Obsessive Compulsive Disorder
Complete Guide to Obsessive-Compulsive Disorder (OCD): Symptoms, Causes, and Effective Treatments
- Home
- Obsessive Compulsive Disorder
Obsessive Compulsive Disorder
Effective Homeopathic Treatment for Obsessive Compulsive Disorder
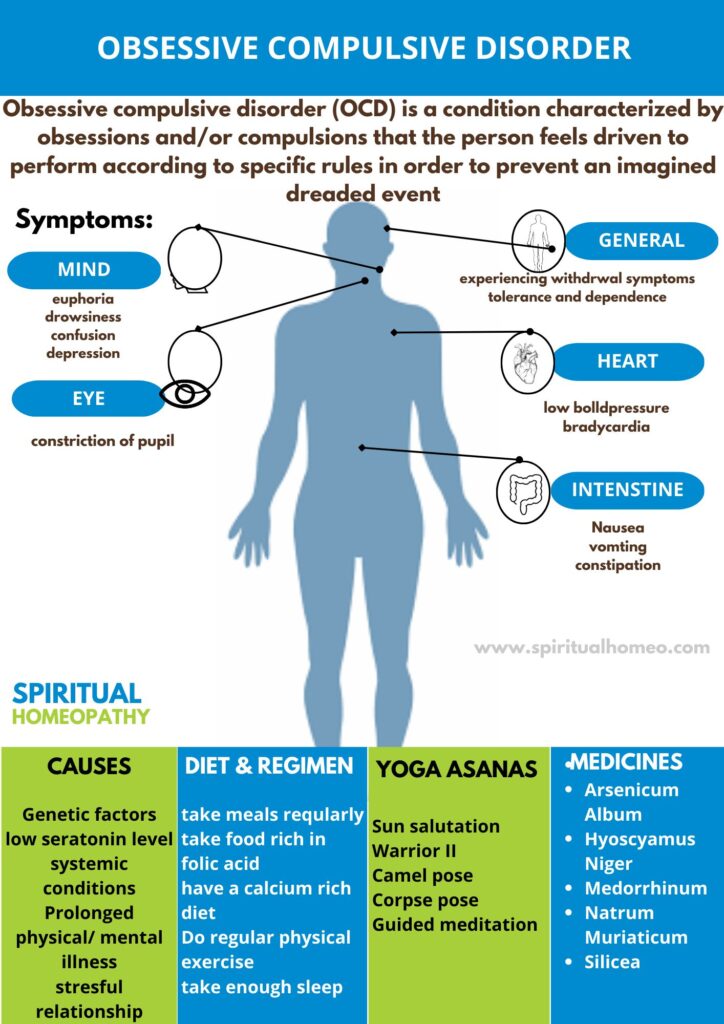
Obsessive-Compulsive Disorder (OCD) is a mental health condition marked by persistent obsessions and compulsions. Individuals with OCD feel compelled to follow specific rituals or rules to prevent feared, often imagined, events from occurring.
Everything You Need to Know
Overview
What Are Obsessions?
Obsessions are recurrent, unwanted thoughts or images that repeatedly enter the mind, despite attempts to dismiss them. These thoughts are intrusive and often cause significant mental distress.
Key features of an obsession include:
Intrusive nature: The thoughts, impulses, or images invade the conscious mind and may interfere with daily functioning.
Ego-alien: The individual recognizes the obsession as irrational and foreign to their own personality but feels unable to control it.
Insight present: People with obsessive-compulsive disorder (OCD) are usually aware that their thoughts are unreasonable.
Resistance is difficult: Attempts to resist the obsession often increase anxiety and emotional discomfort.
Consultation with a healthcare professional can help assess symptom patterns and guide appropriate care. Consultations are available at Spiritual Homeopathy Clinic across multiple branches in Hyderabad, as well as through online and international modes.
What Are Compulsions?
Compulsions are repetitive behaviors or mental acts performed to reduce or neutralize the anxiety caused by obsessive thoughts. These actions are not experienced as pleasurable but are carried out to relieve distress.
Characteristics of compulsions include:
Behavioral response to obsession: Compulsions usually follow obsessive thoughts and are performed to manage fear or anxiety.
Irrational or excessive: The behavior is often disproportionate to the actual situation.
Subjective compulsion: Individuals experience a strong internal urge to perform the act, even while recognizing its irrational nature.
