Functional Enuresis
Functional Enuresis in Children and Adults: Natural Ways to Manage Bedwetting
- Home
- Functional Enuresis
Functional Enuresis
Homeopathy treatment for Functional Enuresis
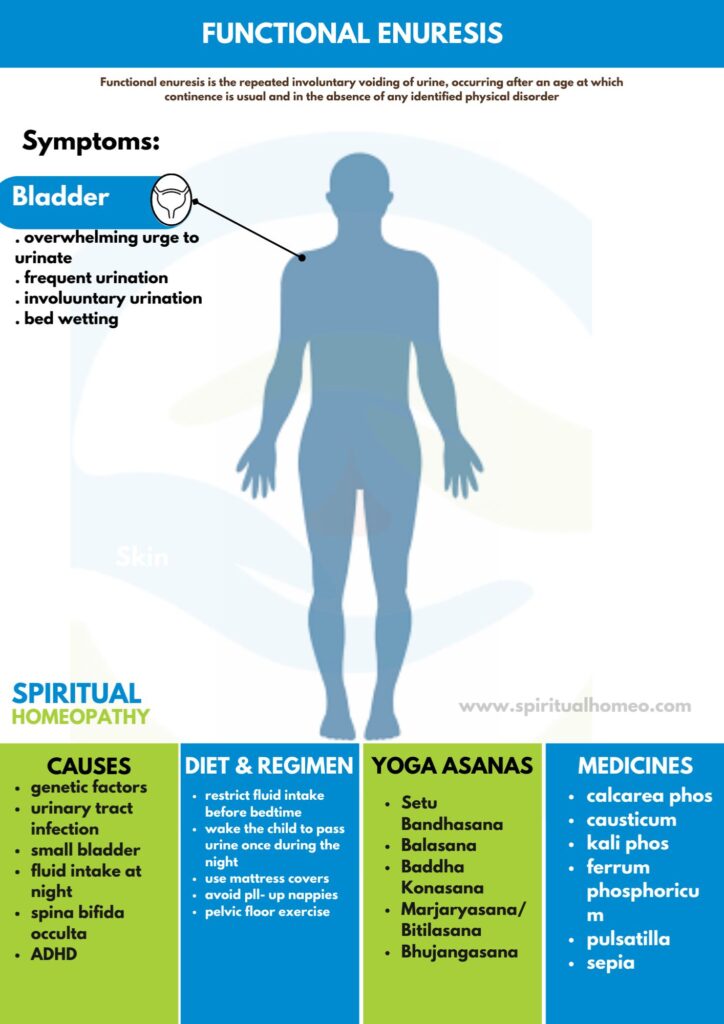
Functional Enuresis refers to the repeated, involuntary passing of urine—typically during sleep—after the age when bladder control is normally achieved, and without any underlying medical or physical condition causing it.
Everything You Need to Know
Overview of Functional Enuresis (Bedwetting)
Functional enuresis is a condition in which involuntary urination occurs in children or adults who have otherwise reached the expected age for bladder control. It is commonly categorized into two main types:
Nocturnal Enuresis – bedwetting during sleep
Diurnal Enuresis – involuntary urination during waking hours
Some individuals may experience both forms.
Nocturnal enuresis is further classified as:
Primary enuresis, where the individual has never achieved consistent nighttime bladder control
Secondary enuresis, where bedwetting reappears after a dry period, usually lasting six months or longer
Most children develop reliable daytime and nighttime bladder control between the ages of 3 and 4 years. The age of 5 years is generally considered the minimum age for diagnosing enuresis.
Consultation with a healthcare professional helps assess contributing factors and guide individualized care. At Spiritual Homeopathy Clinic, consultations are available across multiple branches in Hyderabad, as well as through online and international consultation services.
Prevalence and Emotional Impact
Nocturnal enuresis is relatively common and can be emotionally distressing for both children and parents. Concerns often arise due to embarrassment, social avoidance, or emotional stress related to misunderstanding or inappropriate responses.
Reported prevalence includes:
Around 10% of children at age 5
Approximately 4% at age 8
About 1% by age 14
Nearly 0.5% of cases may persist into adulthood
The condition is more frequently observed in boys with nighttime enuresis, while daytime enuresis is less common and occurs more often in girls.
A supportive and understanding approach, along with professional guidance, can help manage the emotional and physical aspects of enuresis over time.
Causes of Functional Enuresis
In most cases of primary nocturnal enuresis (bedwetting during sleep), the exact cause is idiopathic, meaning no clear underlying medical condition is identified. The most commonly recognized factor is a delay in the maturation of the nervous system responsible for bladder control.
