Idiopathic Thrombocytopenic Purpura
Idiopathic Thrombocytopenic Purpura (ITP): Causes, Symptoms, Diagnosis & Treatment Options
- Home
- Idiopathic Thrombocytopenic Purpura
Idiopathic Thrombocytopenic Purpura
Effective Homeopathic Treatment for Idiopathic Thrombocytopenic purpura
Idiopathic Thrombocytopenic Purpura (ITP)—also known as Immune Thrombocytopenic Purpura—is a blood disorder characterized by a low platelet count without an identifiable cause and with otherwise normal bone marrow function. This autoimmune condition occurs when the body’s immune system mistakenly attacks and destroys its own platelets. ITP often leads to symptoms like easy bruising, a red or purple skin rash (called purpura), and an increased risk of bleeding.
Everything You Need to Know
Overview
Idiopathic Thrombocytopenic Purpura (ITP) presents in two main forms: acute and chronic. The acute form typically affects children and often follows a viral infection, with symptoms usually resolving within a few weeks to two months. Chronic ITP lasts longer than six months and may occur without a clearly identifiable cause.
ITP is an autoimmune condition, in which the immune system mistakenly targets and destroys platelets, leading to a reduced platelet count and increased bleeding tendency.
Diagnosis primarily involves detecting a low platelet count through a complete blood count (CBC). Because ITP is a diagnosis of exclusion, additional tests—such as a bone marrow examination—may sometimes be necessary to rule out other causes of low platelets.
Consultation Note: Expert evaluation is available at Spiritual Homeopathy Clinic, with in-clinic appointments across multiple Hyderabad branches and online or international consultations for patients who cannot visit in person. Early assessment allows for an individualized care plan tailored to platelet levels, symptoms, and overall health.
Causes of Idiopathic Thrombocytopenic Purpura (ITP)
1. Decreased Platelet Production
Reduced platelet production may occur due to impaired function of megakaryocytes, the cells responsible for producing platelets in the bone marrow. This can result from bone marrow suppression, exposure to certain substances, or underlying systemic conditions, leading to thrombocytopenia.
2. Increased Platelet Destruction
This is the most common mechanism in ITP, where the immune system mistakenly identifies platelets as foreign and destroys them. When no clear cause is identified, the condition is referred to as idiopathic immune thrombocytopenia. In secondary ITP, platelet destruction may be associated with underlying conditions or triggers, including:
Immune-Related Conditions:
Collagen vascular diseases
Autoimmune disorders such as systemic lupus erythematosus
Lymphoproliferative disorders
Drug-Related Triggers:
Certain medications may interfere with platelet survival or immune regulation, contributing to reduced platelet counts.
Non-Immune Mechanisms:
Platelet destruction may also occur due to non-immune causes, such as:
Disseminated intravascular coagulation (DIC)
Thrombotic microangiopathies
Bone marrow suppression or failure
Hematological malignancies
3. Abnormal Platelet Pooling
In some cases, platelets may become sequestered in the spleen or other organs, reducing the number available in circulation. This may be seen in conditions such as:
Splenomegaly
Congestive splenic enlargement
Certain neoplastic disorders
4. Other Contributing Factors
Additional conditions that may be associated with low platelet counts include:
Chronic viral infections
Liver-related disorders
Pregnancy-related changes
Systemic illnesses affecting immune regulation
Clinical Note:
Since ITP can result from multiple overlapping factors, identifying the underlying mechanism is essential. A detailed clinical evaluation helps support an individualized care approach based on platelet trends, associated conditions, and overall health status.
Types of Idiopathic Thrombocytopenic Purpura (ITP)
1. Acute Idiopathic Thrombocytopenic Purpura (Acute ITP)
Acute ITP primarily affects children and often follows an infection, such as a viral illness. The condition usually develops suddenly, with a rapid decline in platelet count. In many cases, symptoms improve within a few weeks to months. Acute ITP is generally transient in nature, and most children recover without long-term complications.
2. Chronic Idiopathic Thrombocytopenic Purpura (Chronic ITP)
Chronic ITP is diagnosed when low platelet levels persist for more than six months. This form is more commonly seen in adults and may continue for an extended period. In several cases, no specific cause is identified, though immune system dysregulation is frequently involved. Individuals with chronic ITP may need ongoing monitoring and long-term management to reduce the risk of bleeding and maintain platelet stability.
