Bronchiectasis
Understanding Bronchiectasis: Symptoms, Causes, and Treatment Options
- Home
- Bronchiectasis
Bronchiectasis
Brochiectasis
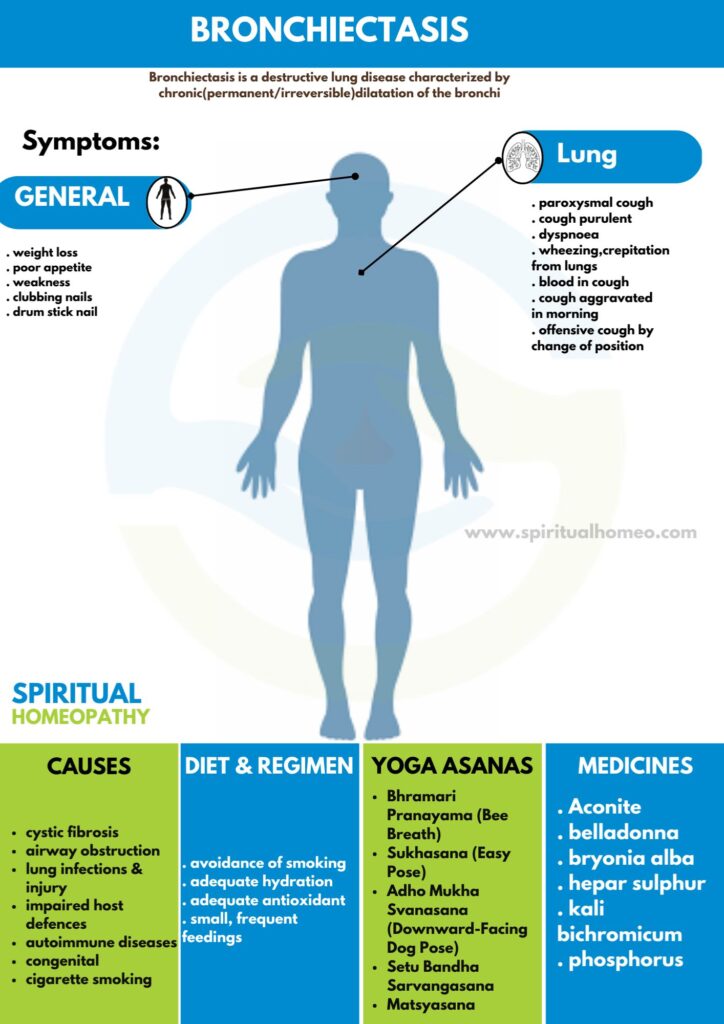
Bronchiectasis is a chronic and irreversible lung condition marked by the permanent enlargement of the bronchi. It is associated with ongoing inflammation in the lungs, which can vary in severity over time. This destructive disease leads to the progressive deterioration of lung tissue, impairing respiratory function.
Everything You Need to Know
Overview
Bronchiectasis is a chronic lung condition that affects between 1 in 1,000 and 1 in 250,000 adults. It is more commonly seen in women and tends to become more prevalent with age. Cystic fibrosis is identified as the underlying cause in up to 50% of cases.
When bronchiectasis occurs without cystic fibrosis, it is referred to as non-CF bronchiectasis. Historically, about half of non-CF bronchiectasis cases have been classified as idiopathic, meaning no clear cause is identified.
Several factors and conditions can contribute to the development of bronchiectasis, and its diagnosis often requires a thorough evaluation, including medical history, imaging, and pulmonary function tests.
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, as well as online and international appointments, allowing patients to receive professional guidance and individualized care for bronchiectasis.
Causes of Bronchiectasis
Bronchiectasis is a complex lung condition that can arise from multiple factors. Causes vary by geographic location, and while cystic fibrosis (CF) is a common contributor, many cases are idiopathic or have other identifiable origins. Understanding these causes helps guide appropriate management and care.