Temporary anxiety reduction: Performing the compulsion may bring short-term relief, but the cycle often repeats.
OCD in India vs. Other Countries
Studies indicate that OCD appears more frequently among unmarried males in India, whereas international data does not consistently show gender-based differences. The condition is also reported more commonly among individuals from higher social strata and those with above-average intelligence. These observations highlight the influence of cultural, social, and environmental factors.
Age of Onset
In India, the average age of onset for OCD is commonly in the late 20s (late third decade of life). In contrast, individuals in Western countries often experience the onset of symptoms at a younger age. Early recognition supports better long-term management.
Long-Term Outlook for OCD
Long-term studies on OCD suggest varying outcomes:
25% of individuals may show little or no improvement over time.
50% experience moderate to marked improvement with appropriate care.
25% may achieve complete recovery.
Outcomes depend on symptom severity, duration, and timely professional support.
Key Takeaways
OCD involves persistent obsessions that cause distress and often lead to compulsive behaviors aimed at reducing anxiety.
Insight into the irrational nature of these thoughts and actions is usually present, yet individuals feel compelled to act.
The condition shows variations in prevalence and age of onset across different populations.
With structured and individualized care, many individuals experience meaningful improvement over time.
Genetics, Neurobiological Factors, and Psychological Causes of Obsessive-Compulsive Disorder (OCD)
Obsessive-Compulsive Disorder (OCD) is a complex condition with multiple contributing factors, including genetic, neurobiological, autoimmune, and psychological influences. Understanding these mechanisms provides insight into how OCD develops and why symptom patterns vary between individuals.
Genetics and Family History of OCD
Research indicates that the lifetime risk of developing OCD increases nearly tenfold in first-degree relatives, such as parents or siblings, of individuals diagnosed with the disorder. This finding suggests a genetic predisposition to OCD, although it remains unclear how much of this risk is due to inherited genes versus shared family environments.
While large-scale twin and adoption studies are still required for definitive conclusions, family history is considered an important contributing factor. Individuals with a close family member affected by OCD may have a higher likelihood of developing symptoms.
Understanding genetic susceptibility helps guide an individualized care approach based on personal and family history.
Neurobiological Mechanisms in OCD
OCD has been associated with abnormalities in brain structure, function, and neurotransmitter regulation.
Structural Brain Abnormalities
Studies suggest that individuals with OCD may show subtle structural changes in brain regions involved in behavioral control. Parents of individuals with OCD have also been found to exhibit a higher rate of minor, non-localizing neurological signs, although no specific brain lesions have been consistently identified.
Brain Imaging Findings
Neuroimaging techniques such as Positron Emission Tomography (PET) and functional MRI (fMRI) have demonstrated increased activity in specific brain regions, including:
The frontal lobes
The caudate nucleus
The cingulum
These areas are involved in decision-making, impulse regulation, and behavioral control, all of which are relevant to obsessive and compulsive symptoms.
Neurotransmitter Dysregulation
Research has shown that serotonin (5HT) pathways play a significant role in OCD. Evidence supporting this includes increased anxiety responses during serotonin challenge studies, suggesting altered serotonin regulation in affected individuals.
Dopamine pathways may also contribute to OCD. Conditions involving the basal ganglia, such as Tourette’s syndrome or post-encephalitic parkinsonism, are often associated with obsessive symptoms, indicating a possible link between dopamine dysregulation and OCD.
Autoimmune Factors in OCD
Autoimmune mechanisms have been linked to OCD in certain cases. For example, individuals with Sydenham’s chorea, an autoimmune condition affecting the basal ganglia, frequently develop obsessive-compulsive symptoms. Research has identified autoantibodies targeting the caudate nucleus in many of these patients.
More recently, associations have been observed between Group A streptococcal infections and the onset of OCD or tic disorders in some individuals, suggesting that immune responses triggered by infections may play a role in symptom development.
The Role of Early Experiences in OCD
Early life experiences may influence the development of obsessive traits. Children raised by caregivers with pronounced obsessional behaviors may adopt similar patterns through social learning, particularly in environments marked by anxiety or heightened control.
Psychological and Behavioral Causes of OCD
From a psychological perspective, OCD is often understood as a learned or conditioned response to anxiety-provoking thoughts or situations.
Conditioned Response
When an individual experiences anxiety, compulsive behaviors may develop as a way to reduce distress. Although these behaviors provide temporary relief, they reinforce the cycle of obsession and compulsion over time.
