
Close your eyes and focus on natural breathing
Remain for 5–10 minutes
Benefits:
Encourages relaxation and mental clarity
Helps reduce stress and fatigue
🌿 Why Choose Homeopathy?
Homeopathy is a system of complementary medicine that focuses on understanding the underlying factors contributing to illness, rather than addressing symptoms alone. It works alongside the body’s natural regulatory processes and is commonly used as part of long-term health management under professional guidance.
Homeopathic care is individualized, meaning treatment plans are adapted to a person’s symptoms, health history, and overall constitution. This approach is used for both acute concerns and chronic conditions, depending on individual needs and clinical assessment.
🌟 Spiritual Homeopathy Clinic: Patient-Focused Care
At Spiritual Homeopathy Clinic, care is centered on a comprehensive understanding of physical, emotional, and lifestyle factors that may influence health. Consultations are conducted by qualified homeopathy practitioners with clinical experience across a range of conditions.
The clinic operates across multiple branches in Hyderabad and also provides online and international consultations, allowing patients to access care based on their location and convenience.
💫 Approach to Care at Spiritual Homeopathy Clinic
The clinical approach is based on classical homeopathic principles combined with systematic case evaluation. Key aspects include:
Individualized Care: Each case is assessed separately, with treatment plans tailored to the patient’s overall health profile.
Focus on Contributing Factors: Attention is given to possible triggers, lifestyle influences, and long-standing patterns.
Professional Guidance: Care is provided under qualified supervision, with regular monitoring and follow-up.
Supportive & Integrative Care: Homeopathy may be used alongside appropriate medical advice when required.
🔍 Our Treatment Process
🩺 1. Detailed Consultation
The consultation involves a structured discussion of medical history, current symptoms, lifestyle patterns, and emotional well-being. This helps in forming a clear clinical picture and planning individualized care.
Consultations are available in-clinic at Hyderabad branches, as well as through online and international consultation modes.
🔄 2. Ongoing Assessment and Follow-Up
Follow-up consultations are used to observe symptom changes, overall response, and general well-being. Adjustments are made based on clinical evaluation, ensuring care remains aligned with the patient’s progress.
❤️ Commitment to Patient Care
Spiritual Homeopathy Clinic emphasizes responsible, patient-centered care. The goal is to support symptom management, improve functional well-being, and address contributing factors through a structured and individualized approach.
When to Consult
You should consult a healthcare professional if osteoarthritis (OA) symptoms become frequent, persistent, or begin to interfere with daily activities, mobility, or sleep. Early evaluation helps identify contributing factors, assess joint involvement, and reduce the risk of further joint damage.
Seek consultation if you experience:
Recurrent or long-lasting joint pain
Difficulty or pain while moving joints, walking, or climbing stairs
Persistent joint stiffness, swelling, or discomfort
Symptoms that worsen after activity or disturb sleep
Reduced joint flexibility or difficulty performing daily tasks
Symptoms not improving with routine lifestyle measures or exercise
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for individuals who are unable to visit in person. A professional assessment supports an individualized care approach based on symptoms, joint involvement, and overall health status.
For appointments or guidance, contact 9069 176 176.
FAQ
1. What is Osteoarthritis (OA)?
Osteoarthritis (OA) is a degenerative joint disease where the cartilage that cushions the joints breaks down over time. This leads to pain, swelling, and reduced movement in the affected joints. OA commonly affects the knees, hips, hands, and spine.
2. What causes Osteoarthritis?
OA occurs when the cartilage in the joints deteriorates, which leads to bones rubbing against each other. The exact cause can vary, but common risk factors include:
Aging: Cartilage naturally wears down over time.
Injury or trauma: Previous joint injuries can increase the risk of OA.
Genetics: Family history can play a role.
Obesity: Extra weight puts additional stress on weight-bearing joints.
Repetitive stress: Activities or jobs that put repeated strain on joints can contribute to OA.
3. What are the symptoms of Osteoarthritis?
Symptoms of OA can vary but typically include:
Joint pain: A deep, aching pain that worsens with activity.
Stiffness: Especially after periods of inactivity, such as waking up in the morning.
