Pneumonia
Pneumonia Explained: Symptoms, Causes, Treatment, and Prevention Tips
- Home
- Pneumonia
Pneumonia
Effective Homeopathic Treatment for Pneumonia
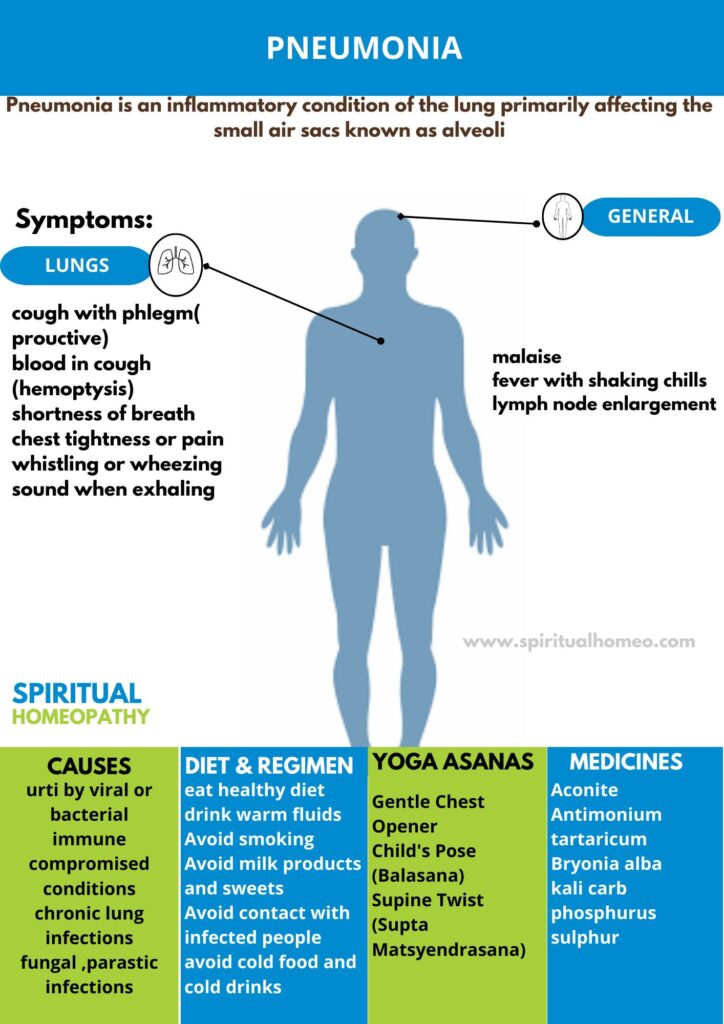
Pneumonia is a serious lung infection that causes inflammation in the alveoli, the tiny air sacs in the lungs. This condition can result from bacterial, viral, or fungal infections, leading to symptoms such as cough, fever, difficulty breathing, and chest pain. Pneumonia can range from mild to severe and may require hospitalization in more serious cases. Early diagnosis and proper treatment are essential for managing pneumonia and preventing complications, especially in high-risk groups like the elderly and those with weakened immune systems.
Everything You Need to Know
Overview
Pneumonia is primarily caused by viral or bacterial infections, though other microorganisms can also be responsible. Diagnosing pneumonia can be challenging, as it often relies on symptoms, physical examination, and diagnostic tools such as chest X-rays, blood tests, and sputum cultures. Pneumonia may be classified into community-acquired, hospital-acquired, or healthcare-associated types. Affecting an estimated 450 million people globally each year, pneumonia remains a significant cause of illness and mortality, particularly among older adults, young children, and individuals with chronic health conditions. Despite improvements in outcomes due to antibiotics and vaccination programs, pneumonia continues to be an important public health concern worldwide.
