Premenstrual syndrome (PMS)
Premenstrual Syndrome (PMS): Symptoms, Causes, Treatment & Relief Tips
- Home
- Premenstrual syndrome (PMS)
Premenstrual syndrome (PMS)
Effective Homeopathic Treatment for Premenstrual syndrome (PMS)
Premenstrual Syndrome (PMS): Overview, Symptoms & Impact
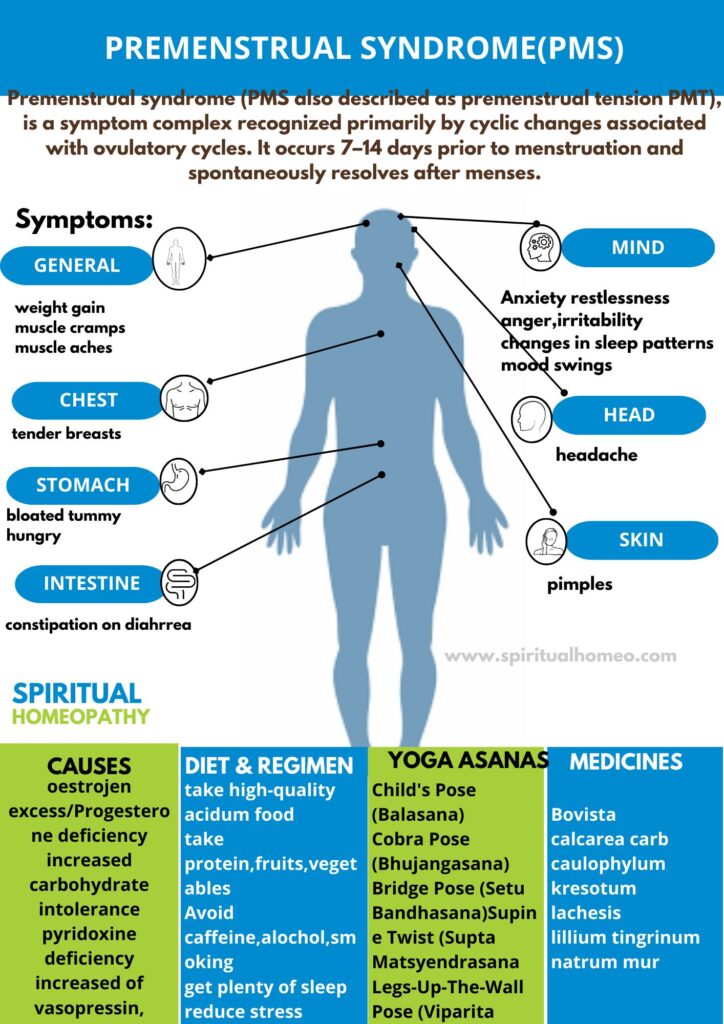
Premenstrual Syndrome (PMS) refers to a set of physical, emotional, and behavioral symptoms that occur during the luteal phase of the menstrual cycle—typically 1 to 2 weeks before menstruation begins. Common PMS symptoms include mood swings, irritability, fatigue, bloating, breast tenderness, headaches, food cravings, and sleep disturbances. The severity of PMS varies widely, ranging from mild discomfort to symptoms that significantly disrupt daily life. PMS affects millions of women and is influenced by hormonal changes, lifestyle factors, and overall health.
Everything You Need to Know
Overview
Understanding Premenstrual Syndrome (PMS): Causes, Symptoms & Relief
Most women experience mild physical and emotional changes in the days leading up to their period. These symptoms, known as menstrual molimina, usually subside with the onset of menstruation, providing relief. Premenstrual Syndrome (PMS) is more noticeable in some women, particularly between the ages of 30 and 45, with reported prevalence varying widely. The condition is commonly associated with hormonal fluctuations and increased stress during the third and fourth decades of life.
Symptoms of PMS may include mood swings, breast tenderness, food cravings, fatigue, irritability, sleep disturbances, and, in some cases, low mood or depressive feelings. The intensity and combination of symptoms can vary from person to person and from cycle to cycle.