Psychoanalytic Perspective
According to Sigmund Freud’s psychoanalytic theory, OCD symptoms arise from unresolved internal conflicts, often associated with distressing impulses. These conflicts generate anxiety, which may be managed through defense mechanisms such as compulsive behaviors.
Recognizing the psychological and behavioral contributors to OCD supports long-term management through individualized and comprehensive care.
Types of Obsessive-Compulsive Disorder (OCD): Understanding the Various Forms and Symptoms
Obsessive-Compulsive Disorder (OCD) can present in different forms, depending on the nature of the obsessions (persistent, intrusive thoughts) and compulsions (repetitive behaviors or mental actions) experienced by an individual. Symptoms may be episodic or long-standing, and their intensity can vary over time. OCD is commonly categorized based on the predominant patterns of obsessions and compulsions involved.
Understanding the specific type of OCD helps guide individualized care and long-term management.
1. Contamination OCD
Contamination OCD is one of the most commonly recognized forms of OCD. Individuals experience intense fears related to germs, dirt, or harmful substances, often leading to repetitive cleaning behaviors.
Common Obsessions:
Fear of germs, bacteria, illness, or becoming contaminated.
Common Compulsions:
Excessive handwashing, cleaning objects repeatedly, or avoiding places or people perceived as unclean.
2. Checking OCD
Checking OCD involves persistent fears that harm or danger may occur unless certain actions are checked repeatedly. These behaviors are driven by anxiety rather than actual risk.
Common Obsessions:
Fear of harm, danger, or making mistakes, such as forgetting to lock doors or turn off appliances.
Common Compulsions:
Repeatedly checking locks, switches, appliances, or scanning surroundings for potential hazards.
3. Symmetry / Ordering OCD
This type of OCD is characterized by a strong need for symmetry, exactness, or order. Individuals may feel significant discomfort if things are not arranged in a specific way.
Common Obsessions:
A need for things to be aligned, balanced, or arranged according to specific rules.
Common Compulsions:
Repeatedly arranging, organizing, or adjusting items until they feel “just right.”
4. Hoarding OCD
In Hoarding OCD, individuals feel compelled to save items due to fear of losing something important or being unprepared in the future. This can result in excessive clutter and functional difficulties.
Common Obsessions:
Fear of discarding items that may be needed later or have perceived importance.
Common Compulsions:
Collecting, saving, or avoiding discarding items, even when they are no longer useful.
5. Intrusive Thoughts OCD (Pure O)
Intrusive Thoughts OCD, often referred to as “Pure O,” involves distressing thoughts or images without obvious outward compulsions. Mental rituals are commonly used to reduce anxiety.
Common Obsessions:
Unwanted violent thoughts, fears of causing harm, disturbing images, or thoughts that conflict with personal values.
Common Compulsions:
Mental rituals such as silent repetition of words, counting, or mentally neutralizing distressing thoughts.
6. Religious or Moral OCD (Scrupulosity)
Scrupulosity involves obsessive concerns related to religious, spiritual, or moral beliefs. Individuals may feel excessive guilt or fear about wrongdoing.
Common Obsessions:
Fear of sin, blasphemy, or failing to meet moral or religious standards.
Common Compulsions:
Repeated prayers, excessive confession, reassurance-seeking, or ritualistic behaviors to feel morally acceptable.
7. Harm OCD
Harm OCD is characterized by intrusive fears about harming oneself or others, despite having no intention to act on these thoughts.
Common Obsessions:
Fear of losing control, acting violently, or unintentionally harming others.
Common Compulsions:
Avoiding sharp objects or certain situations, mental reassurance, or repeated checking behaviors.
8. Sexual OCD
Sexual OCD involves intrusive and unwanted sexual thoughts that are distressing and inconsistent with the individual’s values.
Common Obsessions:
Intrusive sexual thoughts involving inappropriate or taboo content.
Common Compulsions:
Mental checking, reassurance-seeking, or avoiding situations that trigger the thoughts.
9. Relationship OCD (ROCD)
Relationship OCD focuses on persistent doubts about romantic relationships. These doubts may cause anxiety and repeated reassurance-seeking.
Common Obsessions:
Questioning feelings toward a partner, doubts about relationship quality, or fear that the relationship is flawed.
Common Compulsions:
Seeking reassurance, mentally reviewing interactions, or comparing relationships with others.