Predisposing Factors for Pneumonia
Several factors can increase the risk of developing pneumonia, including smoking, immunodeficiency, alcoholism, chronic obstructive pulmonary disease (COPD), asthma, chronic kidney disease, liver disease, and biological aging. In children, additional risks include lack of breastfeeding, exposure to secondhand smoke, malnutrition, and socioeconomic challenges. The use of acid-suppressing medications such as proton-pump inhibitors or H2 blockers may also increase susceptibility. People on mechanical ventilation are particularly prone to ventilator-associated pneumonia, while those with gastric feeding tubes have a higher risk of aspiration pneumonia. Genetic variations can further influence an individual’s susceptibility to pneumonia and its complications.
Understanding these factors helps guide an individualized care approach based on overall health status and risk profile.
Pneumonia Infection Causes
Bacterial Pneumonia
Bacterial infections are the most common cause of community-acquired pneumonia (CAP). Streptococcus pneumoniae accounts for a significant proportion of cases, while Haemophilus influenzae, Chlamydophila pneumoniae, and Mycoplasma pneumoniae are also frequently identified. Drug-resistant strains, including drug-resistant Streptococcus pneumoniae (DRSP) and methicillin-resistant Staphylococcus aureus (MRSA), are increasingly reported in clinical settings.
Organism Spread
Certain risk factors promote the spread of pneumonia-causing organisms. Alcoholism is commonly associated with Streptococcus pneumoniae, anaerobic organisms, and Mycobacterium tuberculosis. Smoking facilitates infections caused by Streptococcus pneumoniae, Haemophilus influenzae, Moraxella catarrhalis, and Legionella pneumophila. Exposure to birds increases the risk of Chlamydia psittaci, while contact with farm animals is linked to Coxiella burnetii. Aspiration pneumonia is often caused by anaerobic organisms, and cystic fibrosis increases susceptibility to Pseudomonas aeruginosa and Staphylococcus aureus infections.
Viral Pneumonia
Viruses account for approximately one-third of pneumonia cases in adults and about 15% in children. Common viral causes include rhinoviruses, coronaviruses, influenza virus, respiratory syncytial virus (RSV), and adenovirus. Herpes simplex virus may cause pneumonia in immunocompromised individuals, such as those undergoing cancer treatment or organ transplantation. In people with weakened immune systems, cytomegalovirus (CMV) pneumonia is more frequently observed.
Secondary Infections
Viral respiratory infections can predispose individuals to secondary bacterial infections. Streptococcus pneumoniae, Staphylococcus aureus, and Haemophilus influenzae are commonly involved. During influenza seasons, viral pneumonia and related secondary infections tend to increase.
Fungal Pneumonia
Fungal pneumonia is uncommon but occurs more frequently in individuals with compromised immune systems, including those with HIV/AIDS or those receiving immunosuppressive therapy. Common causative organisms include Histoplasma capsulatum, Blastomyces, Cryptococcus neoformans, Pneumocystis jiroveci (PCP), and Coccidioides immitis. In people living with HIV/AIDS, PCP remains a notable opportunistic infection.
Parasitic Pneumonia
Parasites such as Toxoplasma gondii, Strongyloides stercoralis, Ascaris lumbricoides, and Plasmodium malariae can involve the lungs. These organisms typically enter the body through the skin, ingestion, or insect vectors. Parasitic pneumonia is more common in immunodeficient individuals and in those who have lived in or traveled to endemic regions.
Noninfectious Pneumonia
Noninfectious pneumonia includes conditions such as idiopathic interstitial pneumonia, organizing pneumonia, and other interstitial lung diseases. These may involve nonspecific interstitial pneumonia, lymphocytic interstitial pneumonia, and desquamative interstitial pneumonia. Lipoid pneumonia, caused by lipid material entering the lungs through inhalation or systemic spread, is a rare noninfectious form.
Pneumonia is sometimes referred to as “the old man’s friend” because, in frail or terminally ill individuals, it has historically been observed to shorten prolonged suffering. Clinically, pneumonia is classified based on how and where it is acquired, as well as the area of the lungs involved. Understanding these classifications helps in assessment, anticipating possible complications, and planning appropriate care.