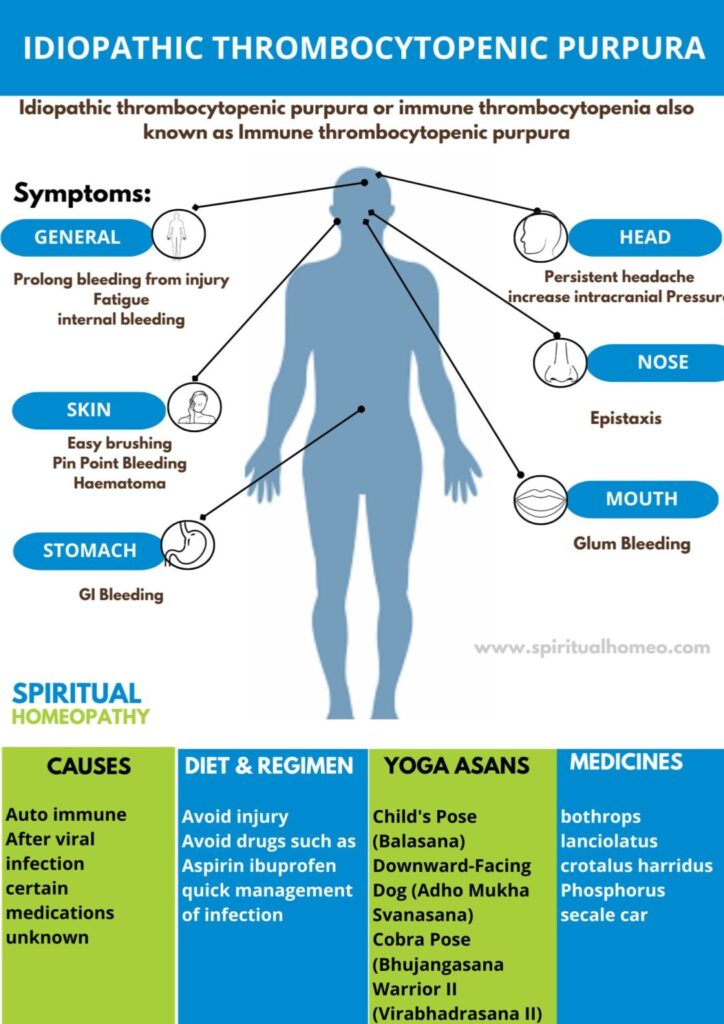
Signs and Symptoms of Idiopathic Thrombocytopenic Purpura (ITP)
Acute Thrombocytopenia (Acute ITP)
In cases of acute thrombocytopenia, symptoms can be more pronounced, particularly when the condition develops suddenly. These may include:
Widespread purpura and easy bruising
Mucosal bleeding, such as nosebleeds (epistaxis) or bleeding gums
Cerebral and gastrointestinal (GI) hemorrhage, which may present as fundal hemorrhage, persistent headaches, or other signs of raised intracranial pressure
Children with acute thrombocytopenia generally experience milder symptoms and tend to have a better prognosis, especially when the condition follows viral infections such as measles or Epstein–Barr virus (EBV). These cases are often self-limiting and may resolve without aggressive intervention, with many children recovering over time under medical supervision.
Chronic Idiopathic Thrombocytopenic Purpura (Chronic ITP)
Chronic ITP is more frequently observed in young adults, particularly women. Symptoms may vary over time, with periods of remission and flare-ups. Common features of chronic ITP include:
Purpura (purple discoloration or bruising under the skin)
Epistaxis (recurrent nosebleeds)
Menorrhagia (heavy or prolonged menstrual bleeding) in women
Chronic ITP may follow a viral illness, although the underlying cause is not always identifiable. As in acute ITP, symptom severity largely depends on the degree of platelet reduction.
Platelet Count and Severity of Bleeding in ITP
The risk and severity of bleeding in both acute and chronic ITP are closely related to platelet levels:
Platelet count > 50,000/µL: Spontaneous bleeding is uncommon
Platelet count 10,000–50,000/µL: Bleeding may involve the skin and mucous membranes
Platelet count < 10,000/µL: There is a higher risk of post-traumatic bleeding and serious gastrointestinal or genitourinary hemorrhage, which may require urgent medical attention
Clinical Note:
If symptoms are frequent, worsening, or associated with significant bleeding, timely consultation with a healthcare professional is advised for proper evaluation and monitoring.
