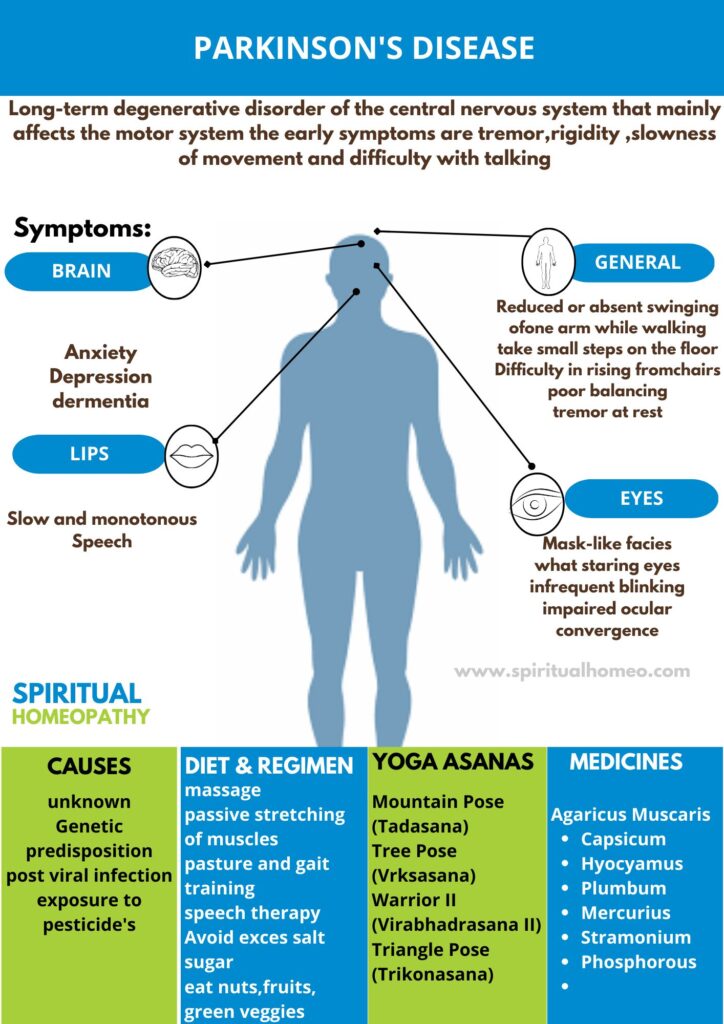
Parkinson’s Disease
Living with Parkinson’s Disease: Tips for Patients and Caregivers
- Home
- Parkinson’s Disease
Parkinson’s Disease
Effective Homeopathic Treatment for Parkinson's Disease
Discover everything you need to know about Parkinson’s disease, including early symptoms, common causes, how it’s diagnosed, and the latest treatment options. Learn how to manage Parkinson’s effectively and improve quality of life.
Everything You Need to Know
Overview
Who Is Affected by Parkinson’s Disease?
Parkinson’s disease (PD) can affect individuals of any gender, race, occupation, or nationality. It is more commonly seen in older adults, with the average age of onset around 60 years. However, young-onset Parkinson’s disease can also occur, affecting individuals in their 20s or younger.
The risk of developing Parkinson’s disease increases with age, but it is not limited to the elderly population. Genetic factors, environmental influences, and overall neurological health may also play a role in disease development, which can vary from person to person.
Causes and Risk Factors of Parkinson’s Disease
Most cases of Parkinson’s disease (approximately 85–90%) occur sporadically, meaning they develop without a clearly identifiable cause. The exact reason why Parkinson’s disease develops in most individuals remains unclear. Current research suggests that a combination of genetic susceptibility and environmental influences may contribute to its onset.
🧬 Genetic vs. Environmental Factors
Genetic factors appear to play a more significant role in individuals who develop Parkinson’s disease at a younger age.
In people over the age of 50, environmental exposures are believed to have a stronger influence.
Twin studies support this age-related difference in the origin of Parkinson’s disease.