Types of Pneumonia Based on Acquisition
Community-Acquired Pneumonia (CAP)
Community-acquired pneumonia occurs outside healthcare settings. It is generally less likely to involve multidrug-resistant bacteria compared to healthcare-associated forms. However, drug-resistant strains can still be present, though they are less common in CAP.
Healthcare-Associated Pneumonia (HCAP)
Healthcare-associated pneumonia is linked to recent exposure to healthcare environments such as hospitals, outpatient clinics, nursing homes, dialysis centers, or home care services. Also known as medical care–associated pneumonia (MCAP), it may involve more resistant organisms due to repeated healthcare contact.
Hospital-Acquired Pneumonia (HAP)
Hospital-acquired pneumonia develops during hospitalization, usually 48 hours or more after admission. It often involves multidrug-resistant bacteria and commonly affects individuals with underlying medical conditions or weakened immunity.
Ventilator-Associated Pneumonia (VAP)
Ventilator-associated pneumonia occurs in patients receiving mechanical ventilation. It is defined as pneumonia developing 48–72 hours after endotracheal intubation. VAP carries higher risks due to resistant organisms and direct airway instrumentation.
Types of Pneumonia Based on Lung Area Affected
Lobar Pneumonia
Lobar pneumonia affects a single lobe of the lung. It is typically localized and commonly associated with Streptococcus pneumoniae.
Bronchial Pneumonia
Bronchial pneumonia presents as patchy areas of infection scattered throughout the lungs, often involving the smaller airways.
Acute Interstitial Pneumonia
This form affects the interstitial tissues of the lungs and may progress rapidly, often presenting with more severe symptoms.
Pneumonia in Children
In children, pneumonia is also classified according to the severity of symptoms, which guides clinical decision-making:
Non-severe
Severe
Very severe
Early evaluation is advised if symptoms are persistent, worsening, or associated with breathing difficulty.
General Symptoms of Pneumonia
Productive Cough: Coughing up mucus or sputum is a common feature.
Fever and Chills: Fever accompanied by chills or shaking is frequently reported.
Shortness of Breath: Difficulty breathing or a sensation of breathlessness may occur, especially with activity.
Sharp Chest Pain: Chest pain, often sharp or stabbing, can be felt while taking deep breaths or coughing.
Increased Breathing Rate: Rapid or labored breathing may indicate lung involvement.
Persistent or worsening symptoms should be medically evaluated to assess severity and possible complications.
Symptoms in Older Adults
In older adults, pneumonia may present atypically. Confusion or altered mental status can be more prominent than fever or cough and should not be overlooked.
Symptoms in Children
Under Five Years Old: Fever, cough, and rapid or difficult breathing are commonly observed.
Under Two Months Old: Infants may not show a cough, but fever, poor feeding, and breathing difficulty may still be present.
Severe Symptoms in Children
In more serious cases, children may develop:
Blue-tinged skin (cyanosis)
Refusal to drink or feed
Convulsions
Ongoing vomiting
Extreme temperature changes
Decreased level of consciousness
Immediate medical attention is advised if these signs are noticed.
Specific Types of Pneumonia and Their Symptoms
Legionella Pneumonia: Along with typical respiratory symptoms, abdominal pain, diarrhea, or confusion may be present.
Streptococcus pneumoniae: This form may cause rust-colored sputum.
Klebsiella Pneumonia: Can produce thick, blood-tinged sputum and may indicate more severe infection.
Tuberculosis and Other Causes: Hemoptysis (bloody sputum) can be seen in tuberculosis, certain Gram-negative pneumonias, lung abscesses, and acute bronchitis.
Mycoplasma Pneumonia: May be associated with swollen neck lymph nodes, joint pain, or middle ear symptoms.
Viral Pneumonia: Often presents with wheezing and milder sputum production compared to bacterial pneumonia.
Best Diet for Pneumonia Recovery
1. Stay Well Hydrated
Why it matters: Hydration helps thin mucus, making it easier to clear from the lungs and supports overall respiratory function.
