Osteoporosis
Osteoporosis Explained: Causes, Symptoms, Treatment Options, and Prevention Tips
- Home
- Osteoporosis
Osteoporosis
Effective Homeopathic Treatment for Osteoporosis
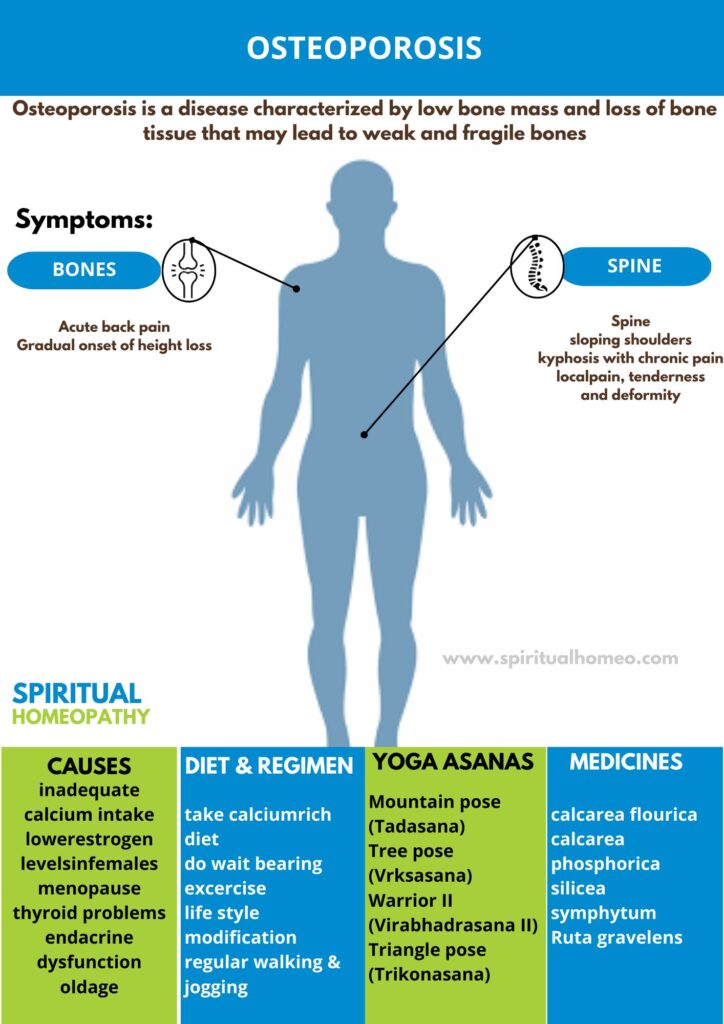
Osteoporosis is a condition where bones become weak and brittle due to low bone mass and loss of bone tissue. This progressive disease increases the risk of fractures, especially in the spine, hips, and wrists. It often develops silently over time, with no noticeable symptoms until a fracture occurs. Osteoporosis is more common in older adults and can be managed with a healthy diet, weight-bearing exercises, and medications to strengthen bones and reduce fracture risk.
Everything You Need to Know
Overview
Osteoporosis is the most common bone disease, affecting millions of people worldwide. It leads to weakened bones, increasing the risk of fractures, particularly in the forearm, spine, and hip. In developed countries, osteoporosis-related fractures affect around 30% of women and 12% of men. In the UK alone, more than 250,000 fractures occur each year, with an estimated treatment cost of £1.75 billion.
Hip fractures are considered the most serious, associated with an immediate mortality rate of around 12% and a 20% increase in long-term mortality. Osteoporosis is characterized by reduced bone density and micro-architectural deterioration of bone tissue, which increases fracture risk even with minor falls or stress. As age advances, bone density naturally declines, particularly in women, making osteoporosis more prevalent. The condition develops when new bone formation does not keep pace with the loss of existing bone.