-
Cystic Fibrosis (CF)
Cystic fibrosis is a genetic disorder affecting the lungs, pancreas, liver, and intestines. It leads to thick mucus buildup in the lungs, causing airway blockages, increased susceptibility to infections, and airway inflammation, which can damage lung tissue. Approximately 5–10% of CF patients develop bronchiectasis. -
Airway Obstruction
Obstructions caused by tumors, foreign bodies, or other factors can impair airflow and trigger repeated infections, contributing to bronchiectasis. In adults, foreign body aspiration often affects the right lower lobe or posterior segments of the upper lobe and is commonly associated with altered consciousness. -
Lung Infections
Chronic bacterial, mycobacterial, and viral infections are significant contributors. Bacteria such as Pseudomonas aeruginosa, Haemophilus influenzae, and Streptococcus pneumoniae are frequently found in affected patients. Mycobacterial infections, including tuberculosis and non-tuberculous mycobacteria (e.g., Mycobacterium avium complex), and severe viral infections during childhood can also cause long-term airway damage. -
Impaired Host Defenses
Individuals with congenital or acquired immune deficiencies are at higher risk. Primary ciliary dyskinesia, HIV/AIDS, and other immunodeficiency conditions can lead to frequent infections that weaken bronchial walls and promote bronchiectasis. -
Allergic Bronchopulmonary Aspergillosis (ABPA)
ABPA is caused by an allergic reaction to the fungus Aspergillus fumigatus, often in patients with asthma. It can result in productive coughing, mucus buildup, and airway damage, with imaging typically showing central and peripheral bronchiectasis. -
Autoimmune Diseases
Autoimmune conditions such as rheumatoid arthritis, Sjogren syndrome, and Crohn’s disease can trigger lung inflammation, eventually contributing to bronchiectasis. Graft-versus-host disease following stem cell transplantation may also increase risk. -
Lung Injury
Chronic lung injury from inhaling toxic gases, pulmonary aspiration from acid reflux or hiatal hernia, or physical trauma can damage lung tissue, promoting bronchiectasis development. -
Congenital Disorders
Other than CF, rare genetic disorders like primary ciliary dyskinesia, Young’s syndrome, and Williams-Campbell syndrome may cause bronchiectasis. Kartagener’s syndrome, associated with situs inversus, chronic sinusitis, and bronchiectasis, is another example. -
Tracheobronchomegaly (Mounier-Kuhn Syndrome)
This rare condition leads to abnormal dilation of the trachea and bronchi, causing recurrent lower respiratory infections and increasing the risk of bronchiectasis. -
Alpha-1 Antitrypsin Deficiency
A deficiency of alpha-1 antitrypsin reduces lung protection from elastase, an enzyme that breaks down lung tissue. This increases susceptibility to damage and bronchiectasis. -
Cigarette Smoking
While not a direct cause, smoking can worsen existing lung damage and accelerate bronchiectasis progression.
Types of Conditions That Can Lead to Bronchiectasis
Several underlying health conditions can cause or contribute to the development of bronchiectasis. Recognizing these types helps guide proper evaluation and personalized management.
1. Cystic Fibrosis (CF)
Cystic fibrosis is a genetic disorder and a leading cause of bronchiectasis, particularly in the United States. It results in thick, sticky mucus in the lungs, which increases the risk of frequent infections and airway damage.
2. Immunodeficiency Disorders
Conditions that weaken the immune system, such as common variable immunodeficiency (CVID) and, less commonly, HIV/AIDS, make the lungs more susceptible to infections that may lead to bronchiectasis.
3. Allergic Bronchopulmonary Aspergillosis (ABPA)
ABPA is an allergic reaction to the Aspergillus fungus, causing chronic inflammation and mucus accumulation in the airways. Over time, this immune response can contribute to bronchiectasis.
4. Ciliary Dysfunction Disorders
Diseases like primary ciliary dyskinesia affect the function of cilia—tiny hair-like structures that clear mucus from the respiratory tract. Impaired cilia movement leads to mucus buildup and recurrent infections, resulting in airway damage.
5. Chronic Pulmonary Aspiration
Repeated inhalation of food, liquids, or stomach acid into the lungs can irritate and inflame the airways. If persistent, this can lead to the development of bronchiectasis.