What to drink:
Water: Aim for 8–10 glasses daily.
Herbal teas: Ginger, chamomile, and peppermint may help soothe the throat.
Broths: Chicken or vegetable broth provides fluids and nutrients.
Fresh juices: Vitamin C–rich options like orange or lemon juice, taken in moderation.
Coconut water: Helps replenish electrolytes.
2. Increase Protein Intake
Why it matters: Protein supports tissue repair, immune function, and strength during recovery.
Protein-rich foods:
Lean meats such as chicken or turkey
Fatty fish like salmon, tuna, or mackerel
Eggs
Low-fat dairy products
Plant-based proteins including lentils, beans, tofu, and tempeh
3. Eat Foods High in Vitamin C
Why it matters: Vitamin C contributes to immune defense and recovery.
Foods to include:
Citrus fruits (oranges, lemons, grapefruits)
Bell peppers
Kiwis and strawberries
Leafy greens such as spinach, kale, and broccoli
4. Add Anti-Inflammatory Foods
Why it matters: Lung inflammation is common in pneumonia, and certain foods may help support recovery.
Helpful options:
Fatty fish rich in omega-3 fats
Olive oil
Spices such as turmeric and ginger
Berries like blueberries, raspberries, and blackberries
5. Boost Zinc Intake
Why it matters: Zinc supports immune function and tissue healing.
Zinc-rich foods:
Shellfish
Lean red meat (in moderation)
Poultry
Legumes
Nuts and seeds
6. Focus on Easy-to-Digest Foods
Why it matters: Fatigue or reduced appetite is common, and gentle foods help maintain nutrition.
Suitable choices:
Soups and broths
Steamed vegetables
Bananas
Oatmeal or porridge
7. Increase Fiber Intake
Why it matters: Reduced activity and illness can affect digestion; fiber supports gut health.
High-fiber options:
Whole grains
Fruits and vegetables
Legumes
8. Get Adequate Vitamin A
Why it matters: Vitamin A supports lung tissue health and immune balance.
Food sources:
Carrots and sweet potatoes
Leafy greens
Eggs and dairy products
Dietary recommendations may vary based on age, severity of illness, and overall health, and should be adjusted individually.
Supportive Regimen for Recovering from Pneumonia
1. Prioritize Rest and Sleep
Adequate rest supports immune recovery. Aim for sufficient nighttime sleep and short daytime rest periods if needed.
2. Practice Breathing Exercises
Gentle breathing techniques may help improve lung expansion and comfort. Diaphragmatic and pursed-lip breathing are commonly advised under guidance.
3. Stay Active—Gently
Light activity such as short walks or simple stretches can support circulation when tolerated.
4. Follow Medical Advice Carefully
Adhere to professional guidance and report any new or worsening symptoms, such as increasing breathlessness or chest discomfort.
5. Avoid Smoking and Pollutants
Smoke and airborne irritants can delay recovery. Maintaining clean, well-ventilated indoor air is helpful.
6. Monitor Symptoms
Track fever, breathing patterns, fatigue, and chest pain to identify changes early.
7. Manage Stress
Stress can affect immune response. Relaxation practices and a calm environment may support recovery.
🧘♂️ Yoga Asanas for Pneumonia Recovery
The following yoga practices are supportive measures during pneumonia recovery. They are intended to complement medical care and should be practiced gently, based on individual strength and comfort.
1. Sukhasana (Easy Pose) with Deep Breathing
Benefits: Enhances lung capacity, calms the mind, and supports slow, conscious breathing.
How to do it:
Sit cross-legged with a straight spine.
Close your eyes and place your hands on your knees.
Inhale deeply through the nose, expanding the lungs.
Exhale slowly through the nose or pursed lips.
Repeat for 5–10 minutes.
2. Bhujangasana (Cobra Pose)
Benefits: Opens the chest, stretches the lungs, and supports oxygen intake.
How to do it:
Lie on your stomach with palms under the shoulders.