10. Body Dysmorphic Disorder (BDD) – Related to OCD
Body Dysmorphic Disorder is closely related to OCD and involves excessive preoccupation with perceived physical flaws that may not be noticeable to others.
Common Obsessions:
Fear of being unattractive or physically defective despite reassurance.
Common Compulsions:
Excessive grooming, mirror checking, comparing appearance, or avoiding social situations.
Obsessions in OCD
Obsessions are persistent and intrusive thoughts, images, or impulses that forcibly enter the patient’s mind and often cause significant distress. These thoughts are unwanted, unpleasant, or disturbing, and the individual usually makes repeated attempts to resist or suppress them. Despite this, the obsessions continue to recur and interfere with normal functioning.
Common forms of obsessions include:
Obsessive Thoughts:
These may involve single words, phrases, or rhymes that are unpleasant, obscene, or blasphemous in nature and cause marked emotional distress.
Obsessive Images:
Vivid and disturbing mental images, often related to violence or abnormal sexual content, which the individual finds repulsive or anxiety-provoking.
Obsessive Ruminations:
Repetitive internal debates or arguments that the individual feels compelled to review continuously, leading to prolonged and exhausting thought cycles.
Obsessive Doubts:
Persistent uncertainty about whether actions were performed adequately, such as locking doors or completing routine tasks, or fears of unintentionally causing harm.
Obsessive Impulses:
Sudden and distressing urges to perform irrational or socially inappropriate acts, such as shouting inappropriate words or jumping into danger. These impulses are usually resisted but create intense internal conflict and anxiety.
If obsessions become frequent, severe, or interfere with daily life, professional evaluation is advised.
Compulsions in OCD
Compulsions are repetitive behaviors or mental acts performed in response to an obsession or according to rigid internal rules. These actions are intended to reduce anxiety or prevent a feared outcome, even though they are often excessive or not realistically connected to the situation.
Key features include:
Obsessive Rituals:
These may involve repetitive behaviors such as excessive handwashing, repeated checking, or mental rituals like counting or silently repeating words. Although performing the ritual may bring temporary relief, uncertainty often returns, leading to repeated cycles.
Awareness of Illogical Behavior:
Most individuals with OCD recognize that their compulsive behaviors are illogical or excessive. However, they feel driven to perform them and may attempt to conceal these behaviors due to embarrassment or fear of judgment.
Co-occurring Symptoms in OCD
Along with obsessions and compulsions, individuals with OCD may experience additional psychological symptoms that contribute to overall distress:
Anxiety and Depression:
OCD commonly coexists with anxiety and depressive symptoms. In some individuals, these emotional difficulties arise directly from persistent obsessive thoughts, while in others they may develop independently.
Depersonalization:
Some individuals experience feelings of detachment from themselves or their surroundings, which can increase discomfort and affect daily functioning.
A comprehensive assessment helps identify co-occurring symptoms and supports an individualized care approach.
Dietary Tips to Manage OCD Symptoms
A well-balanced diet plays an essential role in supporting brain function, regulating mood, and reducing stress. Appropriate dietary habits may help support overall mental well-being in individuals with OCD.
1. Nutrient-Rich Foods for Mental Health
Omega-3 Fatty Acids:
These healthy fats are important for brain health and mood regulation. They may also help reduce anxiety and low mood, which are commonly associated with OCD.
Sources: Fatty fish (salmon, mackerel, sardines), walnuts, flaxseeds, chia seeds.
Magnesium:
Magnesium supports nervous system relaxation and may help in managing stress and anxiety levels.
Sources: Dark leafy greens (spinach, kale), almonds, pumpkin seeds, avocados, bananas.
B Vitamins:
These vitamins are essential for neurotransmitter production involved in mood regulation and cognitive function. Low levels may contribute to irritability and anxiety.
Sources: Whole grains, eggs, leafy greens, legumes, beans.
Antioxidants:
Antioxidants help reduce oxidative stress and inflammation, which may support mental clarity and emotional balance.
Sources: Berries, nuts, seeds, dark leafy greens, and colorful vegetables.
Probiotics:
A healthy gut microbiome is linked with mental well-being. Probiotic-rich foods may support gut–brain balance and stress regulation.
Sources: Yogurt with live cultures, kefir, kimchi, sauerkraut.
Vitamin D:
Vitamin D plays a role in mental health and emotional regulation.