Causes of Osteoporosis
Osteoporosis occurs when there is an imbalance between new bone formation and old bone resorption. This imbalance may result from insufficient new bone formation, excessive bone loss, or a combination of both. Key minerals such as calcium and phosphate are essential for healthy bone development. When calcium intake is inadequate or absorption is impaired, bone production is affected, leading to weaker and more fragile bones.
Hormonal changes are a major contributing factor, particularly a decline in estrogen in women and testosterone in men. Women over the age of 60, especially during and after menopause, are at a higher risk due to reduced estrogen levels. Additional contributing factors include:
Inadequate calcium and vitamin D intake
Lack of regular weight-bearing exercise
Age-related hormonal changes
Prolonged use of corticosteroids (e.g., in conditions such as Cushing syndrome)
Thyroid-related disorders
Reduced muscle use or prolonged immobility
Bone-related cancers
Certain genetic disorders
Long-term use of specific medications, including corticosteroids
Types of Osteoporosis and Their Causes
Osteoporosis is a condition in which bones become fragile and more prone to fractures. It can be classified based on the cause, age of onset, and factors contributing to bone loss. The main types of osteoporosis are outlined below:
1. Primary Osteoporosis
Primary osteoporosis develops without an identifiable underlying medical condition, most commonly due to aging or hormonal changes. It includes two subtypes:
Type 1 (Postmenopausal Osteoporosis):
Cause: A decline in estrogen levels after menopause, which directly affects bone density.
Characteristics: Mainly affects trabecular bone, especially in the spine and wrists, increasing fracture risk.
Onset: Typically seen in women aged 50 years and above following menopause.
Type 2 (Senile Osteoporosis):
Cause: Age-related bone loss in both men and women due to reduced bone formation and decreased calcium absorption.
Characteristics: Involves both cortical and trabecular bones and is often associated with long-term low bone mass.
Onset: Common after the age of 70, affecting both genders, with a higher prevalence in postmenopausal women.
2. Secondary Osteoporosis
Secondary osteoporosis occurs as a result of underlying medical conditions, long-term medication use, or lifestyle factors. Common causes include:
Medications:
Prolonged use of corticosteroids (e.g., prednisone), which can interfere with bone formation and calcium balance.
Certain anticonvulsants and chemotherapy agents that may affect bone health over time.
Endocrine Disorders:
Conditions such as hyperthyroidism, Cushing’s syndrome, and diabetes, which can contribute to reduced bone strength.
Lifestyle Factors:
Smoking and excessive alcohol consumption, both of which accelerate bone loss.
Nutritional deficiencies, particularly low calcium and vitamin D intake.
Other Medical Conditions:
Rheumatoid arthritis, gastrointestinal disorders (such as celiac disease), and chronic kidney disease, all of which may increase osteoporosis risk.
3. Idiopathic Osteoporosis
Idiopathic osteoporosis refers to cases where no clear cause can be identified.
Onset: May occur in younger individuals under 50 years of age.
Characteristics: Often detected after an unexpected fracture and can affect both men and women, with a possible genetic component.
4. Juvenile Osteoporosis
This is a rare form affecting children and adolescents.
Cause: May be related to genetic or metabolic disorders, or secondary to conditions such as juvenile arthritis.
Characteristics: Can present with frequent fractures, delayed growth, and impaired bone development.
5. Glucocorticoid-Induced Osteoporosis (GIOP)
This specific type of secondary osteoporosis results from long-term glucocorticoid use.
Mechanism: These medications reduce bone formation, increase calcium loss, and lower overall bone mass.
At Risk: Individuals receiving glucocorticoids for conditions such as asthma, rheumatoid arthritis, or lupus.
6. Osteoporosis Pseudoglioma Syndrome (OPGS)
OPGS is a rare genetic disorder characterized by early-onset osteoporosis and visual impairment.
Cause: Mutations in the LRP5 gene leading to weak bones and eye conditions such as pseudoglioma, which can result in vision loss.
Osteoporosis Symptoms and Fractures: What to Watch For and Natural Support Options
Osteoporosis is often referred to as a “silent disease” because it typically progresses without obvious symptoms until a fracture occurs. By the time signs appear, significant bone loss may have already taken place. Understanding the warning signs and types of fractures associated with osteoporosis can help in early identification and timely management.