🌱 Environmental Risk Factors
Epidemiological studies have identified several factors that may be associated with an increased or decreased risk of developing Parkinson’s disease:
Factors associated with increased risk:
Long-term exposure to pesticides
Living in rural areas
Consumption of well water
Factors associated with decreased risk:
Cigarette smoking (not recommended as a preventive approach)
Caffeine consumption
⚠️ Note: While these associations have been observed, no single environmental factor has been definitively proven to cause typical Parkinson’s disease.
🦠 Viral Infections and Parkinsonism
In rare cases, viral infections can lead to a condition known as post-encephalitic Parkinsonism, which differs from typical Parkinson’s disease. This form may develop after encephalitis (inflammation of the brain) and was notably observed following viral outbreaks such as the 1918 influenza pandemic.
Types of Parkinson’s Disease: Symptoms, Causes & Progression
Parkinson’s disease (PD) is a progressive neurodegenerative disorder that primarily affects movement, but it may also influence cognition, mood, and daily functioning over time. There are several recognized types of Parkinson’s disease, each with distinct characteristics, patterns of onset, and progression. Understanding these differences supports accurate diagnosis and appropriate long-term care planning.
🔹 1. Idiopathic Parkinson’s Disease (IPD)
This is the most common form of Parkinson’s disease, accounting for approximately 85–90% of cases.
Cause: Unknown (idiopathic), though a combination of genetic susceptibility and environmental factors may play a role.
Symptoms: Typical motor features include tremors, bradykinesia (slowness of movement), muscle rigidity, and postural instability.
Onset: Usually begins after the age of 60 and progresses gradually.
🔹 2. Early-Onset Parkinson’s Disease (EOPD)
This form of Parkinson’s disease develops before the age of 50 and often has a stronger genetic association.
Symptoms: Similar to idiopathic Parkinson’s disease but may progress more slowly.
Genetic link: Genetic variations may be more commonly involved.
Prognosis: Longer disease duration due to earlier onset.
🔹 3. Atypical Parkinsonism (Parkinson’s Plus Syndromes)
These conditions resemble Parkinson’s disease but have additional neurological features and typically progress more rapidly. Common subtypes include:
▪ Multiple System Atrophy (MSA)
Involves autonomic dysfunction such as blood pressure instability, bladder issues, and coordination problems.
Often shows limited response to conventional Parkinson’s treatments.
▪ Progressive Supranuclear Palsy (PSP)
Characterized by balance problems, frequent falls, and difficulty with eye movements.
Usually progresses faster with earlier functional impairment.
▪ Corticobasal Degeneration (CBD)
Presents with asymmetric motor symptoms, muscle stiffness, and cognitive changes.
Often affects one side of the body more prominently.
🔹 4. Genetic Parkinson’s Disease
Some cases of Parkinson’s disease are directly linked to inherited genetic mutations.
Symptoms: Generally similar to idiopathic Parkinson’s disease.
Presentation: May occur as early-onset or typical Parkinson’s disease depending on the genetic background.
🔹 5. Vascular Parkinsonism
This type results from reduced blood flow to certain areas of the brain, commonly due to strokes or small vessel disease.
Symptoms: Gait disturbances, slowness, and difficulty with balance.
Progression: May progress differently from idiopathic Parkinson’s disease and is often influenced by vascular health.
🔹 6. Drug-Induced Parkinsonism
Certain medications can lead to Parkinson-like symptoms by affecting dopamine pathways.
Symptoms: Tremor, stiffness, and slowed movements.
Course: Symptoms may improve after identifying and discontinuing the triggering medication under medical supervision.
🔹 7. Toxic Parkinsonism
This form is associated with prolonged exposure to environmental toxins.
Symptoms: Similar to those of typical Parkinson’s disease.
Causes: Long-term exposure to substances such as pesticides, heavy metals, or industrial chemicals.
🔹 8. Parkinson’s Disease Dementia (PDD)
A complication that may develop in later stages of Parkinson’s disease.
Symptoms: Memory impairment, confusion, executive dysfunction, and mood changes.
Progression: Usually appears after several years of motor symptoms and can significantly affect daily functioning.
Common Symptoms of Parkinson’s Disease
Parkinson’s disease (PD) is a progressive neurological disorder marked by both motor and non-motor symptoms. Understanding these signs is important for early recognition and supportive management. The following is a structured overview of commonly observed symptoms.