Enuresis often shows a familial pattern. Children whose parents experienced bedwetting are more likely to develop the condition. Studies indicate a higher likelihood when there is a family history—about 44% if one parent was affected and up to 70% if both parents had enuresis.
While primary nocturnal enuresis is frequently linked to developmental delay, secondary nocturnal or diurnal enuresis may involve additional medical, psychological, or lifestyle-related factors.
Common Causes of Nocturnal Primary Enuresis
Idiopathic developmental delay: Delayed maturation of bladder control mechanisms
Genetic factors: A strong family history increasing susceptibility
Less Common Causes (Usually Associated with Secondary Enuresis)
Urinary tract infections (UTIs): May cause urgency and irritation
Diabetes mellitus: Increased urine output can contribute to wetting
Urinary tract abnormalities: Such as reduced bladder capacity or vesicoureteric reflux
Nervous system conditions: Including spina bifida occulta
Chronic constipation: Pressure on the bladder may lead to incontinence
Diuretics: Caffeine, alcohol, and similar substances increase urine production
ADHD (Attention Deficit Hyperactivity Disorder): May affect awareness of bladder signals
Developmental or learning disorders: Difficulty recognizing or responding to bodily cues
Psychological factors: Stress, trauma, bereavement, or bullying
Obstructive sleep apnoea: Altered sleep patterns may contribute to nighttime wetting
Epilepsy: Neurological disturbances can interfere with bladder control
Additional Contributing Factors
Excess fluid intake at night: Can exceed bladder capacity
Bladder pressure from bowel issues: Constipation affecting bladder function
Reduced bladder sensation: Difficulty recognizing bladder fullness
Stress and anxiety: Emotional factors influencing involuntary urination
Hyperactivity: Delayed or missed toileting due to excessive activity
Lack of attention: Distraction from bodily signals, especially during play
Understanding these contributing factors helps guide an individualized care approach based on the child’s symptoms, development, and overall health. Consultation with a healthcare professional supports appropriate evaluation and long-term management. At Spiritual Homeopathy Clinic, consultations are available across multiple branches in Hyderabad, as well as through online and international consultation options.
Types of Functional Enuresis (Bedwetting)
Functional enuresis, commonly known as bedwetting, is a condition seen mainly in children and is broadly classified into two main types: Primary Enuresis and Secondary Enuresis. Understanding the type helps in planning appropriate and individualized care. Consultation is available at Spiritual Homeopathy Clinic through in-clinic visits at multiple Hyderabad branches, as well as online and international consultations.
Primary Enuresis
Primary enuresis refers to children who have never achieved consistent nighttime dryness. It is commonly observed in younger children and is often considered part of normal developmental variation. Most children gradually outgrow this condition as bladder control matures. However, in some cases, primary enuresis may continue beyond the expected age.
Genetic factors and delayed development of bladder control are commonly associated with primary enuresis, highlighting the need for age-appropriate and individualized assessment.
Secondary Enuresis
Secondary enuresis occurs when a child who was previously dry at night begins bedwetting again after a significant dry period. This type usually requires closer evaluation, as it may be associated with factors such as emotional stress, changes in environment, urinary infections, or other underlying health concerns.
Identifying and addressing the contributing cause is important in managing secondary enuresis effectively under professional guidance.
Key Influencing Factors
Both primary and secondary enuresis may be influenced by multiple factors, including:
Genetic factors: A family history of bedwetting can increase the likelihood of enuresis.
Environmental factors: Changes in routine, family stress, or emotional triggers may play a role.
Physiological factors: Delayed bladder maturation, reduced bladder capacity, or sleep patterns can affect nighttime bladder control.
These factors are carefully considered during consultation to support individualized care planning.
Treatment Approaches
Management of functional enuresis generally focuses on understanding the underlying factors and supporting the child’s overall development. Common approaches may include:
Behavioral strategies: Bladder training techniques and maintaining regular bathroom routines.
Medical evaluation: Assessment to rule out infections or other contributing conditions.
Professional guidance: Consultation with a qualified healthcare professional to plan appropriate long-term management.
Treatment strategies may vary based on the child’s age, type of enuresis, and overall health status.
When to Consult a Doctor
Medical consultation is advised if bedwetting is frequent, persists beyond the expected age, begins suddenly after dryness, or is associated with other symptoms such as pain, stress, or behavioral changes.
At Spiritual Homeopathy Clinic, experienced doctors offer in-clinic, online, and international consultations for personalized evaluation.