Sources: Fatty fish, egg yolks, fortified dairy products, and safe sunlight exposure.
2. Foods to Avoid
Caffeine:
May increase anxiety and intensify obsessive thoughts in some individuals.
Sugar:
Excessive sugar intake can cause fluctuations in blood sugar levels, potentially affecting mood and anxiety.
Processed Foods:
Foods high in artificial additives and preservatives may negatively affect overall mental health.
Alcohol:
Alcohol can disrupt sleep and emotional regulation, potentially worsening OCD-related symptoms.
3. Hydration
Adequate hydration supports brain function and overall well-being. Drinking sufficient water throughout the day may help maintain focus and emotional balance.
Regimen for Managing OCD Symptoms
Along with dietary measures, a structured daily regimen plays an important role in managing OCD symptoms. A combination of professional care and self-care practices may support long-term symptom management.
1. Cognitive Behavioral Therapy (CBT) & Exposure and Response Prevention (ERP)
CBT helps individuals recognize and challenge maladaptive thought patterns associated with OCD.
ERP, a structured component of CBT, involves gradual exposure to anxiety-provoking situations while resisting compulsive responses, helping reduce symptom intensity over time.
2. Medical Management (Under Professional Supervision)
In some cases, medical management may be advised by a qualified healthcare professional, depending on symptom severity and individual needs. Any such approach should be carefully monitored.
3. Mindfulness and Stress Management
Mindfulness practices, deep breathing exercises, and relaxation techniques can help individuals respond to obsessive thoughts with greater awareness and reduced emotional reactivity.
4. Regular Exercise
Physical activity supports emotional regulation by reducing stress and improving mood. Moderate exercise for about 30 minutes, several times a week, may be beneficial.
5. Sleep Hygiene
Adequate and consistent sleep is essential for mental well-being. Helpful practices include:
Maintaining regular sleep and wake times
Limiting screen exposure before bedtime
Establishing a calming bedtime routine
6. Time Management
A structured daily schedule can help reduce uncertainty and stress, which are common triggers for OCD symptoms.
7. Social Support
Support from family, friends, or support groups can reduce isolation and provide emotional reassurance.
8. Limiting Triggers
Identifying personal triggers and creating a supportive environment may help reduce symptom flare-ups, even though complete avoidance is not always possible.
9. Journaling
Writing down thoughts, triggers, and emotional responses can help identify patterns and support self-awareness over time.
Yoga and Lifestyle Practices for OCD Support
Yoga and breathing practices may support relaxation, stress regulation, and mind–body awareness in individuals with OCD. These practices are intended as supportive measures and should be used alongside professional medical or psychological care, not as a replacement.
1. Sukhasana (Easy Pose)
Benefits:
Sukhasana is a seated meditation pose that promotes relaxation and helps focus the mind. It supports calming of the nervous system and may assist in managing anxiety and mental restlessness.
How to do it:
Sit on the floor with your legs crossed comfortably.
Keep your spine straight, shoulders relaxed, and hands resting on your knees.
Focus on your breath, inhaling deeply and exhaling slowly.
Remain in this position for 5–10 minutes, maintaining gentle awareness of breathing.
2. Adho Mukha Svanasana (Downward-Facing Dog)
Benefits:
This posture helps reduce stress, improves circulation, and promotes a sense of relaxation. It may assist in releasing physical tension that can accompany anxiety.
How to do it:
Begin in a tabletop position on your hands and knees.
Lift your hips upward and backward, forming an inverted V shape.
Keep hands shoulder-width apart and feet hip-width apart.
Relax the head and neck, breathing steadily.
Hold for 30 seconds to 1 minute.
3. Tadasana (Mountain Pose)
Benefits:
Tadasana supports posture, balance, and mental grounding. It may help improve focus and body awareness in individuals experiencing repetitive or intrusive thoughts.
How to do it:
Stand with feet together and arms by your sides.
Distribute weight evenly across both feet.
Lengthen the spine and lift the chest gently.
Raise arms overhead with palms facing each other.
Hold for about 30 seconds while breathing calmly.
4. Balasana (Child’s Pose)
Benefits:
Balasana is a restorative posture that promotes mental calmness and relaxation. It gently stretches the back and hips while encouraging restful breathing.
How to do it:
Start on hands and knees.
Bring big toes together and separate the knees slightly.
Sit back toward the heels, extending arms forward.