While PMS can affect daily comfort and emotional balance, it does not have to significantly disrupt quality of life. With appropriate evaluation, supportive care, and lifestyle adjustments, symptoms can often be managed more effectively.
What Causes Premenstrual Syndrome (PMS)?
The exact cause of Premenstrual Syndrome (PMS) remains unclear. However, several biochemical and physiological factors have been proposed as potential contributors:
Hormonal Imbalances: An excess of estrogen or a relative deficiency of progesterone during the luteal phase of the menstrual cycle is believed to influence PMS symptoms.
Carbohydrate Intolerance: Some women experience increased carbohydrate intolerance during the luteal phase, which may aggravate symptoms such as fatigue, cravings, and mood changes.
Vitamin Deficiencies: A deficiency of pyridoxine (Vitamin B6) has been associated with PMS. This vitamin plays a role in estrogen metabolism and in the synthesis of neurotransmitters like serotonin and dopamine, which influence mood regulation.
Fluid Retention: Increased activity of hormones such as vasopressin, aldosterone, and prolactin, along with systemic prostaglandins, may contribute to fluid retention, bloating, and breast tenderness commonly seen in PMS.
Endorphin Fluctuations: Variations in opiate peptides affecting endorphin levels have been observed, although biochemical testing has not consistently confirmed this mechanism.
While PMS is often considered an exaggerated response to normal hormonal fluctuations of the menstrual cycle, underlying hormonal sensitivity or imbalance may also be involved. Notably, women who have undergone hysterectomy but retained their ovaries may still experience PMS symptoms, highlighting the role of ovarian hormones.
Additionally, reduced levels of beta-endorphins and serotonin are thought to contribute to emotional symptoms such as irritability, mood swings, and low mood. In some cases, genetic predisposition may also influence the likelihood of developing PMS, as it can run in families.
Types of Premenstrual Syndrome (PMS)
Premenstrual Syndrome (PMS) can manifest in different ways, and symptoms may vary in type and severity from one individual to another. Based on the predominant pattern of symptoms, PMS is generally categorized into the following types:
PMS with Depression (Affective Type)
Symptoms: Mood swings, irritability, anxiety, sadness, low mood, and emotional outbursts. Some women may feel overwhelmed, overly sensitive, or more tearful than usual.
Cause: Fluctuations in serotonin and other neurotransmitters are believed to influence mood changes and emotional distress.
PMS with Anxiety (Anxiety Type)
Symptoms: Increased feelings of stress, nervousness, or panic, along with physical signs such as restlessness or disturbed sleep.
Cause: Hormonal fluctuations may trigger heightened stress responses, particularly in women with a predisposition to anxiety.
PMS with Physical Symptoms (Somatic Type)
Symptoms: Bloating, breast tenderness, headaches, fatigue, joint pain, or muscle discomfort. Fluid retention and increased pain sensitivity may also occur.
Cause: Changes in estrogen and progesterone levels during the luteal phase contribute to these physical symptoms.
PMS with Food Cravings (Cravings Type)
Symptoms: Strong cravings for sugary, salty, or high-carbohydrate foods, often accompanied by changes in appetite or overeating.
Cause: Variations in blood sugar levels and appetite-regulating hormones such as insulin and leptin may influence cravings.
PMS with Sleep Disruption (Sleep Type)
Symptoms: Difficulty falling asleep, frequent awakenings, poor sleep quality, and excessive daytime fatigue.
Cause: Hormonal shifts, particularly changes in progesterone levels, can interfere with normal sleep patterns.
PMS with Mixed Symptoms (Combination Type)
Symptoms: A combination of physical, emotional, and behavioral symptoms, including mood changes, bloating, headaches, fatigue, and sleep issues.
Cause: A combination of hormonal and neurotransmitter fluctuations, including estrogen, progesterone, and serotonin, often leads to this pattern.