Symptoms of Functional Enuresis
Functional enuresis can manifest in various ways, and the pattern of involuntary urination may differ among individuals. Identifying these patterns is important for proper assessment and management. Consultations for evaluation and personalized care are available at Spiritual Homeopathy Clinic through multiple branches in Hyderabad, as well as online and international consultations.
Urge Incontinence
This occurs when there is a sudden, strong urge to urinate that is difficult to control, often leading to frequent accidents. Children or adults may struggle to delay urination, and it can sometimes be associated with urinary tract infections (UTIs).
Voiding Postponement
Voiding postponement involves intentionally delaying urination, often due to situational factors such as school, work, or social settings. Over time, this may lead to discomfort and affect normal bladder function.
Stress-Related Leakage
Functional enuresis may include urine leakage triggered by physical pressure on the bladder, such as coughing, sneezing, laughing, or physical activity.
Giggling Incontinence
Some individuals experience involuntary urine loss specifically during laughter or play, caused by sudden pressure on the bladder.
Secondary Functional Enuresis
This type may develop after significant emotional stress, trauma, or life changes. Symptoms are often linked to psychological or situational triggers rather than a direct physical cause and require careful assessment.
Diet and Regimen for Managing Functional Enuresis (Bedwetting)
Managing functional enuresis, commonly known as bedwetting, involves supportive dietary habits and daily routines that help maintain healthy bladder function. Along with medical guidance, consistent lifestyle measures play an important role in overall management.
Increase Fluid Intake During the Day
Adequate hydration during daytime hours is important for normal bladder function. Drinking sufficient water throughout the day is encouraged, while fluid intake may be reduced 1–2 hours before bedtime to help limit nighttime wetting.
Avoid Caffeine and Sugary Drinks
Beverages that may irritate the bladder, such as caffeinated drinks, sodas, and sugary beverages, should be limited, as they can increase urine production and worsen bedwetting episodes.
Maintain a Healthy Diet
A balanced diet that includes fruits, vegetables, whole grains, and lean proteins supports overall health and may contribute to better bladder regulation.
Practice Bladder Training
Gradually extending the time between daytime urination can help improve bladder capacity and awareness, supporting better control over time.
Establish a Regular Bathroom Routine
Encouraging urination every 2–3 hours during the day, even without a strong urge, helps maintain a consistent bladder emptying pattern and supports healthy habits.
Prevent Constipation
Including fiber-rich foods such as fruits, vegetables, and whole grains can help prevent constipation, which may place pressure on the bladder and aggravate enuresis.
Dietary and routine guidance may vary depending on individual age, symptoms, and associated factors.
Yoga and Lifestyle Support for Functional Enuresis
Yoga practices may help support pelvic muscle awareness, relaxation, and stress management. These practices are considered supportive measures and should not replace medical evaluation or treatment.
1. Vajrasana (Thunderbolt Pose)
This pose helps strengthen pelvic muscles and supports bladder control. It also promotes calmness and aids digestion, which may be helpful if constipation is a contributing factor.
How to do it:
Sit on your knees with your back straight and hands resting on your thighs.
Keep your feet flat and close together, with big toes touching.
Sit back on your heels and hold for 1–2 minutes while breathing deeply.
2. Baddha Konasana (Bound Angle Pose)
This posture focuses on the pelvic region, helping improve circulation and muscle tone around the bladder.
How to do it:
Sit on the floor with legs extended.
Bend your knees and bring the soles of your feet together.
Hold your feet with your hands, keeping your back straight.
Gently press your knees toward the floor.
Hold for 30 seconds to 1 minute with deep breathing.
3. Setu Bandhasana (Bridge Pose)
Bridge Pose supports pelvic floor strength, which may assist in bladder control over time.
How to do it:
Lie on your back with knees bent and feet flat on the floor.
Keep arms by your sides with palms facing down.
Lift your hips while keeping feet and shoulders grounded.
Hold for 20–30 seconds and lower slowly.
Repeat 3–5 times.
4. Uttanasana (Standing Forward Bend)
This pose promotes relaxation and mental calmness, which may help reduce stress-related triggers of enuresis.
How to do it:
Stand with feet hip-width apart.
Bend forward from the hips, lowering your torso toward your legs.
Reach for your feet or the floor, keeping knees slightly bent if needed.
Hold for 30 seconds to 1 minute with steady breathing.
5. Paschimottanasana (Seated Forward Bend)
This posture stretches the lower back and supports nervous system relaxation, which may help reduce stress-related symptoms.
How to do it:
Sit with legs extended straight ahead.
Inhale and lengthen the spine.
Exhale and bend forward, reaching toward your feet.
Hold for 30 seconds to 1 minute with calm breathing.