6. Connective Tissue Diseases
Autoimmune conditions such as rheumatoid arthritis, Sjögren’s syndrome, and Crohn’s disease can trigger lung inflammation, which may contribute to bronchiectasis over time.
Signs and Symptoms of Bronchiectasis
Bronchiectasis is a chronic lung condition characterized by abnormal widening of the airways, leading to mucus buildup and repeated infections. Early recognition of symptoms can help in management and improve quality of life. Consult a healthcare professional if symptoms are frequent, severe, or worsening.
1. Recurrent Respiratory Infections
Frequent episodes of bronchitis, especially during colder months, are common early signs.
Individuals may experience repeated chest infections with persistent coughing and mucus production.
2. Chronic Cough and Sputum Production
A chronic, productive cough is a hallmark symptom.
In severe cases, thick, purulent (pus-filled) sputum may be expelled daily.
Cough may worsen in certain positions, particularly if caused by airway obstruction (e.g., foreign body or post-anesthesia).
3. Hemoptysis (Coughing Up Blood)
Some patients may experience recurrent hemoptysis without significant mucus production (bronchiectasis sicca).
These episodes can occur even if the patient feels well between attacks.
4. Clubbing of Fingers
Long-standing cases may show bulbous fingertips and curved nails, ranging from mild “parrot-beak” curvature to “drumstick” enlargement.
5. Shortness of Breath and Wheezing
Approximately 75% of patients report dyspnea (shortness of breath) and wheezing during flare-ups.
These symptoms may sometimes be mistaken for asthma or COPD.
6. Chest Pain
Sharp, pleuritic chest pain may occur in about half of patients.
It is typically caused by inflammation in the lung lining (pleura) or distended peripheral airways.
7. Low-Grade Fever
Fever is uncommon during bronchiectasis exacerbations.
If present, particularly with chest pain or worsening symptoms, pneumonia should be considered.
8. Progressive Lung Changes
As the disease advances, physical signs may vary based on affected areas:
-
Early stages: Fine crackles (rales), sticky rhonchi, slight changes in breath sounds.
-
Late stages: Bronchial breathing, coarse crepitations, or signs of lung cavities.
Recurrent pneumonia in the same lung region is a classic feature.
9. Other Lung Complications
Signs may overlap with or mimic:
-
Chronic bronchitis
-
Pulmonary fibrosis
-
Lung collapse or consolidation
-
Cavitations or lung abscesses
Best Diet and Lifestyle Regimen for Managing Bronchiectasis
Managing bronchiectasis involves more than medications—daily diet and lifestyle choices play a key role in reducing flare-ups, supporting the immune system, and improving lung function. Individual guidance may vary depending on health status and severity of symptoms.
1. Stay Well-Hydrated
Drink plenty of water throughout the day to help thin mucus, making it easier to clear from the lungs.
Herbal teas and broths are also helpful for maintaining hydration.
2. Eat a Protein-Rich Diet
Include lean protein sources such as chicken, fish, eggs, beans, and lentils to support immune defense and muscle maintenance.
Protein is essential during infection recovery and helps repair damaged tissues.
3. Load Up on Antioxidant-Rich Foods
Consume colorful fruits and vegetables like berries, spinach, kale, and bell peppers.
These foods provide vitamins C and E, which help reduce inflammation and protect lung tissue.
4. Incorporate Healthy Fats
Add omega-3 fatty acids from sources like salmon, flaxseeds, chia seeds, and walnuts.
These fats offer anti-inflammatory benefits and support overall lung function.
5. Limit Salt Intake
Excess salt can lead to fluid retention and higher blood pressure, potentially affecting breathing.
Choose low-sodium alternatives and avoid heavily processed foods.
6. Eat Small, Frequent Meals
Smaller meals spaced throughout the day prevent bloating and make breathing easier, especially when lung function is reduced.
Avoid heavy meals before bedtime.
7. Stay Active with Gentle Exercise
Engage in regular, low-impact activities like walking, swimming, or yoga to improve lung capacity and stamina.