Inhale and gently lift your chest using the back muscles.
Keep elbows close to the body and avoid strain.
Hold for 10–15 seconds, then release.
Note: Avoid this pose if there is marked fatigue, breathlessness, or chest discomfort.
3. Setu Bandhasana (Bridge Pose)
Benefits: Opens the chest, improves circulation, and gently activates the lungs.
How to do it:
Lie on your back with knees bent and feet flat on the floor.
Inhale and lift the hips while keeping shoulders relaxed on the mat.
Hold for a few breaths and slowly lower down.
4. Matsyasana (Fish Pose – Supported)
Benefits: Expands the chest and lungs and helps relieve respiratory muscle tension.
How to do it:
Lie on your back with a rolled towel or cushion under the upper back.
Allow the head to rest back comfortably.
Breathe slowly and deeply for 1–2 minutes.
5. Adho Mukha Svanasana (Downward-Facing Dog – Gentle Version)
Benefits: Improves circulation and provides a mild stretch to the chest and lungs.
How to do it:
From an all-fours position, lift the hips gently into an inverted V-shape.
Keep knees slightly bent if required.
Maintain slow breathing for 30 seconds to 1 minute.
6. Balasana (Child’s Pose)
Benefits: Promotes relaxation, reduces tension in the chest and back, and supports deep breathing.
How to do it:
Sit on your heels and fold forward, extending arms or resting them by your sides.
Place the forehead on the mat or a cushion.
Breathe calmly for 1–3 minutes.
7. Viparita Karani (Legs-Up-the-Wall Pose)
Benefits: Helps reduce fatigue, calms the nervous system, and supports gentle circulation.
How to do it:
Lie on your back with legs resting up against a wall.
A pillow may be placed under the hips for comfort.
Relax and breathe deeply for 5–10 minutes.
🌬️ Pranayama (Breathing Exercises)
1. Anulom Vilom (Alternate Nostril Breathing)
Supports: Balanced breathing, oxygenation, and mental calmness.
2. Bhramari (Bee Breathing)
Supports: Relaxation of the nervous system and controlled exhalation.
Important: Fast or forceful breathing techniques (such as Kapalabhati or Bhastrika) should be avoided during active illness or early recovery. Yoga and breathing exercises are supportive practices and not a substitute for medical evaluation.
🌿 Why Choose Homeopathy?
Homeopathy is a system of care that focuses on understanding the individual as a whole rather than addressing symptoms alone. It aims to support the body’s natural healing responses by considering physical, emotional, and lifestyle factors. When guided by a qualified professional, homeopathic care is generally well-tolerated and may be used across different age groups as part of a long-term management approach.
Homeopathy may be considered for both acute and chronic conditions, with care plans adapted to individual health needs and overall constitution.
🌟 Spiritual Homeopathy Clinic: Approach to Care
At Spiritual Homeopathy Clinic, patient care is guided by established homeopathic principles along with careful clinical assessment. The focus remains on identifying contributing factors and patterns related to illness, rather than symptom control alone.
Consultations are available across multiple branches in Hyderabad, as well as through online and international consultation services, allowing continuity of care for patients in different locations.
💫 Our Clinical Approach
The care model emphasizes personalized evaluation and ongoing monitoring. Key aspects include:
Individualized Care: Each patient is assessed based on their medical history, current symptoms, lifestyle, and overall health profile.
Addresses Contributing Factors: Treatment planning considers factors that may influence disease progression or recovery.
Long-Term Management: Follow-up consultations help guide adjustments based on response and recovery patterns.
Professional Guidance: Homeopathic care is provided under professional supervision to ensure responsible and appropriate use.
🔍 Our Consultation Process
🩺 1. Detailed Case Assessment
The initial consultation involves a structured discussion covering health history, symptom patterns, and relevant lifestyle factors to support individualized planning.
🔄 2. Ongoing Review and Follow-Up
Progress is reviewed periodically to understand response and make necessary adjustments. This helps ensure care remains aligned with the patient’s evolving health status.
