Vericose vein
Varicose Veins: Causes, Symptoms & Treatment Options | Expert Vein Care
- Home
- Vericose vein
Vericose vein
Effective Homeopathic Treatment for Varicose veins
Varicose veins are enlarged, swollen, and twisted veins that appear just beneath the surface of the skin, most commonly in the legs. They develop when vein valves become weak or damaged, causing blood to flow backward and pool, leading to visible bulging and discomfort. Common symptoms include aching, heaviness, and pain in the affected area. If left untreated, varicose veins can worsen over time and may impact daily comfort and mobility.
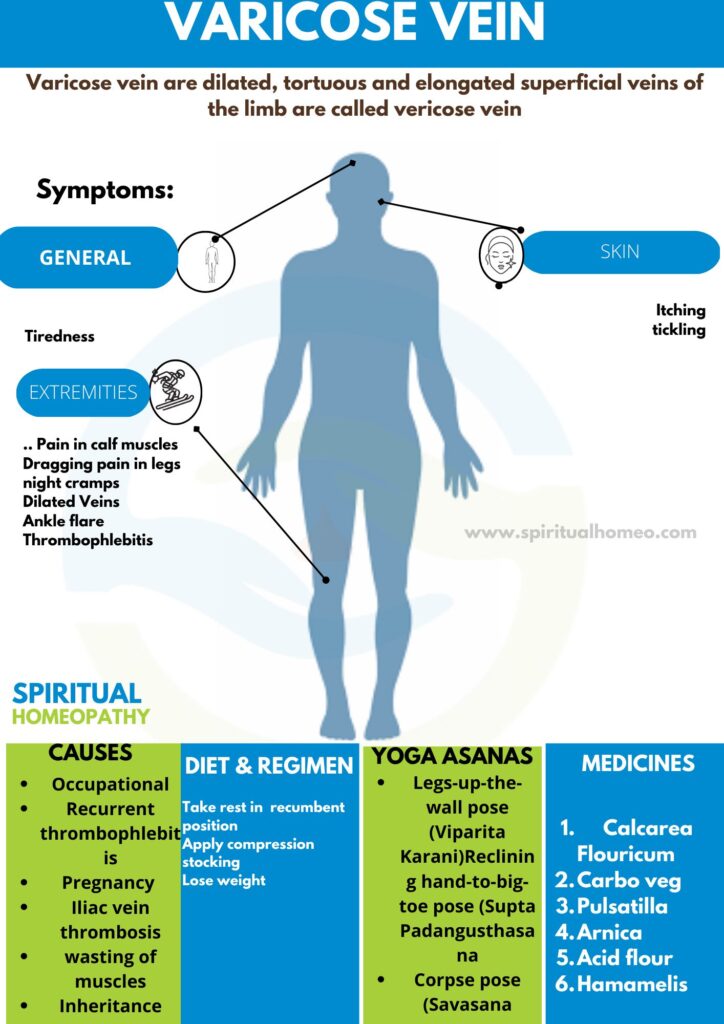
Everything You Need to Know
Overview
Varicose veins are often considered the price we pay for walking upright, as blood in the legs must work against gravity to return to the heart. In many people, varicose veins cause no symptoms; however, when symptoms are present, they may lead to discomfort, heaviness, and visible swelling of the veins. Raised intra-abdominal pressure—commonly seen in women due to repeated pregnancies—can increase the risk of developing this condition. In some cases, complications associated with varicose veins may become significant and require medical attention or hospitalization.
Consultations for varicose vein concerns are available at Spiritual Homeopathy Clinic across multiple branches in Hyderabad, as well as through online and international consultation services.
Causes
Varicose veins are most commonly found in the lower limbs due to the effects of gravity and our upright posture. The veins in the legs must push blood upward toward the heart, working against gravity. Over time, this sustained pressure can weaken vein valves and contribute to the development of varicose veins.
Causes of Varicosities:
Primary Varicosities
These develop without an underlying medical condition and may be associated with:
Congenital valve defects or absence of valves
Muscle weakness or loss, affecting vein support
Defective connective tissue or smooth muscle in vein walls
Stretching of the deep fascia
Hereditary factors, such as mutations in the FOXC2 gene
Klippel–Trenaunay syndrome, a rare congenital vascular disorder
Secondary Varicosities
These occur due to other health conditions or external factors, including:
Recurrent episodes of thrombophlebitis (inflammation of veins)
Occupations requiring prolonged standing, such as police or security services
Conditions that obstruct venous return, including abdominal tumors or enlarged lymph nodes
Pregnancy, particularly due to hormonal influences such as progesterone
Arteriovenous malformations, present from birth or acquired later
Thrombosis of the iliac vein
Understanding the underlying causes helps guide an individualized care approach, as contributing factors can vary from person to person and influence long-term management strategies.