Pulmonary rehabilitation or guided breathing exercises can be beneficial under medical supervision.
Additional Tips:
Avoid smoking, air pollutants, and exposure to cold air, as these can exacerbate bronchiectasis symptoms.
🧘♂️ Best Yoga Asanas for Bronchiectasis
Yoga can support lung health, improve breathing, and reduce stress, but it should not replace medical care or prescribed treatments. Patients with bronchiectasis should consult a healthcare professional before starting new exercises.
1. Bhujangasana (Cobra Pose)
Benefits: Expands the chest and lungs, loosens mucus, improves posture, and opens the airways.
How to Practice: Lie on your stomach, place your hands under your shoulders, and slowly lift your upper body while inhaling. Hold for a few seconds, then exhale as you return to the floor.
2. Ardha Matsyendrasana (Half Spinal Twist)
Benefits: Enhances lung function, promotes oxygen flow, and massages internal organs to support digestion and immunity.
How to Practice: Sit with one leg bent and the opposite foot placed over the knee. Twist your torso toward the raised knee, using your opposite arm for support.
3. Setu Bandhasana (Bridge Pose)
Benefits: Opens the chest, strengthens the back, and improves circulation to the lungs.
How to Practice: Lie on your back with knees bent and feet flat. Lift your hips while keeping your shoulders on the floor and breathe deeply.
4. Anulom Vilom (Alternate Nostril Breathing)
Benefits: Clears nasal passages, improves respiratory balance, and calms the nervous system.
How to Practice: Inhale through one nostril while closing the other with your finger, then switch sides for exhalation. Repeat for 5–10 minutes daily.
5. Adho Mukha Svanasana (Downward-Facing Dog)
Benefits: Encourages mucus drainage from the lungs, increases lung capacity, and strengthens the diaphragm.
How to Practice: Start on hands and knees, lift your hips up and back to form an inverted V shape, and hold while breathing deeply.
6. Marjariasana-Bitilasana (Cat-Cow Stretch)
Benefits: Loosens the spine and chest, promotes better breathing, and relieves tension in the chest area.
How to Practice: On hands and knees, alternate between arching your back (cow) and rounding it (cat) with each breath.
7. Shavasana (Corpse Pose) with Deep Breathing
Benefits: Promotes relaxation, reduces stress, and allows for focused breathwork to improve lung capacity.
How to Practice: Lie flat on your back, close your eyes, and focus on deep, slow breathing while fully relaxing your body.
Homeopathic Treatment for Bronchiectasis at Spiritual Homeopathy
Why Choose Spiritual Homeopathy?
At Spiritual Homeopathy, we provide a holistic and compassionate approach that combines classical homeopathy with attention to physical, emotional, and spiritual well-being. Our aim is to support overall health and help manage the symptoms of bronchiectasis through individualized care.
Our experienced homeopaths in Hyderabad, also available for online and international consultations, design treatment plans tailored to each patient’s unique health profile and lifestyle.
Our Holistic Approach to Healing
Effective management of bronchiectasis involves addressing underlying factors in addition to symptom relief. Our homeopathic approach focuses on:
-
Supporting the body’s natural healing mechanisms
-
Reducing chronic inflammation
-
Enhancing immune resilience
-
Promoting better lung function and airway clearance
-
Supporting emotional and mental well-being
This comprehensive approach helps manage recurring infections, fatigue, and respiratory discomfort while supporting long-term health.
What We Offer
🩺 Personalized Consultations
Our practitioners conduct in-depth consultations, in-clinic or online, to understand your symptoms, medical history, and lifestyle. This enables an individualized treatment plan that aligns with your health needs.
🌿 Gentle and Natural Support
Homeopathic care aims to address the underlying imbalances contributing to bronchiectasis. Our treatments are generally well-tolerated under professional guidance and suitable for patients of different ages and health conditions.
🔄 Ongoing Follow-Up and Support
Healing is an ongoing process. Our team provides regular follow-ups, monitors progress, and adjusts treatment as needed to help manage symptoms and support long-term well-being.