🔄 Tremor (Shaking)
Often the first noticeable symptom, usually beginning in one upper limb.
Typically a resting tremor, often described as a “pill-rolling” movement of the fingers.
May involve the head or lower limbs in some individuals.
Commonly reduces during voluntary movement and disappears during sleep.
🪵 Rigidity (Stiff Muscles)
Often described as uniform muscle stiffness affecting both flexor and extensor muscles.
When tremor is present, stiffness may feel jerky during movement.
Can affect posture, joint mobility, and the ability to perform daily activities.
🐢 Bradykinesia (Slowness of Movement)
Considered a core motor feature of Parkinson’s disease.
Involves reduced speed, range, and fluidity of movements.
Common observations include:
Reduced facial expression (mask-like face)
Infrequent blinking and limited eye movement
Soft, slow, or monotone speech
Small, cramped handwriting
Reduced arm swing while walking
Short, rapid steps with a forward-leaning posture
🧍♂️ Postural Instability (Balance Problems)
Difficulty maintaining balance and upright posture.
May struggle with movements such as standing up from a chair or turning in bed.
Impaired balance recovery can increase the risk of falls, especially in later stages.
🚶 Gait Disturbances (Walking Difficulties)
Early sign may include reduced arm swing on one side.
As the condition progresses:
Shortened stride and stiff trunk
Turning the whole body rather than rotating the torso
Episodes of “freezing,” where movement temporarily stops
Shuffling steps with a forward-bent posture
Walking pattern usually remains narrow-based.
🧠 Non-Motor Symptoms
🔸 Pain
May present as deep aching, cramping, or discomfort.
Can occur independently or in association with muscle stiffness and posture changes.
🔸 Mental Health and Cognitive Changes
Anxiety and depression are frequently reported.
Cognitive changes may appear in later stages, including memory difficulties, reduced motivation, or visual disturbances.
🔸 Postural Hypotension
A drop in blood pressure on standing, leading to dizziness, fatigue, or unsteadiness.
May be related to disease progression or treatment effects.
🔸 Dyskinesia
Involuntary movements affecting limbs or the trunk.
Often associated with long-term management of Parkinson’s disease.
If these symptoms become noticeable, progressive, or begin to interfere with daily activities, professional evaluation is advised to support timely care planning.
Healthy Eating Tips for a Balanced Diet
Maintaining a balanced diet is key to supporting overall health, sustaining daily energy levels, and reducing the risk of long-term lifestyle-related conditions. The following practical nutrition tips can help support healthier food choices as part of daily routine.
🥗 1. Load Up on Fruits and Vegetables
Aim for at least five servings of fruits and vegetables each day. Include a variety of naturally colorful options such as spinach, carrots, berries, and bell peppers, which provide essential vitamins, minerals, and antioxidants that support body functions.
🌾 2. Choose Whole Grains Over Refined Grains
Replacing refined grains with whole grains supports digestion and heart health due to higher fiber and nutrient content. Consider options such as:
Whole wheat bread
Brown rice
Oatmeal
Quinoa
🥩 3. Limit Red and Processed Meats
Reducing intake of red meats like beef, pork, lamb, and goat, and avoiding processed meats such as sausages, hot dogs, and bologna, may support long-term health. Instead, include lean protein sources such as:
Fish
Skinless poultry
Beans and legumes
Eggs
🥑 4. Choose Healthy Fats
Including moderate amounts of healthy fats can support overall nutrition. Prefer sources such as:
Olive oil
Nuts (almonds, walnuts, pecans)
Trans fats and partially hydrogenated oils, commonly found in packaged and fast foods, should be limited.
🥤 5. Cut Back on Sugary Drinks and Sweets
Sugar-sweetened beverages such as soft drinks and packaged fruit juices contribute excess calories without nutritional benefit. Desserts and sweets are best limited to occasional consumption to support balanced blood sugar and weight management.
🧂 6. Reduce Sodium Intake
Excess salt intake may affect blood pressure and cardiovascular health. Helpful steps include:
Reading nutrition labels for sodium content
Choosing low-sodium options where possible
Limiting canned, processed, and ready-to-eat meals
🍽️ 7. Watch Portions and Eat Mindfully
Practicing portion control and mindful eating supports digestion and helps recognize natural hunger and fullness signals. Eating slowly and stopping when comfortably satisfied can prevent overeating.