Physical and Emotional Symptoms of Premenstrual Syndrome (PMS)
PMS can cause a wide range of physical, emotional, and behavioral symptoms, which may vary in type and severity from woman to woman. These symptoms typically occur during the luteal phase of the menstrual cycle, usually one to two weeks before menstruation begins. Below is a clear overview of the commonly observed physical and emotional symptoms associated with PMS.
Physical Symptoms of PMS:
Bloating and Water Retention
Feelings of fullness or swelling in the abdomen
Swollen hands and feet due to fluid retention
Cramps
Abdominal cramps or lower back pain, often related to uterine contractions
Tender Breasts
Breast sensitivity or swelling, sometimes painful to touch
Hunger and Food Cravings
Increased appetite, especially cravings for sweets, salty foods, or carbohydrates
Headaches
Migraines or tension-type headaches linked to hormonal changes
Muscle Aches and Joint Pain
General soreness or discomfort affecting daily movement
Pimples (Acne)
Skin breakouts due to hormonal fluctuations
Weight Gain
Temporary weight gain, usually related to water retention or appetite changes
Constipation or Diarrhea
Altered bowel habits influenced by hormonal shifts
Emotional and Behavioral Symptoms of PMS:
Anxiety and Restlessness
Persistent feelings of nervousness or difficulty relaxing
Anger and Irritability
Heightened emotional sensitivity and frustration
Changes in Appetite and Cravings
Increased desire for comfort foods, often linked to emotional stress
Sleep Pattern Changes
Difficulty sleeping or excessive tiredness due to disturbed sleep
Sadness or Low Mood
Feelings of tearfulness, low mood, or emotional heaviness
Mood Swings
Sudden emotional shifts, including irritability or emotional outbursts
Decreased Sex Drive
Reduced interest in sexual activity, influenced by physical or emotional discomfort
Difficulty Concentrating
Problems with focus, memory, and mental clarity
Severe PMS and PMDD (Premenstrual Dysphoric Disorder):
While most women experience mild to moderate PMS, some may develop severe symptoms that significantly affect daily functioning, classified as Premenstrual Dysphoric Disorder (PMDD).
PMDD Symptoms include:
Severe depression, intense mood swings, or anger
Increased anxiety and feelings of being overwhelmed
Difficulty concentrating and impaired memory
Extreme irritability and emotional tension
Managing Premenstrual Syndrome (PMS): Diet and Lifestyle Tips for Relief
Premenstrual Syndrome (PMS) can affect many women, leading to physical, emotional, and behavioral symptoms that may interfere with daily activities. A balanced diet and supportive lifestyle habits can help reduce symptoms such as bloating, fatigue, irritability, and mood changes. The following guidance focuses on practical, everyday measures that may support overall well-being during the menstrual cycle.
Diet Tips for Managing PMS Symptoms
1. Focus on Complex Carbohydrates
Why: Complex carbohydrates help regulate blood sugar levels and may reduce irritability, cravings, and fatigue commonly associated with PMS.
Foods to include:
Whole grains: brown rice, quinoa, oats, barley
Root vegetables: sweet potatoes and similar vegetables
Legumes: beans, lentils, chickpeas
Tip: Choose high-fibre options to support digestion and bowel regularity.
2. Increase Magnesium Intake
Why: Magnesium supports muscle relaxation and may help with cramps, headaches, and fluid retention.
Foods to include:
Leafy greens such as spinach and kale
Nuts and seeds, including almonds and pumpkin seeds
Fruits and whole grains like bananas and oats
3. Consume Omega-3 Fatty Acids
Why: Omega-3 fatty acids have anti-inflammatory properties and may help ease menstrual discomfort.
Foods to include:
Fatty fish such as salmon and sardines
Plant sources like flaxseeds, chia seeds, and walnuts
4. Include Vitamin B6-Rich Foods
Why: Vitamin B6 plays a role in neurotransmitter function and may help with mood-related symptoms.
Foods to include:
Poultry and fish
Fruits and vegetables such as bananas, potatoes, and spinach
Fortified cereals
5. Add Vitamin E-Rich Foods
Why: Vitamin E intake may help reduce breast tenderness and general discomfort.