Homeopathic Support for Bronchiectasis
Homeopathy at Spiritual Homeopathy Clinic is designed to:
-
Support mucus clearance and ease chronic coughing
-
Help improve lung function and reduce shortness of breath
-
Reduce the frequency of respiratory infections
-
Support tissue health and relieve chest discomfort
-
Strengthen overall immunity and resilience
By addressing both physical symptoms and contributing factors, homeopathic care can complement conventional approaches and help patients manage bronchiectasis more effectively.
Online Homeopathy Consultations
For patients in Hyderabad, across India, or internationally, online consultations make it convenient to access expert homeopathic guidance. Our practitioners provide ongoing support, from symptom management to long-term wellness planning.
Your Health, Our Priority
At Spiritual Homeopathy, we focus on supporting respiratory health, improving quality of life, and providing individualized care for bronchiectasis. Consultations are available at multiple Hyderabad branches, online, and internationally.
When to Consult a Doctor
You should consult a healthcare professional if bronchiectasis symptoms become frequent, severe, or start affecting daily activities or quality of life. Early evaluation helps identify contributing factors, prevent complications, and guide long-term management.
Seek consultation if you experience:
-
Recurrent or persistent respiratory infections
-
Chronic cough with thick or discolored mucus
-
Coughing up blood (hemoptysis)
-
Shortness of breath or wheezing that interferes with activities
-
Chest pain or discomfort
-
Unexplained fatigue, weight loss, or fever
-
Symptoms not improving with standard lifestyle or supportive measures
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients who cannot visit in person. Professional assessment ensures an individualized care plan based on your symptoms and overall health.
For appointments or guidance, contact 9069 176 176.
📌 Frequently Asked Questions (FAQs) About Bronchiectasis
1. What is Bronchiectasis?
Bronchiectasis is a chronic lung condition where the airways (bronchi) become permanently widened and damaged. This abnormal dilation leads to mucus buildup, making the lungs more prone to infections and inflammation. Over time, it can result in persistent respiratory symptoms and reduced lung function.
2. What are the Common Symptoms of Bronchiectasis?
Symptoms may vary depending on severity. Common signs include:
-
Chronic cough producing large amounts of mucus or phlegm
-
Shortness of breath (dyspnea) and wheezing
-
Recurrent respiratory infections or episodes of bronchitis
-
Hemoptysis (coughing up blood), particularly in advanced cases
-
Clubbing of the fingers (enlarged, rounded fingertips)
-
Chest discomfort or pain, especially during flare-ups
-
Paroxysmal cough, often worse at night or with a change in position
Note: Frequent or severe symptoms should be evaluated by a healthcare professional.
3. What Causes Bronchiectasis?
Bronchiectasis may develop due to various factors that damage the airways over time, including:
-
Genetic conditions affecting mucus production or lung defenses
-
Chronic or severe lung infections (e.g., pneumonia, whooping cough)
-
Airway obstruction from foreign objects, tumors, or scarring
-
Impaired immune function leading to repeated infections
-
Allergic reactions to environmental fungi or airborne irritants
-
Autoimmune disorders causing lung inflammation
-
Lung injuries from trauma, surgery, or harmful inhaled substances
-
Congenital abnormalities affecting airway structure
-
Long-term exposure to toxins, including cigarette smoke or pollution
Understanding the underlying cause is important for individualized care and effective management.
4. How Can Bronchiectasis Be Managed?
Management involves a combination of medical care, lifestyle adjustments, and supportive therapies:
-
Regular monitoring and treatment of infections
-
Breathing exercises and gentle physical activity to improve lung function
-
Nutritional guidance to support immunity and overall health
-
Homeopathic care focused on individualized treatment, reducing chronic symptoms, and supporting long-term respiratory health
5. When Should I Consult a Doctor?
Consult a healthcare professional if you experience:
-
Persistent or worsening cough
-
Frequent respiratory infections
-
Shortness of breath affecting daily activities
-
Coughing up blood
-
Chest discomfort or recurring fever