Consultations for osteoporosis evaluation and long-term management are available at Spiritual Homeopathy Clinic, with multiple branches across Hyderabad, as well as online and international consultation options.
Common Symptoms and Signs of Osteoporotic Fractures
While osteoporosis itself may not cause noticeable discomfort in its early stages, fractures related to weakened bones can present with a range of symptoms depending on their location.
1. Spinal (Vertebral) Fractures
The spine is one of the most commonly affected areas in osteoporosis. Vertebral fractures may occur suddenly or develop gradually over time and can result in:
Sudden or persistent back pain
Gradual loss of height
Rounded or sloping shoulders
A hunched posture (kyphosis), often associated with long-term discomfort
These fractures may occur from minimal stress, such as bending forward, lifting light objects, or even coughing.
2. Acute Vertebral Fracture
When a vertebral fracture occurs abruptly, it may cause:
Sharp back pain that can radiate to the chest or abdomen
Discomfort sometimes mistaken for cardiac or digestive conditions
Pain that worsens with movement
Localized tenderness along the spine
Because these symptoms can resemble other medical conditions, proper clinical evaluation is important for accurate diagnosis and appropriate care.
3. Peripheral Osteoporotic Fractures (Limbs)
Fractures affecting the arms or legs often result from minor falls or low-impact injuries and may present with:
Localized pain and swelling
Visible deformity in the affected area
Pain following minimal trauma, such as slipping or bumping into furniture
These fractures commonly involve the wrist, forearm, or ankle.
4. Hip Fracture
Hip fractures are considered one of the more serious complications of osteoporosis, particularly in older adults. Common signs include:
Difficulty or inability to bear weight on the affected leg
Shortening of the leg on the fractured side
Outward rotation of the leg
Severe pain in the hip or groin region
Such fractures usually require prompt medical attention and may affect long-term mobility if not managed appropriately.
Natural and Holistic Support for Osteoporosis
Alongside conventional medical care, supportive natural approaches may help in maintaining bone health and reducing the risk of further complications. A homeopathy-based approach focuses on individualized care, addressing contributing factors such as age, lifestyle, nutritional status, and overall health.
Natural Support Strategies May Include:
Supporting bone regeneration: Gentle, individualized care may assist the body’s natural healing processes during fracture recovery.
Enhancing nutrient absorption: Holistic guidance may support better utilization of calcium and other essential nutrients.
Maintaining bone strength: Long-term management emphasizes minimizing further bone loss through lifestyle, dietary measures, and supportive care.
Homeopathic care is generally well-tolerated when guided by a qualified professional and is intended to complement, not replace, standard medical evaluation.
Diet for Osteoporosis: Nourishing Bones for Strength and Health
A nutrient-dense diet plays a pivotal role in supporting bone health, particularly for individuals with osteoporosis. A focus on foods rich in calcium, vitamin D, magnesium, protein, vitamin K, and omega-3 fatty acids can support bone strength and help reduce fracture risk. Dietary guidance is best tailored to individual needs, age, and overall health status. Below are key dietary recommendations for osteoporosis:
1. Calcium-Rich Foods for Bone Strength
Calcium is a vital mineral for bone structure. Adequate intake supports bone density and helps reduce bone weakening:
Dairy Products: Milk, yogurt, and cheese
Leafy Greens: Kale, collard greens, and bok choy
Fortified Foods: Almond or soy milk and fortified orange juice
Fish with Bones: Sardines and canned salmon
Tofu: Calcium-set tofu
Almonds and Figs: Naturally rich in calcium
2. Vitamin D-Rich Foods for Calcium Absorption
Vitamin D supports effective calcium absorption and utilization:
Fatty Fish: Salmon, mackerel, sardines
Egg Yolks: Moderate source
Fortified Foods: Fortified milk (dairy and plant-based), cereals, orange juice
Sunlight: Short, regular sunlight exposure supports natural vitamin D synthesis, depending on skin type and location
3. Magnesium-Rich Foods for Bone Metabolism
Magnesium helps regulate calcium balance and bone formation:
Leafy Greens: Spinach, kale, Swiss chard
Nuts and Seeds: Almonds, sunflower seeds, cashews
Whole Grains: Brown rice, quinoa, oats
Legumes: Beans, lentils, chickpeas
4. Protein-Rich Foods for Bone and Muscle Health
Adequate protein supports both muscle mass and bone structure:
Lean Meats: Chicken, turkey, lean beef
Fatty Fish: Salmon, tuna
Plant-Based Proteins: Tofu, tempeh, beans, lentils, quinoa
5. Vitamin K-Rich Foods for Bone Mineralization
Vitamin K plays a role in proper calcium regulation within bones:
Leafy Greens: Kale, spinach, Swiss chard
Cruciferous Vegetables: Broccoli, Brussels sprouts
Herbs: Parsley, basil
6. Omega-3 Fatty Acids for Bone and Joint Health
Omega-3 fatty acids help support joint comfort and overall bone health:
Fatty Fish: Salmon, sardines, mackerel
Nuts and Seeds: Walnuts, flaxseeds, chia seeds
7. Anti-Inflammatory Foods for Reducing Bone Loss
Managing inflammation may help slow bone loss:
Fruits: Berries, oranges, apples, cherries
Vegetables: Tomatoes, broccoli, sweet potatoes, bell peppers
Spices: Turmeric and ginger
8. Hydration for Bone Health
Adequate hydration supports nutrient transport and overall metabolic function, indirectly benefiting bone health.
Foods to Avoid for Osteoporosis
Certain dietary habits may negatively affect bone health:
Excessive Salt: Can increase calcium loss
Caffeine: High intake may increase calcium excretion
Alcohol: Excess consumption may interfere with bone formation
Soda: Cola beverages may affect calcium balance
Sugar: High intake may contribute to gradual bone loss
Regimen for Osteoporosis: Exercise and Lifestyle Habits for Stronger Bones
Along with diet, appropriate physical activity plays an important role in maintaining bone strength and reducing fall risk. Exercise routines should be adapted to individual fitness levels and medical conditions.
1. Weight-Bearing Exercises for Bone Support
These activities help stimulate bone maintenance:
Walking
Jogging (if joint health permits)
Hiking
Dancing
Stair climbing
2. Strength Training for Muscle Support
Stronger muscles help protect bones and improve stability:
Light weightlifting
Resistance band exercises
Bodyweight exercises such as squats and lunges
3. Balance and Flexibility Exercises to Prevent Falls
Improving balance is especially important in osteoporosis:
Tai Chi
Gentle yoga
Pilates
Simple standing balance exercises
4. Low-Impact Cardiovascular Exercises
These activities support heart health with minimal bone stress:
Swimming
Cycling
Elliptical training
Yoga and Lifestyle Support for Osteoporosis
The following yoga poses are commonly recommended as supportive practices to improve posture, balance, flexibility, and muscle strength in individuals with osteoporosis. These practices are intended to complement medical care and are not a replacement for clinical evaluation or treatment. Movements should be gentle and adapted to individual bone health and physical capacity.
1. Mountain Pose (Tadasana)
Benefits: Improves posture, strengthens the legs, and promotes balance.
How to Do It:
Stand tall with your feet hip-width apart, grounding evenly through both feet.
Engage your thighs, lift your chest, and keep the spine neutral.
Raise your arms overhead with palms facing inward, keeping shoulders relaxed.
Hold for 15–30 seconds with steady breathing.
2. Cat–Cow Pose (Marjaryasana–Bitilasana)
Benefits: Enhances spinal mobility and flexibility; may help ease back stiffness.
How to Do It:
Begin on hands and knees, wrists under shoulders and knees under hips.
Inhale and gently arch the back, lifting the head and tailbone (cow pose).
Exhale and round the spine, tucking the chin and pelvis (cat pose).
Repeat slowly for 5–10 rounds with controlled breathing.