Foods to include:
Nuts and seeds
Green vegetables like spinach and broccoli
Avocados
6. Stay Hydrated
Why: Adequate fluid intake supports digestion and may reduce bloating and headaches.
Tip: Aim for regular water intake throughout the day. Mild herbal teas may also support hydration.
7. Limit Sugar and Refined Carbohydrates
Why: Excess sugar and refined foods can contribute to blood sugar fluctuations, worsening fatigue and irritability.
Foods to limit:
Sugary snacks and beverages
Refined grains such as white bread and pasta
8. Reduce Salt Intake
Why: High sodium intake can increase water retention and bloating.
Foods to limit:
Processed and packaged foods
Excessively salty snacks
9. Support Gut Health
Why: A healthy digestive system supports nutrient absorption and overall hormonal balance.
Foods to include:
Fermented foods with live cultures, such as yogurt
Dietary recommendations may vary based on individual health status and symptom patterns.
Lifestyle Regimen for PMS Relief
1. Stress Management
Why: Stress can intensify emotional symptoms such as anxiety and mood swings.
What to do:
Practice mindfulness or relaxation techniques
Include gentle yoga or stretching
Use slow, deep breathing exercises
2. Regular Physical Activity
Why: Moderate exercise supports hormonal balance and may reduce cramps and fatigue.
What to do:
Engage in activities like walking, swimming, or cycling most days of the week
Add light stretching to improve circulation
3. Prioritize Sleep
Why: Adequate sleep supports mood stability and energy levels.
What to do:
Maintain a consistent sleep schedule
Aim for sufficient, uninterrupted rest
Create a calming bedtime routine
4. Limit Caffeine and Alcohol
Why: Excess caffeine and alcohol may worsen sleep disturbances and emotional symptoms.
What to do:
Reduce caffeine intake, especially in the second half of the cycle
Keep alcohol consumption minimal
5. Maintain a Healthy Weight
Why: A balanced weight supports hormonal regulation and overall menstrual health.
What to do:
Follow regular meal patterns
Focus on whole, minimally processed foods
Combine balanced nutrition with regular activity
Yoga and Lifestyle Support for Premenstrual Syndrome (PMS)
Gentle yoga practices may help support physical comfort and emotional balance during Premenstrual Syndrome (PMS). The following poses focus on relaxation, improved circulation, and easing muscle tension. These practices are supportive in nature and should be performed comfortably, without strain. Yoga can be used alongside medical guidance and does not replace professional care.
1. Child’s Pose (Balasana)
Benefits:
Calms the nervous system
Relieves lower back pain and abdominal discomfort
Reduces stress and anxiety, promoting emotional balance
How to Do:
Start on your knees with your big toes together and knees apart.
Sit back onto your heels and fold forward, bringing your forehead to the mat.
Extend your arms in front or place them alongside your body.
Breathe deeply and hold for 30 seconds to 1 minute.
2. Cat–Cow Pose (Marjaryasana–Bitilasana)
Benefits:
Relieves tension in the spine, lower back, and abdomen
Improves blood circulation to the pelvic area
Reduces bloating and menstrual cramps
How to Do:
Begin in a tabletop position with wrists under shoulders and knees under hips.
Inhale as you arch your back (Cow Pose), lifting your chest and tailbone.
Exhale as you round your back (Cat Pose), drawing the chin toward the chest.
Continue slowly for 1–2 minutes.
3. Butterfly Pose (Baddha Konasana)
Benefits:
Opens the hips and releases pelvic tension
May ease menstrual cramps and lower back discomfort
Improves circulation to the pelvic region
How to Do:
Sit with legs extended, then bring the soles of your feet together.
Allow knees to fall gently to the sides.
Hold your feet and sit upright, breathing steadily.
Hold for 30 seconds to 1 minute.
4. Supine Twist (Supta Matsyendrasana)
Benefits:
Relieves tension in the lower back and hips
Supports digestion and may reduce bloating
Helps calm emotional stress
How to Do:
Lie on your back with knees bent.
Stretch arms out to the sides.
Gently drop knees to one side while keeping shoulders relaxed on the floor.