Different Types of Varicose Veins
Varicose veins come in various forms, each with distinct features. While some types are mainly cosmetic, others may indicate underlying venous insufficiency or circulatory concerns. Understanding the type helps in appropriate evaluation and long-term management. The main types of varicose veins include:
1. Trunk Varicose Veins
These are large, rope-like veins that bulge above the surface of the skin, most commonly seen on the legs. They are the most noticeable type and are often associated with aching, heaviness, or discomfort, especially after prolonged standing.
2. Reticular Varicose Veins
Smaller than trunk veins, reticular veins appear as blue or green lines beneath the skin. They usually form in clusters and may not cause symptoms, but they can be an early sign of venous insufficiency.
3. Spider Veins (Telangiectasia)
These are tiny, thread-like veins visible close to the skin’s surface, forming a web-like pattern in red, blue, or purple shades. Spider veins commonly appear on the legs or face and are usually a cosmetic concern rather than a medical one.
4. Perforator Veins
Perforator veins connect the superficial veins to the deep venous system. When these veins become incompetent, they allow backward blood flow, increasing pressure in surface veins and contributing to the formation of varicosities.
5. Saphenous Varicose Veins
These involve the great or small saphenous veins, which run along the length of the leg. Varicosities in these veins can be extensive and may require careful medical evaluation due to the potential risk of complications.
6. Asymptomatic Varicose Veins
Not all varicose veins cause pain or swelling. Asymptomatic varicosities may still be visible and, over time, can progress or lead to complications if not medically assessed, even in the absence of discomfort.
Evaluation of the type of varicose veins supports an individualized care approach, which is central to long-term management under professional guidance.
Signs and Symptoms of Varicose Veins
Varicose veins can range from a mild cosmetic concern to a painful condition that affects daily life. Recognizing the symptoms early can help reduce the risk of progression and guide timely medical evaluation. Below are the most common signs and symptoms of varicose veins:
1. Visible, Twisted, or Bulging Veins
One of the most noticeable signs is the presence of enlarged, twisted, or bulging veins just beneath the skin—typically dark blue or purple in color. These are most often seen on the legs and are a hallmark feature of varicose veins.
2. Leg or Ankle Swelling
Swelling in the lower legs or ankles, especially after standing or sitting for long periods, may occur due to impaired blood flow and fluid accumulation in the affected veins.
3. Aching or Heavy Feeling in the Legs
Many individuals experience a dull ache or a heavy, tired sensation in the legs, particularly after prolonged standing, walking, or physical activity.
4. Pain or Tenderness Around Veins
The affected areas may feel sore or tender to the touch. Pain can be intermittent in some cases, while others may notice persistent discomfort throughout the day.
5. Itching or Burning Sensation
Skin around varicose veins may become itchy, dry, or irritated. A burning or tingling sensation is also commonly reported.
6. Skin Changes
With time, untreated varicose veins may lead to visible skin changes, including:
Thinning of the skin over the veins
Brownish discoloration, usually near the ankles
Dry, scaly patches or varicose eczema
In advanced cases, open sores or venous ulcers
7. Leg Cramps or Restlessness
Muscle cramps, particularly at night, and a restless or uncomfortable feeling in the legs can be associated with underlying venous circulation issues.
8. Throbbing or Pulsing Sensation
Some individuals notice a throbbing or pulsing sensation in the legs, especially after prolonged standing or walking.
9. Worsening of Symptoms With Prolonged Sitting or Standing
Symptoms often intensify after long periods of sitting or standing. Temporary relief may occur with leg elevation or gentle movement.
If these symptoms are frequent, worsening, or affecting daily activities, medical consultation is advised for proper assessment and guidance.
Diet and Lifestyle Tips for Managing Varicose Veins
While varicose veins are often a long-standing condition, certain diet and lifestyle changes can help reduce symptoms, support circulation, and maintain vein health. The following measures may assist in managing varicose veins as part of an overall care plan.
Diet for Varicose Vein Management:
1. Consume High-Fiber Foods
Why: Fiber supports digestion, reduces constipation, and helps limit pressure on veins, which may otherwise worsen varicose veins.