Swelling: Joint areas may become swollen or tender.
Reduced flexibility: Difficulty moving the joint through its full range of motion.
Cracking or popping sounds: Known as crepitus, when moving the joint.
4. Which joints are most affected by Osteoarthritis?
OA can affect almost any joint in the body, but the most commonly affected joints include:
Knees
Hips
Hands (especially the fingers)
Spine (lower back and neck)
Feet (especially the big toe)
5. How is Osteoarthritis diagnosed?
Diagnosis of OA usually involves:
Medical History: A doctor will ask about your symptoms, lifestyle, and family history.
Physical Examination: The doctor will examine your joints for signs of swelling, tenderness, and limited movement.
X-rays: These can help identify changes in the joint, such as cartilage loss or bone spurs.
MRI: In some cases, an MRI may be used to get a more detailed image of the joint’s cartilage and soft tissues.
Blood Tests: Although not typically used to diagnose OA, blood tests may rule out other conditions like rheumatoid arthritis.
6. Can Osteoarthritis be cured?
Currently, there is no cure for osteoarthritis. However, there are treatments available that can help manage symptoms, reduce pain, and improve joint function. Treatment plans often include a combination of medications, lifestyle changes, physical therapy, and in some cases, surgery.
7. What are the treatment options for Osteoarthritis?
Treatment for OA aims to relieve symptoms and improve joint function. Common options include:
Medications:
Over-the-counter pain relievers like acetaminophen or NSAIDs (ibuprofen, naproxen) for pain relief.
Topical creams or patches to soothe joint pain.
Prescription medications for more severe pain.
Physical Therapy: Exercises to strengthen muscles around the joints and improve flexibility.
Lifestyle Changes:
Weight management to reduce pressure on affected joints.
Joint protection techniques and ergonomic adjustments.
Surgical Options: In severe cases, joint replacement surgery (e.g., knee or hip replacement) may be considered.
8. How can exercise help with Osteoarthritis?
Exercise is one of the best ways to manage OA symptoms. Regular, low-impact exercise can:
Strengthen muscles around the affected joints, helping to reduce strain on the joint.
Improve flexibility and joint range of motion.
Reduce stiffness and improve overall joint function.
Aid in weight management, which can relieve pressure on weight-bearing joints like the knees and hips.
Low-impact activities such as swimming, cycling, walking, and yoga are particularly beneficial for OA sufferers.
9. Can I manage Osteoarthritis through diet?
Yes, a healthy diet can help reduce inflammation, manage weight, and support joint health. Key dietary tips include:
Anti-inflammatory foods: Omega-3 fatty acids (found in fatty fish and flaxseeds), antioxidants (found in berries, leafy greens), and healthy fats (like olive oil) can help reduce inflammation.
Maintain a healthy weight: Reducing excess weight can take pressure off your joints, especially in the knees and hips.
Supplements: Some people find relief from supplements like glucosamine and chondroitin, though research on their effectiveness is mixed. Always consult your doctor before starting any supplements.
10. When should I see a doctor for Osteoarthritis?
It’s important to see a doctor if:
You experience significant pain or swelling in your joints.
You notice reduced range of motion or difficulty performing daily tasks.
Your symptoms interfere with your quality of life or ability to work.
Your pain doesn’t improve with home treatments or lifestyle changes.
A healthcare provider can help assess the severity of your condition and recommend the appropriate treatments.
11. Can stress make Osteoarthritis worse?
Yes, stress can exacerbate the symptoms of osteoarthritis. Stress can lead to muscle tension, which increases joint pain and stiffness. Additionally, emotional stress can affect how the body responds to pain. Practices like mindfulness, relaxation techniques, and regular physical activity can help manage stress and its impact on OA.
12. Is surgery necessary for Osteoarthritis?
Surgery is typically reserved for severe cases of OA when other treatments have not provided relief. Some surgical options include:
Arthroscopy: A minimally invasive procedure to clean out debris or smooth rough cartilage.
Joint replacement: In cases where the joint is severely damaged, a full joint replacement (e.g., hip or knee replacement) may be recommended.