Hold for 30 seconds to 1 minute, then switch sides.
5. Legs Up the Wall Pose (Viparita Karani)
Benefits:
Reduces swelling and heaviness in the legs
Relieves pelvic and lower back discomfort
Calms the nervous system
How to Do:
Sit close to a wall and slowly raise your legs upward as you lie back.
Keep arms relaxed by your sides, palms facing up.
Hold for 5–10 minutes with slow, deep breathing.
6. Seated Forward Bend (Paschimottanasana)
Benefits:
Relieves tension in the lower back and hamstrings
Promotes mental calmness
Improves circulation to the pelvic area
How to Do:
Sit with legs extended straight.
Inhale to lengthen the spine, then exhale to fold forward gently.
Reach toward feet or shins without forcing.
Hold for 30 seconds to 1 minute.
7. Sphinx Pose (Salamba Bhujangasana)
Benefits:
Gently stretches the lower back and abdomen
May help relieve bloating
Encourages relaxation
How to Do:
Lie on your stomach with elbows under shoulders.
Press forearms into the floor and lift the chest slightly.
Keep breathing steady and relaxed.
Hold for 30 seconds to 1 minute.
8. Corpse Pose (Savasana)
Benefits:
Promotes deep relaxation
Reduces overall physical and mental tension
Supports energy restoration during the menstrual phase
How to Do:
Lie flat on your back with arms and legs relaxed.
Close your eyes and focus on slow, natural breathing.
Remain in the pose for 5–10 minutes.
Why Choose Homeopathy?
Homeopathy is a system of medicine that focuses on understanding the individual as a whole rather than addressing symptoms alone. It aims to support the body’s natural healing response by identifying underlying factors that contribute to illness. Care is tailored to each individual’s physical, emotional, and lifestyle profile and is generally well-tolerated when provided under professional guidance.
Homeopathy may be considered for both acute conditions and long-term health concerns as part of a holistic, individualized care approach.
About Spiritual Homeopathy Clinic
At Spiritual Homeopathy Clinic, care is centered on supporting overall well-being through individualized assessment and classical homeopathic principles. The clinical approach considers physical symptoms along with emotional and lifestyle influences that may affect health.
Consultations are available at multiple branches in Hyderabad, as well as through online and international consultation options, allowing continuity of care for patients who are unable to visit in person.
Approach to Care at Spiritual Homeopathy Clinic
The clinic follows a structured and patient-focused care process that emphasizes understanding contributing factors rather than symptom suppression.
In-Depth Consultation
Each consultation involves a detailed discussion of medical history, current concerns, lifestyle patterns, and emotional factors. This comprehensive evaluation supports an individualized care plan aligned with the patient’s overall health status.
Individualized Homeopathic Care
Homeopathic management focuses on long-term health support and addressing contributing imbalances. Care plans are selected based on the individual presentation rather than a one-size-fits-all approach and are reviewed periodically based on response.
Follow-Up and Ongoing Care
Regular follow-ups help monitor progress and make appropriate adjustments over time. Ongoing assessment supports continuity of care, especially in chronic or recurring conditions.
Commitment to Patient Care
Spiritual Homeopathy Clinic maintains a professional, patient-centered approach focused on safety, clarity, and individualized management. Care is guided by clinical evaluation and tailored to each patient’s needs and health goals.
When to Consult a Doctor
You should consult a healthcare professional if PMS symptoms are frequent, severe, or start to interfere with your daily activities, work, or sleep. Early assessment can help identify underlying factors and guide an individualized care plan.
Seek consultation if you experience:
Severe mood swings, irritability, or anxiety that affect relationships or work
Intense cramps, bloating, or breast tenderness that disrupt daily routines
Significant fatigue or sleep disturbances
Strong food cravings or appetite changes that impact health
Symptoms that do not improve with lifestyle or dietary adjustments
Emotional distress, depression, or sudden changes in mood
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for patients unable to visit in person. A professional assessment supports an individualized care approach tailored to your symptoms, lifestyle, and overall health.