Rest the forehead on the mat.
Remain for 1–2 minutes with slow, deep breathing.
5. Setu Bandhasana (Bridge Pose)
Benefits:
Bridge Pose may help relieve stress and physical tension. It supports chest opening and encourages steady breathing, which can assist emotional regulation.
How to do it:
Lie on your back with knees bent and feet flat on the floor.
Press feet into the ground and lift hips gently.
Keep arms by your sides.
Hold for 20–30 seconds, then lower slowly.
Repeat 2–3 times as comfortable.
6. Viparita Karani (Legs-Up-The-Wall Pose)
Benefits:
This restorative posture helps calm the nervous system and promote relaxation. It may be useful during periods of heightened mental stress.
How to do it:
Sit sideways near a wall and gently swing legs upward while lying back.
Rest arms comfortably with palms facing upward.
Relax the neck and shoulders.
Hold for 5–10 minutes with steady breathing.
7. Pranayama (Breathing Techniques)
Benefits:
Controlled breathing practices support relaxation and mental clarity. They may help reduce the intensity of anxious or repetitive thoughts.
How to do it:
Sit comfortably with the spine upright.
Close your eyes and begin slow, deep breathing.
Practice alternate nostril breathing with gentle awareness.
Continue for 5–10 minutes without strain.
8. Utkatasana (Chair Pose)
Benefits:
Chair Pose supports physical strength and balance while encouraging mental focus and discipline. It may help improve body awareness.
How to do it:
Stand with feet together and raise arms overhead.
Bend knees as if sitting back into a chair.
Keep chest lifted and breathe steadily.
Hold for 20–30 seconds.
9. Savasana (Corpse Pose)
Benefits:
Savasana promotes deep relaxation and helps integrate the effects of yoga practice. It supports mental calmness and physical rest.
How to do it:
Lie flat on your back with arms relaxed by your sides.
Close your eyes and focus on slow, natural breathing.
Remain for 5–10 minutes, allowing the body to relax fully.
🌿 Why Choose Homeopathy?
Homeopathy is a natural system of care that focuses on understanding the underlying factors contributing to illness, rather than addressing symptoms alone. It works by supporting the body’s natural regulatory mechanisms and is commonly used across different age groups under professional guidance. Individualized care is central to homeopathic practice and is often used as part of long-term health management.
Homeopathy may be considered for both chronic conditions and acute concerns, with treatment plans tailored to the individual’s physical, emotional, and lifestyle factors.
🌟 Spiritual Homeopathy Clinic: Approach to Care
At Spiritual Homeopathy Clinic, care is centered on a comprehensive understanding of each patient’s health concerns. The clinical approach emphasizes careful evaluation of symptoms, overall health status, and contributing factors to support balanced well-being.
Consultations are available across multiple branches in Hyderabad, with options for online and international consultations for those unable to visit in person.
💫 Why Choose Spiritual Homeopathy Clinic?
The clinic follows a structured and individualized approach based on classical homeopathic principles and clinical assessment. Key aspects of care include:
Individualized Care: Treatment plans are tailored based on personal health history, symptoms, and overall constitution.
Root-Factor Assessment: Focus is placed on identifying contributing physical and emotional factors influencing the condition.
Clinical Experience: Consultations are provided by qualified homeopathy practitioners across Hyderabad branches, with online consultation support available.
Well-Tolerated Approach: Homeopathic care is generally well-tolerated when taken under professional supervision.
Holistic Perspective: Attention is given to the interaction between physical health, emotional well-being, and lifestyle factors.
🔍 Our Treatment Process
🩺 1. In-Depth Consultation
Each consultation involves a detailed discussion of symptoms, medical history, lifestyle patterns, and emotional health. This assessment supports the development of an individualized care plan aligned with the patient’s needs.
🔄 2. Individualized Homeopathic Care
The homeopathic approach focuses on addressing contributing factors and supporting long-term management. Care plans are adjusted based on response and overall progress.
🔁 3. Follow-Up and Monitoring
Regular follow-ups allow ongoing evaluation of symptoms and response to care. Adjustments are made as needed to support gradual and sustained improvement.
❤️ Patient Care Commitment
Spiritual Homeopathy Clinic emphasizes ethical practice, patient safety, and clear communication. Homeopathic care is intended to support overall health and should be undertaken under professional guidance, especially for chronic or persistent conditions.