6. Pranayama (Breathing Exercises)
Breathing techniques such as Anulom Vilom and Ujjayi may help reduce stress and promote nervous system balance.
How to do it (Anulom Vilom):
Sit comfortably with a straight spine.
Close the right nostril and inhale through the left.
Close the left nostril, open the right, and exhale.
Continue for 5–10 minutes.
7. Savasana (Corpse Pose)
This relaxation pose helps release tension and promotes deep rest, which may support stress-related symptom management.
How to do it:
Lie flat on your back with arms relaxed by your sides.
Close your eyes and focus on slow, natural breathing.
Remain in this position for 5–10 minutes.
Additional Tips
Practice yoga regularly, preferably at the same time each day.
Combine yoga with healthy daily habits, such as adequate daytime hydration and limiting fluids before bedtime.
Results may vary based on individual factors, age, and associated conditions.
Consultation with a healthcare professional is advised before starting any new yoga or lifestyle routine, especially if symptoms are persistent.
Why Choose Spiritual Homeopathy?
At Spiritual Homeopathy Clinic, we provide a holistic approach to healing that blends classical homeopathic methods with a deep understanding of the physical, emotional, and spiritual aspects of health. Our experienced team of homeopaths ensures compassionate, individualized care tailored to each patient’s needs.
Our Healing Approach
We focus on achieving harmony across physical, emotional, and spiritual health. Rather than only addressing symptoms, we work to identify underlying factors that contribute to your condition. This approach supports the body’s natural healing processes and promotes long-term well-being.
Our Services
Consultations: Our homeopaths in Hyderabad offer thorough in-person consultations at multiple branches, as well as online and international consultations for patients who cannot visit the clinic. Each consultation evaluates your medical history and current health concerns to design a personalized treatment plan.
Homeopathic Care: We provide gentle, carefully selected homeopathic remedies suitable for acute and chronic conditions. These treatments are intended to support individualized care while addressing contributing factors in a safe, well-monitored manner.
Follow-Up Support: Continuous guidance is an essential part of our care. Regular follow-ups help monitor progress, adjust treatment plans, and ensure your health goals are steadily supported.
Our Commitment
At Spiritual Homeopathy Clinic, your wellness is our priority. We are dedicated to compassionate, personalized care, focusing on overall health and well-being. Whether seeking support for a specific condition or enhancing general wellness, we provide guidance and care at every step of your healing journey.
When to Consult a Doctor
You should consult a healthcare professional if functional enuresis (bedwetting) becomes frequent, persistent, or begins to affect emotional well-being, daily activities, or sleep. Early evaluation helps identify contributing factors and supports appropriate management.
Seek consultation if you notice:
Bedwetting continuing beyond the expected age for bladder control
Sudden return of bedwetting after a dry period
Daytime urinary accidents or urgency
Pain or burning during urination
Bedwetting associated with stress, behavioral changes, or sleep disturbances
Symptoms not improving with routine measures and lifestyle adjustments
At Spiritual Homeopathy Clinic, consultations are available across multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for those unable to visit in person. Professional evaluation helps guide individualized care based on the child’s or adult’s overall health and contributing factors.
For consultation or guidance, contact 9069 176 176.
FAQ – Functional Enuresis
1. What is Functional Enuresis?
Functional enuresis is the involuntary passing of urine in children or adults who have typically reached the age of bladder control, without any identifiable physical abnormalities. It can occur during the day (diurnal) or at night (nocturnal) and may improve over time or with appropriate care. Consultations are available at our Hyderabad branches, as well as online and internationally.
2. What causes Functional Enuresis?
Functional enuresis can result from multiple factors, including:
Delayed development of bladder control
Family history or genetic predisposition
Urinary tract infections (UTIs)
Diabetes mellitus
Structural or functional abnormalities of the urinary tract
Nervous system issues
Chronic constipation
Use of diuretics such as caffeine or alcohol
Attention Deficit Hyperactivity Disorder (ADHD)
The causes vary for each individual, highlighting the importance of personalized care and professional assessment.
3. What are the symptoms of Functional Enuresis?
Common symptoms may include:
Urge incontinence: A sudden, strong need to urinate followed by accidental leakage
Voiding postponement: Difficulty urinating when the urge arises, often due to distractions or limited access to a restroom
Stress incontinence: Urine leakage with increased pressure on the bladder, such as during coughing, sneezing, or physical activity
Giggling incontinence: Involuntary urine loss triggered by laughter or sudden movements
If these symptoms are frequent or cause distress, consulting a healthcare professional can help identify underlying causes and develop an individualized management plan.