3. Warrior II (Virabhadrasana II)
Benefits: Strengthens the legs, supports posture, and improves balance.
How to Do It:
Stand with feet wide apart, turning one foot outward and the other slightly inward.
Bend the front knee while extending arms parallel to the floor.
Keep the knee aligned over the ankle and gaze forward.
Hold for 20–30 seconds, then switch sides.
4. Tree Pose (Vrksasana)
Benefits: Enhances balance, focus, and lower limb strength.
How to Do It:
Stand upright and shift weight onto one leg.
Place the sole of the opposite foot on the inner calf or thigh (avoid the knee).
Bring palms together at the chest or raise arms overhead.
Hold for 20–30 seconds, then change sides.
5. Bridge Pose (Setu Bandhasana)
Benefits: Strengthens the back, gluteal muscles, and legs; supports spinal alignment.
How to Do It:
Lie on your back with knees bent and feet hip-width apart on the floor.
Press through the feet and gently lift the hips upward.
Keep shoulders grounded; hands may be clasped beneath the back if comfortable.
Hold for 15–30 seconds, then lower slowly.
6. Chair Pose (Utkatasana)
Benefits: Builds strength in the legs, core, and spine.
How to Do It:
Stand with feet together or hip-width apart.
Bend the knees as if sitting back into a chair, keeping weight in the heels.
Raise arms overhead while maintaining a long spine.
Hold for 15–30 seconds and return slowly to standing.
7. Downward-Facing Dog (Adho Mukha Svanasana)
Benefits: Lengthens the spine and strengthens the arms and legs.
How to Do It:
Start on hands and knees.
Lift hips upward, forming an inverted “V” shape.
Keep hands shoulder-width apart and feet hip-width apart.
Hold for 20–30 seconds with steady breathing.
8. Sphinx Pose (Salamba Bhujangasana)
Benefits: Gently strengthens the lower back and supports spinal posture.
How to Do It:
Lie on your stomach with forearms on the floor, elbows under shoulders.
Press forearms down and lift the chest slightly, lengthening the spine.
Keep hips and legs relaxed on the mat.
Hold for 20–30 seconds while breathing comfortably.
9. Child’s Pose (Balasana)
Benefits: Provides gentle spinal stretch and promotes relaxation.
How to Do It:
Kneel with toes together and knees apart.
Lower hips toward heels and extend arms forward.
Rest the forehead on the floor or a support.
Hold for 1–2 minutes in a relaxed position.
10. Cobra Pose (Bhujangasana)
Benefits: Strengthens the spine and opens the chest.
How to Do It:
Lie on your stomach with palms placed under the shoulders.
Gently press into the palms to lift the chest, keeping elbows slightly bent.
Avoid excessive back extension.
Hold for 15–20 seconds and release slowly.
🌿 Why Choose Homeopathy?
Homeopathy is a gentle, natural system of healthcare that focuses on addressing the underlying causes of illness rather than only treating symptoms. It works in harmony with the body’s innate healing ability and is suitable for all ages. Homeopathic care is individualized, aiming to support long-term health and overall well-being.
It can be applied for both chronic conditions and acute symptoms, providing a holistic and personalized approach to care.
🌟 Spiritual Homeopathy: Your Partner in Natural Healing
At Spiritual Homeopathy Clinic, we focus on supporting physical, emotional, and spiritual health. Our approach combines time-tested homeopathic principles with modern clinical insight, ensuring care that is personalized, careful, and safe.
We aim to identify underlying imbalances and address them thoughtfully, rather than simply suppressing symptoms.
💫 What Sets Spiritual Homeopathy Apart?
Our approach emphasizes:
Root-Cause Focus: Evaluating the factors behind your symptoms to support long-term wellness.
Personalized Care: Remedies and treatment plans are tailored to your body, lifestyle, and emotional state.
Experienced Team: Skilled homeopathy doctors in Hyderabad provide in-clinic, online, and international consultations.
Safe & Gentle: Homeopathic remedies are non-toxic and well-tolerated under professional guidance.