For appointments or guidance, contact 9069 176 176.
FAQs
1. What is Premenstrual Syndrome (PMS)?
PMS is a set of physical, emotional, and behavioral symptoms occurring in the luteal phase of the menstrual cycle, typically 1–2 weeks before menstruation. Symptoms can include mood swings, irritability, fatigue, bloating, breast tenderness, and headaches.
2. What causes PMS?
The exact cause is not fully understood, but PMS is primarily linked to hormonal fluctuations during the menstrual cycle, especially changes in estrogen and progesterone. Other factors, such as genetics, stress, and lifestyle, may also contribute. Individual factors can influence symptom severity.
3. How long does PMS last?
Symptoms usually begin 1–2 weeks before menstruation and subside within a few days after the period starts. Duration and intensity can vary among individuals.
4. What are the common symptoms of PMS?
Physical: Bloating, cramps, tender breasts, headaches, muscle or joint pain, fatigue, and appetite changes.
Emotional: Mood swings, irritability, anxiety, sadness, and difficulty concentrating.
Behavioral: Sleep disturbances, food cravings (especially sweets), and reduced sexual desire.
5. Can PMS be prevented?
PMS cannot be completely prevented. However, lifestyle measures—such as regular exercise, balanced nutrition, stress management, and proper sleep—can help reduce symptom severity. Professional guidance may also be useful for persistent or severe symptoms.
6. How can I manage PMS symptoms?
Effective strategies include:
Dietary adjustments: Focus on complex carbohydrates, magnesium, and Omega-3s; limit sugar, salt, and caffeine.
Exercise: Regular physical activity can relieve cramps, improve mood, and reduce stress.
Stress management: Techniques like yoga, meditation, deep breathing, and mindfulness can support emotional balance.
Sleep: Aim for 7–9 hours of quality sleep each night.
Professional care: In some cases, medical or homeopathic guidance may help manage severe symptoms.
7. How do I know if I have PMS or a more serious condition?
PMS is generally cyclical, with symptoms improving after menstruation begins. Severe, prolonged, or disabling symptoms may indicate Premenstrual Dysphoric Disorder (PMDD) or another underlying condition. A healthcare provider can evaluate and guide appropriate management.
8. Can stress worsen PMS symptoms?
Yes, stress can increase symptom severity by affecting hormone levels. Stress reduction practices, such as yoga, meditation, and relaxation techniques, may help alleviate symptoms.
9. Is PMS common?
Yes, most women experience PMS at some point. About 80–90% of women report mild to moderate symptoms, while 5–10% may experience severe symptoms that interfere with daily life (PMDD).
10. Are there any home remedies for PMS relief?
Some supportive measures include:
Warm compresses or heating pads for cramps.
Herbal teas such as chamomile or ginger to ease bloating.
Nutritional support, such as magnesium, vitamin B6, or calcium, under professional guidance.
11. Can PMS affect fertility?
PMS itself does not usually affect fertility. However, underlying conditions such as endometriosis or PCOS, which may cause PMS-like symptoms, can impact fertility. Evaluation by a healthcare provider is recommended if concerned.
12. When should I consult a doctor about PMS?
Seek consultation if PMS symptoms are severe, persistent, or significantly affect daily activities. Early professional assessment helps tailor an individualized care plan. At Spiritual Homeopathy Clinic, consultations are available at multiple Hyderabad branches, as well as online and international options. Contact 9069 176 176 for guidance.
13. Can PMS symptoms change with age?
Yes, symptoms may change as women approach perimenopause. Some experience milder PMS, while others may notice more intense symptoms due to hormonal fluctuations.
14. Is there a link between PMS and other health conditions?
PMS can be associated with conditions such as mood disorders, fibromyalgia, irritable bowel syndrome (IBS), or chronic fatigue syndrome, which may increase symptom severity.
15. How does yoga help with PMS?
Yoga supports relief from cramps, bloating, and lower back discomfort through improved circulation, flexibility, and muscle relaxation. Deep breathing and meditation help manage stress and mood swings, complementing overall symptom management.