When to Consult for Obsessive-Compulsive Disorder (OCD)
You should consult a healthcare professional if obsessive thoughts or compulsive behaviors become frequent, intense, or start interfering with your daily life. Early evaluation helps in understanding the condition better and prevents symptoms from becoming more severe over time.
Seek professional consultation if you experience:
Repeated, unwanted thoughts that cause anxiety or fear
Compulsive behaviors or mental rituals that are hard to control
Spending excessive time on checking, cleaning, counting, or reassurance-seeking
Difficulty concentrating at work, school, or home due to obsessive thoughts
Increased anxiety, restlessness, or emotional distress
Sleep disturbances caused by persistent thoughts or rituals
Avoidance of people, places, or activities due to fear or anxiety
Symptoms that do not improve or worsen over time
At Spiritual Homeopathy Clinic, consultations are available across multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for individuals who are unable to visit the clinic in person.
A professional evaluation helps in creating a personalized treatment plan based on individual symptoms, emotional well-being, and overall health.
📞 For appointments or guidance, contact: 9069 176 176
FAQS
1. What is Obsessive-Compulsive Disorder (OCD)?
Obsessive-Compulsive Disorder (OCD) is a mental health condition marked by recurring, unwanted thoughts (called obsessions) and repetitive behaviors or mental acts (called compulsions). These behaviors are performed to reduce anxiety or prevent a feared outcome, even though the person often knows the thoughts or actions are irrational.
2. What are the common symptoms of OCD?
OCD symptoms generally fall into two categories:
Obsessions
Repeated, intrusive thoughts, images, or urges
Common themes include fear of contamination, harm, mistakes, or unwanted thoughts
These thoughts cause anxiety or distress
Compulsions
Repetitive actions or mental rituals done to reduce anxiety
Examples include excessive hand washing, checking, counting, praying, or mental reviewing
3. Is OCD a type of anxiety disorder?
Yes. OCD is closely related to anxiety disorders and involves intense anxiety and fear. Although it is now classified separately due to its unique features, anxiety remains a central component of the condition.
4. What causes OCD?
There is no single cause of OCD. It is believed to develop due to a combination of factors, including:
Genetic factors: OCD can run in families
Neurobiological factors: Changes in brain structure and function, especially in areas linked to fear and decision-making
Psychological and environmental factors: Trauma, chronic stress, or early life experiences
5. Can OCD be cured?
There is no permanent “cure” for OCD, but it can be effectively managed. With the right treatment approach, many individuals experience significant symptom reduction and improved quality of life.
6. What are the treatment options for OCD?
Common treatment approaches include:
Cognitive Behavioral Therapy (CBT):
Especially Exposure and Response Prevention (ERP), which helps individuals face obsessive thoughts without performing compulsionsMedications:
Selective Serotonin Reuptake Inhibitors (SSRIs) are commonly prescribedSupport groups and counseling:
These provide emotional support and coping strategies
7. Can OCD symptoms get worse over time?
Yes. If left untreated, OCD symptoms may become more severe and interfere with daily life, work, relationships, and emotional well-being. Early diagnosis and consistent treatment lead to better outcomes.
8. What is the difference between obsessions and compulsions?
Obsessions: Unwanted thoughts, urges, or images that cause anxiety
Compulsions: Repetitive behaviors or mental acts performed to reduce anxiety caused by obsessions
9. Is OCD the same as being neat or organized?
No. OCD is not about liking cleanliness or order. People with OCD perform behaviors out of fear and anxiety—not preference or enjoyment—and feel distressed if they cannot complete their rituals.
10. Can children have OCD?
Yes. OCD can affect children and adolescents, often beginning at a young age. Early identification and treatment are important to prevent long-term emotional and behavioral difficulties.
11. Can stress make OCD worse?
Yes. Stress does not cause OCD, but it can trigger symptoms or make existing symptoms more intense. Managing stress is an important part of OCD care.
12. How can I help a loved one with OCD?
You can support someone with OCD by:
Learning about the condition
Encouraging professional treatment
Being patient, supportive, and non-judgmental
Avoiding participation in compulsive behaviors
13. What is Pure O (Pure Obsessional OCD)?
Pure O refers to OCD where compulsions are not easily visible. Instead of physical rituals, individuals experience mental compulsions such as repeated thoughts, mental checking, or silent reassurance. Though less visible, the distress is equally real and challenging.