Yoga & Lifestyle Support for Paralysis
Yoga and supportive lifestyle practices may help improve flexibility, balance, circulation, and overall well-being in individuals affected by paralysis. These practices are intended to be supportive in nature and should be performed only under professional guidance, based on individual ability and medical condition. Yoga is not a replacement for medical evaluation or treatment.
1. Tadasana (Mountain Pose)
Benefits: Improves posture and stability, and helps strengthen the legs and core muscles.
How to do it: Stand straight with feet together and arms at the sides. Inhale and raise the arms overhead, gently lifting the heels off the floor. Hold for a few seconds, then exhale and lower slowly. Support may be used if balance is limited.
2. Vrikshasana (Tree Pose)
Benefits: Enhances balance, coordination, and concentration.
How to do it: Stand on one leg and place the other foot on the inner thigh or calf (avoid the knee). Bring hands to a prayer position at the chest. Use wall or chair support as needed.
3. Marjariasana–Bitilasana (Cat–Cow Pose)
Benefits: Improves spinal flexibility, coordination, and helps reduce stiffness.
How to do it: From a hands-and-knees position, gently alternate between arching the back (cow pose) and rounding the spine (cat pose) while coordinating movement with breathing.
4. Adho Mukha Svanasana (Downward-Facing Dog)
Benefits: Builds upper and lower body strength and stretches the spine and limbs.
Modification: If the full pose is difficult, practice with hands supported on a wall or elevated surface to reduce strain.
5. Utkatasana (Chair Pose)
Benefits: Strengthens leg muscles and improves body awareness.
How to do it: Bend the knees and lower the hips as if sitting on a chair, keeping the arms raised. Hold briefly. A chair or wall may be used for added support.
6. Setu Bandhasana (Bridge Pose)
Benefits: Strengthens the back and hips and supports healthy circulation.
How to do it: Lie on your back with knees bent and feet flat on the floor. Slowly lift the hips while pressing the feet into the ground. Hold briefly and lower gently.
7. Shavasana (Corpse Pose)
Benefits: Promotes deep relaxation, stress relief, and breath awareness.
How to do it: Lie comfortably on your back with arms at the sides and eyes closed. Focus on slow, relaxed breathing.
Optional Supportive Practices
Pranayama (Breathing Exercises): Techniques such as Anulom Vilom and Bhramari may help calm the nervous system and support mental relaxation.
Meditation: Mindfulness or guided meditation can assist in reducing anxiety and improving mental clarity during recovery or long-term management.
🌿 Why Choose Homeopathy?
Homeopathy is a system of complementary medicine that focuses on understanding the individual as a whole, rather than addressing symptoms alone. It aims to support the body’s natural healing responses by considering physical, emotional, and lifestyle factors. When guided by a qualified professional, homeopathy is commonly used across different age groups and health concerns as part of long-term health management.
Homeopathy may be considered for both chronic conditions and acute concerns, with care plans tailored to individual needs and health backgrounds.
🌟 Spiritual Homeopathy Clinic: Our Approach to Care
At Spiritual Homeopathy Clinic, care is centered on understanding each patient’s overall health profile, including physical symptoms, emotional well-being, and lifestyle influences. The clinical approach combines classical homeopathic principles with structured case evaluation and follow-up.
Consultations are available across multiple branches in Hyderabad, as well as through online and international consultation services, allowing continuity of care regardless of location.
💫 Why Consider Care at Spiritual Homeopathy Clinic?
Our approach emphasizes individualized assessment and thoughtful case management. Key aspects include:
Root-Cause Assessment: Focus on identifying contributing factors rather than addressing symptoms alone
Personalized Care: Treatment plans are tailored to the individual’s constitution, lifestyle, and health history
Qualified Medical Team: Experienced homeopathy practitioners offering in-clinic and online consultations
Professional Guidance: Care is planned and monitored under clinical supervision
Holistic Perspective: Attention is given to physical, emotional, and supportive lifestyle factors
🔍 Our Treatment Process
🩺 1. In-Depth Consultation
Each consultation involves a detailed discussion of medical history, current concerns, lifestyle patterns, and emotional factors. This comprehensive assessment helps guide individualized care planning.