Foods to Include: Whole grains (brown rice, oats, quinoa), legumes (lentils, beans), fruits (apples, berries, pears), and vegetables (spinach, broccoli, carrots).
2. Include Vitamin C–Rich Foods
Why: Vitamin C supports collagen and elastin production, which are important for blood vessel structure.
Foods to Include: Citrus fruits, strawberries, bell peppers, kiwi, and leafy greens such as spinach.
3. Add Bioflavonoid-Rich Foods
Why: Bioflavonoids may support circulation and help reduce swelling.
Foods to Include: Berries, apples, onions, citrus fruits, and dark chocolate with higher cocoa content.
4. Incorporate Omega-3 Fatty Acids
Why: Omega-3 fatty acids support healthy blood flow and help manage inflammation.
Foods to Include: Fatty fish, chia seeds, flaxseeds, walnuts, and olive oil.
5. Eat Potassium-Rich Foods
Why: Potassium helps regulate fluid balance and may reduce leg and ankle swelling.
Foods to Include: Bananas, sweet potatoes, spinach, tomatoes, and oranges.
6. Magnesium-Rich Foods
Why: Magnesium supports muscle function and circulation and may help reduce leg cramps.
Foods to Include: Leafy greens, nuts, seeds, and beans.
7. Vitamin E for Healthy Circulation
Why: Vitamin E supports circulation and helps protect blood vessels from oxidative stress.
Foods to Include: Almonds, sunflower seeds, spinach, avocado, and olive oil.
8. Stay Hydrated with Water-Rich Foods
Why: Adequate hydration supports circulation and overall vascular health.
Hydrating Foods: Water, cucumbers, watermelon, celery, and oranges.
9. Anti-Inflammatory Foods
Why: Ongoing inflammation can worsen vein-related discomfort.
Foods to Include: Turmeric, ginger, garlic, green tea, and omega-3–rich foods.
10. Reduce Salt and Processed Foods
Why: Excess sodium can increase fluid retention and swelling.
Action: Limit processed foods and avoid adding extra salt to meals.
Regimen for Varicose Vein Relief:
1. Exercise Regularly
Why: Regular movement supports circulation and muscle tone.
Recommended Exercises: Walking, swimming, cycling, and calf-strengthening exercises.
How Often: Around 30 minutes of moderate activity, 3–5 times per week.
2. Elevate Your Legs
Why: Elevation helps reduce venous pressure and swelling.
Action: Elevate legs above heart level for 15–20 minutes, a few times daily.
3. Avoid Long Periods of Sitting or Standing
Why: Prolonged immobility can cause blood pooling in the legs.
Action: Change position every 30 minutes; avoid crossing legs while sitting.
4. Wear Compression Stockings
Why: Compression supports venous return and may reduce swelling.
How to Use: Wear during daytime hours, especially with prolonged standing or sitting.
5. Maintain a Healthy Weight
Why: Excess weight can increase pressure on leg veins.
Action: Combine balanced nutrition with regular physical activity.
6. Practice Good Posture
Why: Proper posture helps reduce unnecessary strain on veins.
Action: Stand upright and sit with feet flat on the floor and legs uncrossed.
7. Use Cold Compresses
Why: Cold application may help reduce localized swelling and discomfort.
Action: Apply a cold compress for 10–15 minutes, several times daily.
8. Avoid Tight Clothing
Why: Tight garments may restrict circulation.
Action: Choose loose-fitting clothing around the waist and legs.
9. Leg Exercises for Circulation
Why: Targeted movements support venous circulation.
Exercises to Try:
Calf Raises: Lift heels, hold briefly, and repeat.
Leg Lifts: Raise one straight leg at a time while lying down and hold briefly.
Dietary and lifestyle guidance may vary based on individual health status, symptoms, and daily routines, and should be adapted accordingly under professional advice.
Yoga and Lifestyle Support for Varicose Veins
Yoga practices can play a supportive role in managing varicose veins by encouraging circulation, reducing leg discomfort, and promoting relaxation. These practices are meant to complement medical care and are not a substitute for professional treatment.