Holistic Perspective: Treatment integrates mind, body, and emotional aspects of health.
🔍 Our Treatment Process
🩺 1. Comprehensive Consultation
We carefully assess your health history, lifestyle, emotional state, and symptoms to create an individualized care plan.
💊 2. Homeopathic Remedies
We select natural remedies based on your specific condition. Care may support both acute illnesses and long-term health management.
🔄 3. Ongoing Support & Follow-Up
Regular follow-ups allow monitoring, adjustments, and guidance to ensure treatment aligns with your evolving health needs.
❤️ Our Commitment
Your health and well-being are our primary focus. We guide patients toward balanced health using professional, individualized, and supportive homeopathic care
When to Consult a Doctor
You should consult a healthcare professional if you are at risk of osteoporosis or notice symptoms that may indicate weakened bones. Early evaluation helps identify contributing factors and reduces the risk of fractures.
Seek consultation if you experience:
Frequent or unexplained back pain
Loss of height over time or a stooped posture
Fractures from minor falls or minor trauma
Difficulty moving or limited mobility due to bone pain
Bone pain that persists despite rest or basic care
Risk factors such as menopause, long-term steroid use, low calcium or vitamin D intake, or a family history of osteoporosis
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients who cannot visit in person. A professional assessment helps create an individualized care plan based on bone health, lifestyle, and overall well-being.
For appointments or guidance, contact 9069 176 176.
FAQ – Osteoporosis
What is osteoporosis?
Osteoporosis is a condition where bones become weak and brittle due to an imbalance between bone formation and bone loss. This increases the risk of fractures, particularly in the hip, spine, and wrist.What causes osteoporosis?
Common causes include aging, hormonal changes (such as menopause), low calcium and vitamin D intake, insufficient physical activity, smoking, excessive alcohol consumption, and certain medications like corticosteroids. These factors vary by individual and are assessed during consultation.Who is at risk of developing osteoporosis?
People over 50, postmenopausal women, individuals with a family history of osteoporosis, those with low body weight, and people with sedentary lifestyles are at higher risk.What are the symptoms of osteoporosis?
Osteoporosis is often called a “silent disease” because it usually shows no symptoms until a fracture occurs. Warning signs may include back pain, loss of height, stooped posture (kyphosis), and fractures from minor falls. Frequent or severe symptoms should prompt consultation with a healthcare professional.How is osteoporosis diagnosed?
The most common method is a DEXA scan (dual-energy X-ray absorptiometry), which measures bone mineral density (BMD) and compares it with expected bone density for age and gender.What foods help prevent or manage osteoporosis?
A balanced diet rich in calcium, vitamin D, magnesium, protein, and vitamin K supports bone health. Sources include dairy products, leafy greens, fortified foods, fatty fish, nuts, seeds, and legumes. Diet recommendations may vary depending on individual needs.Can osteoporosis be reversed?
Osteoporosis cannot usually be fully reversed, but its progression can be slowed or managed through lifestyle measures, nutrition, exercise, and professional care. Early detection improves outcomes.What are the best exercises for osteoporosis?
Weight-bearing exercises (walking, hiking, dancing) and resistance training (light weightlifting, resistance bands) help strengthen bones. Balance and flexibility exercises, such as yoga or tai chi, can reduce the risk of falls.Is osteoporosis painful?
Osteoporosis itself is generally not painful. Pain usually arises from fractures caused by weakened bones, especially in the spine, which can limit mobility and daily activity.What are the treatment options for osteoporosis?
Management may include nutritional guidance, lifestyle modifications, physical therapy, and homeopathic care under professional guidance. In some cases, conventional medical treatments or surgery may be considered after fractures.Can men get osteoporosis?
Yes. Although more common in women, men—particularly after age 70 or those with low testosterone or prolonged steroid use—can also develop osteoporosis.How can osteoporosis be prevented?
Prevention focuses on adequate calcium and vitamin D intake, regular physical activity, avoiding smoking and excess alcohol, and timely bone density assessments for at-risk individuals.