Homeopathic care is intended to complement appropriate medical evaluation and is not a substitute for emergency or acute medical treatment.
❤️ Patient-Centered Care
Spiritual Homeopathy Clinic follows a patient-focused approach that prioritizes safety, clarity, and informed decision-making. Individuals experiencing persistent, severe, or worsening symptoms should seek timely medical evaluation alongside any complementary care.
When to Consult
You should consult a healthcare professional if pneumonia-related symptoms are persistent, worsening, or begin to interfere with daily activities. Early medical evaluation helps assess severity, identify contributing factors, and reduce the risk of complications.
Seek consultation if you experience:
Persistent or high fever that does not settle
Ongoing cough, especially with mucus or blood
Shortness of breath or difficulty breathing
Chest pain while breathing or coughing
Extreme fatigue, weakness, or confusion (especially in older adults)
Bluish lips or fingernails
Symptoms that do not improve or worsen after a few days
Reduced appetite or difficulty feeding in children
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients who are unable to visit the clinic in person. Professional evaluation helps support an individualized care approach based on symptoms and overall health status.
For appointments or guidance, contact 9069 176 176.
FAQS
1. What is pneumonia?
Pneumonia is an infection that causes inflammation in the air sacs (alveoli) of one or both lungs. These air sacs may fill with fluid, leading to coughing, fever, chills, and difficulty breathing.
2. What causes pneumonia?
Pneumonia can be caused by:
Bacterial infections
Viral infections
Fungal infections (mainly in people with weakened immune systems)
Aspiration, when food or liquids enter the lungs
Identifying the cause helps guide an appropriate and individualized care plan.
3. What are the symptoms of pneumonia?
Common pneumonia symptoms include:
Cough (with or without mucus)
Fever and chills
Chest pain when breathing or coughing
Shortness of breath
Fatigue
Loss of appetite
In severe cases, confusion (especially in older adults), bluish lips or fingernails, or high fever may occur. Medical evaluation is advised if symptoms are persistent or worsening.
4. Is pneumonia contagious?
Some types of pneumonia are contagious, especially those caused by viruses or bacteria, and can spread through coughing, sneezing, or close contact. Other forms, such as aspiration-related pneumonia, are not contagious.
5. How is pneumonia diagnosed?
Pneumonia is commonly diagnosed through:
Physical examination of the lungs
Chest imaging
Blood investigations
Sputum analysis
Oxygen level assessment
6. How is pneumonia managed?
Management depends on the underlying cause and severity. It may include supportive care, monitoring, and condition-specific medical management. Severe cases may require hospital-based care and breathing support.
7. How long does it take to recover from pneumonia?
Recovery time varies:
Mild cases: 1–2 weeks
Moderate to severe cases: Several weeks or longer, especially in older adults or those with chronic conditions
Fatigue and mild cough can persist even after recovery.
8. Can pneumonia come back after recovery?
Yes, recurrence is possible, particularly if immunity is low or contributing factors remain unaddressed. Ongoing medical follow-up and healthy lifestyle practices may help reduce risk.
9. Is pneumonia dangerous?
Pneumonia can be serious, especially in:
Adults over 65
Infants and young children
Individuals with chronic illnesses
People with weakened immune systems
Early diagnosis and timely care reduce the risk of complications.
10. Can pneumonia be prevented?
Risk may be reduced by:
Following recommended vaccinations
Practicing good hygiene
Avoiding smoking and polluted environments
Maintaining balanced nutrition and regular activity
11. What should I eat during pneumonia recovery?
Focus on foods that support recovery, such as:
Protein-rich foods
Fruits and vegetables containing vitamins and minerals
Adequate fluids for hydration
Dietary needs may vary based on individual health status.
12. When should I see a doctor for pneumonia?
Seek medical attention if you experience:
Persistent high fever
Difficulty breathing or chest pain
Confusion or extreme fatigue
Symptoms that worsen or do not improve within a few days