1. Viparita Karani (Legs-Up-the-Wall Pose)
Benefits:
Relieves pressure on the legs and supports venous return
May help reduce swelling in the legs and ankles
Calms the nervous system and promotes relaxation
How to do it:
Sit with one hip close to a wall and gently swing your legs up as you lie on your back
Keep legs straight and feet relaxed
Place arms by your sides with palms facing up and close your eyes
Hold for 5–15 minutes with slow, relaxed breathing
2. Setu Bandhasana (Bridge Pose)
Benefits:
Strengthens the legs and gluteal muscles
Supports circulation in the lower body
Helps relieve back tension and leg discomfort
How to do it:
Lie on your back with knees bent and feet hip-width apart
Place arms beside you, palms down
Press into your feet and gently lift your hips
Keep shoulders and head on the mat
Hold for 15–30 seconds and slowly release
3. Supta Baddha Konasana (Reclining Bound Angle Pose)
Benefits:
Opens hips and inner thighs
Encourages circulation to the lower limbs
May help reduce swelling and discomfort
How to do it:
Lie on your back and bring the soles of your feet together
Allow knees to fall outward comfortably
Place hands on the abdomen or beside the body
Hold for 3–5 minutes with deep breathing
4. Adho Mukha Svanasana (Downward-Facing Dog Pose)
Benefits:
Improves overall circulation
Stretches calves, hamstrings, and lower back
Encourages blood flow toward the heart
How to do it:
Begin on hands and knees
Lift hips upward to form an inverted “V” shape
Press heels gently toward the floor
Hold for 30 seconds to 1 minute, then release
5. Uttanasana (Standing Forward Bend)
Benefits:
Stretches the back and leg muscles
Supports venous circulation
Helps relieve lower body tension
How to do it:
Stand with feet hip-width apart
Hinge forward from the hips
Allow head and neck to relax
Hold for 30 seconds to 1 minute and rise slowly
6. Tadasana (Mountain Pose)
Benefits:
Improves posture and body alignment
Supports balanced weight distribution and circulation
How to do it:
Stand upright with feet together
Engage thighs and lengthen the spine
Keep chin parallel to the floor
Hold for 30 seconds to 1 minute with steady breathing
7. Malasana (Garland Pose)
Benefits:
Opens hips and groin
Supports flexibility in knees and ankles
Encourages circulation in the lower body
How to do it:
Stand with feet slightly wider than hips
Squat down while keeping heels grounded
Place elbows inside knees and palms together
Hold for 30 seconds to 1 minute
8. Anjaneyasana (Low Lunge Pose)
Benefits:
Stretches hip flexors, thighs, and calves
Builds lower body strength
Supports circulation
How to do it:
Step one foot forward into a lunge from a kneeling position
Lower hips gently
Raise arms overhead
Hold for 30 seconds to 1 minute, then switch sides
Additional Tips for Yoga Practice with Varicose Veins
Focus on breathing: Slow, deep breathing supports relaxation and circulation
Avoid overexertion: Do not continue any pose that causes strain or pain
Maintain consistency: Gentle practice 2–3 times per week may offer supportive benefits
Individuals with significant pain, swelling, or complications should seek medical guidance before starting or continuing yoga practices.
Why Choose Spiritual Homeopathy for Care?
At Spiritual Homeopathy Clinic, we follow a holistic and patient-focused approach that considers physical, emotional, and lifestyle factors affecting health. Our homeopathic practitioners aim to provide individualized care based on a detailed understanding of each patient’s health concerns and overall well-being. Consultations are available across multiple branches in Hyderabad, as well as through online and international consultation options.
Our Approach to Care
We believe health concerns often involve multiple contributing factors rather than isolated symptoms. Our approach focuses on understanding these factors and supporting the body’s natural healing processes through long-term management strategies. Care plans are designed to align with the individual’s health history, symptom pattern, and current lifestyle, under professional guidance.
Our Services
Comprehensive Consultations:
Our homeopathy practitioners conduct detailed consultations to understand medical history, current symptoms, and relevant lifestyle aspects. This helps in planning an appropriate and personalized care approach. Online consultations are also available for patients who are unable to visit the clinic in person.
Homeopathic Care Approach:
Homeopathy at Spiritual Homeopathy Clinic focuses on addressing contributing factors and supporting overall balance. The approach is generally well-tolerated when followed under professional supervision and is used as part of a broader health management plan.
Ongoing Follow-Up Care:
Health management is an evolving process. Regular follow-ups help monitor changes in symptoms, review progress, and make necessary adjustments to the care plan over time, based on clinical assessment.