🔄 2. Individualized Care Planning
Based on the consultation, a personalized approach is developed to support long-term management. The focus remains on addressing contributing factors and monitoring progress over time.
🔁 3. Follow-Up and Review
Regular follow-ups help assess response, track changes, and adjust the care plan as required. Ongoing review is an important part of responsible case management.
❤️ Commitment to Patient Care
Spiritual Homeopathy Clinic emphasizes ethical practice, clear communication, and patient-centered care. Individuals are guided with professionalism and sensitivity, with attention to safety, realistic expectations, and continuity of care.
When to Consult
You should consult a healthcare professional if Parkinson’s disease symptoms appear, worsen, or begin to interfere with daily activities, work, or independence. Early evaluation helps in understanding symptom patterns, ruling out other conditions, and planning appropriate long-term management.
Seek consultation if you experience:
Persistent or increasing tremors in the hands, legs, or jaw
Slowness of movement or difficulty initiating movements
Muscle stiffness or rigidity affecting mobility
Problems with balance, frequent falls, or unsteady walking
Changes in speech, handwriting, or facial expressions
Sleep disturbances, mood changes, anxiety, or depression
Symptoms that gradually progress or affect daily functioning
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for individuals who are unable to visit the clinic in person. A professional assessment helps support an individualized care approach based on symptoms, stage of the condition, and overall health status.
For appointments or guidance, contact 9069 176 176.
FAQS
1. What is Parkinson’s Disease?
Parkinson’s Disease (PD) is a progressive neurological disorder that mainly affects movement. It develops when nerve cells in the brain responsible for producing dopamine gradually become impaired, leading to movement-related symptoms.
2. What causes Parkinson’s Disease?
In most cases, the exact cause is unknown. Contributing factors may include genetic susceptibility, environmental exposures, aging, and, in some individuals, inherited genetic changes. The condition often results from a combination of factors rather than a single cause.
3. What are the early signs of Parkinson’s Disease?
Early symptoms may include:
Tremors (shaking) in the hands or fingers
Slowness of movement (bradykinesia)
Muscle stiffness or rigidity
Small or cramped handwriting
Reduced facial expressions or blinking
Early evaluation is advised if these symptoms are persistent or progressive.
4. Is Parkinson’s Disease curable?
Parkinson’s Disease currently has no definitive cure. However, available medical and supportive approaches can help manage symptoms, maintain function, and improve quality of life over time under professional care.
5. Who is at risk for Parkinson’s Disease?
The risk increases with age, particularly after 60 years. Men are slightly more affected than women. Family history, prior head injuries, and exposure to certain environmental toxins may also increase risk.
6. What are the main symptoms of Parkinson’s Disease?
Common symptoms include:
Resting tremors
Muscle rigidity
Slowed movements
Balance and coordination difficulties
Changes in speech and handwriting
Non-motor symptoms such as sleep disturbances, mood changes, or anxiety
7. How is Parkinson’s Disease diagnosed?
There is no single diagnostic test for Parkinson’s Disease. Diagnosis is primarily based on medical history, symptom evaluation, and neurological examination. Imaging studies may be used to exclude other conditions when required.
8. What treatment options are available for Parkinson’s Disease?
Management may involve a combination of approaches, including:
Medical management under neurological supervision
Physical, occupational, and speech therapy
Supportive lifestyle measures such as regular exercise and structured routines
Treatment plans are individualized based on symptoms and overall health status.
9. Can diet or exercise help with Parkinson’s Disease?
Yes. A balanced diet that supports digestion and nutrition, along with regular physical activity, may help maintain mobility, balance, and overall well-being. Lifestyle guidance should be adapted to individual tolerance and needs.
10. Is Parkinson’s Disease fatal?
Parkinson’s Disease itself is not usually life-threatening. However, complications such as falls, infections, or swallowing difficulties may occur in advanced stages. With appropriate medical care and monitoring, many individuals live for years after diagnosis.