Our Commitment to Patient Care
At Spiritual Homeopathy Clinic, patient safety, clarity, and informed decision-making are prioritized. Care is provided with attention to physical comfort, emotional well-being, and realistic health goals. Individuals seeking support for conditions such as varicose veins may benefit from professional evaluation to determine whether homeopathy can be considered as part of their overall care plan.
When to Consult
You should consult a healthcare professional if varicose vein symptoms become noticeable, persistent, or start affecting daily comfort and mobility. Early evaluation helps identify contributing factors and supports timely management, reducing the risk of progression or complications.
Seek consultation if you experience:
Visible, enlarged, or twisted veins in the legs
Leg heaviness, aching, or discomfort after standing or sitting for long periods
Swelling in the legs or ankles, especially by the end of the day
Burning, throbbing, or cramping sensations in the legs
Skin discoloration, dryness, or itching around affected veins
Restlessness or discomfort in the legs during the night
Symptoms not improving with lifestyle measures such as leg elevation or regular movement
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for individuals who are unable to visit in person. A professional assessment helps guide an individualized care approach based on symptoms, circulation status, and overall health.
For appointments or guidance, contact 9069 176 176.
FAQ
1. What are varicose veins?
Varicose veins are enlarged, twisted veins most commonly seen in the legs and feet. They occur when vein valves weaken or become damaged, causing blood to pool and the veins to appear swollen, visible, and sometimes uncomfortable.
2. What causes varicose veins?
Varicose veins develop due to weakened or damaged vein valves that affect normal blood flow. Contributing factors include:
Genetics (family history of varicose veins)
Prolonged standing or sitting
Pregnancy (hormonal changes and increased blood volume)
Obesity
Aging
Hormonal changes (such as menopause or hormonal contraceptives)
Understanding these causes helps guide an individualized care approach.
3. Are varicose veins dangerous?
In most cases, varicose veins are not dangerous but may cause discomfort or cosmetic concerns. In some situations, complications can occur, such as:
Blood clots (thrombophlebitis)
Skin ulcers near affected veins
Bleeding from veins
If severe pain, swelling, or skin changes occur, medical evaluation is advised.
4. What are the symptoms of varicose veins?
Common symptoms include:
Swollen, bulging veins (often dark blue or purple)
Pain, aching, or heaviness in the legs
Itching or burning sensations over veins
Swelling in legs or ankles
Muscle cramps, especially at night
Consultation is recommended if symptoms are frequent, progressive, or interfere with daily activities.
5. Can varicose veins be prevented?
Varicose veins cannot always be prevented, but certain measures may help reduce risk:
Maintaining a healthy weight
Regular physical activity to support circulation
Avoiding prolonged standing or sitting
Elevating legs during rest
Using compression stockings when advised
6. How are varicose veins treated?
Management depends on severity and may include:
Lifestyle measures such as exercise, weight management, and leg elevation
Compression stockings to support circulation
Medical procedures like sclerotherapy or endovenous therapies
Surgical options in selected cases
A healthcare professional can guide suitable options based on individual assessment.
7. Are varicose veins hereditary?
Yes. A family history of varicose veins increases the likelihood of developing the condition.
8. Can I exercise if I have varicose veins?
Yes. Regular, low-impact exercise such as walking, swimming, or cycling is generally beneficial for circulation. Activities that place excessive strain on the legs may need to be moderated based on individual tolerance.
9. Do compression stockings help with varicose veins?
Compression stockings are commonly used to improve blood flow, reduce swelling, and limit blood pooling. They are often recommended for people who stand or sit for long periods.
10. Can varicose veins go away on their own?
Varicose veins usually do not disappear without treatment. Symptoms may improve with lifestyle measures, but visible veins often persist unless addressed through medical intervention.
11. Is there any natural approach for varicose veins?
Natural measures may help ease symptoms but do not eliminate varicose veins. These may include:
Leg elevation
A balanced diet supporting vascular health
Gentle massage and lifestyle modifications
Such measures are supportive and should not replace medical evaluation.
12. How do I know if I need medical care for varicose veins?
Medical advice is recommended if there is significant pain, swelling, skin changes, ulcers, or concern about appearance. Professional assessment helps determine appropriate management options.
13. Will varicose veins come back after treatment?
Recurrence can occur, especially if contributing factors like genetics or prolonged standing remain. Regular follow-up and healthy habits may help reduce recurrence risk.
At Spiritual Homeopathy Clinic, consultations for varicose vein concerns are available at multiple branches in Hyderabad, as well as through online and international consultation options.