Diet and Regimen for Idiopathic Thrombocytopenic Purpura (ITP)
A balanced diet and healthy lifestyle play an important supportive role in managing Idiopathic Thrombocytopenic Purpura (ITP) and overall platelet health. The following dietary and regimen guidelines may help individuals maintain general well-being while living with ITP.
Diet for ITP:
Iron-Rich Foods:
Include spinach, lentils, lean meats, and beets to help support blood health and address anemia when present.
Folate & Vitamin B12:
Leafy green vegetables, eggs, dairy products, and legumes contribute to healthy cell and platelet formation.
Vitamin C:
Citrus fruits, bell peppers, and guava may aid iron absorption and support immune function.
Omega-3 Fatty Acids:
Walnuts, chia seeds, and flaxseeds have anti-inflammatory properties that support overall health.
Avoid:
Limit alcohol intake, refined sugars, highly processed foods, and artificial additives, as these may affect immune balance and platelet function.
Regimen for ITP:
Gentle Exercise:
Low-impact activities such as walking or yoga can improve circulation without increasing the risk of injury or bruising.
Adequate Rest:
Proper sleep supports immune regulation and overall recovery.
Stress Management:
Relaxation practices such as meditation or deep breathing may help reduce stress-related symptom fluctuations.
Hydration:
Maintaining adequate fluid intake supports general health and bodily functions.
Individual dietary and lifestyle recommendations may vary based on age, platelet levels, and associated medical conditions.
Note:
Always consult a qualified healthcare professional before making significant dietary or lifestyle changes, particularly if symptoms worsen or other medical conditions are present. Patients may seek guidance through in-clinic, online, or international consultations available at Spiritual Homeopathy Clinic.
Yoga Asanas for Managing Idiopathic Thrombocytopenic Purpura (ITP)
Yoga can play a supportive role in managing stress, improving circulation, and promoting overall well-being in individuals with Idiopathic Thrombocytopenic Purpura (ITP). Gentle yoga practices may help maintain physical and emotional balance without placing excessive strain on the body, which is especially important for people with low platelet counts.
1. Tadasana (Mountain Pose)
Benefits: Improves posture, supports blood circulation, and helps calm the mind.
How to Do It: Stand with feet hip-width apart, engage the legs, and lengthen the spine. Raise the arms upward with palms facing each other and breathe slowly and steadily.
2. Viparita Karani (Legs-Up-The-Wall Pose)
Benefits: Helps reduce fatigue, promotes relaxation, and supports stress relief.
How to Do It: Sit beside a wall, lie back gently, and extend the legs upward against the wall. Rest the arms comfortably and maintain relaxed breathing for 5–10 minutes.
3. Sukhasana (Easy Pose)
Benefits: Encourages mindfulness, reduces stress, and supports mental clarity.
How to Do It: Sit cross-legged with the spine upright. Place the hands on the knees with palms facing upward, close the eyes, and focus on slow, even breathing.
4. Bhujangasana (Cobra Pose)
Benefits: Strengthens the spine, opens the chest, and supports circulation.
How to Do It: Lie on the abdomen with hands under the shoulders. Gently lift the chest using the arms while keeping the hips and legs grounded. Avoid overstretching.
5. Setu Bandhasana (Bridge Pose)
Benefits: Supports circulation, strengthens the back and legs, and opens the chest area.
How to Do It: Lie on the back with knees bent and feet flat on the floor. Slowly lift the hips upward while keeping the shoulders and feet grounded. Hold briefly and lower gently.
6. Ananda Balasana (Happy Baby Pose)
Benefits: Releases lower back tension and promotes deep relaxation.
How to Do It: Lie on the back, draw the knees toward the chest, and hold the outer edges of the feet. Gently relax into the pose while maintaining steady breathing.
7. Pranayama (Breathing Exercises)
Benefits: Helps calm the nervous system, reduces stress, and supports emotional regulation.
How to Do It: Sit comfortably with eyes closed and focus on the breath. Practice slow, deep breathing—inhale through the nose, pause briefly, and exhale slowly. Continue for several minutes.
Important Note:
Yoga and breathing practices are supportive measures and should not replace medical care. Individuals with very low platelet counts or active bleeding should consult a healthcare professional before starting any physical activity. Guidance may be taken through in-clinic, online, or international consultations at Spiritual Homeopathy Clinic.
🌿 Why Choose Homeopathy?
Homeopathy is a system of healthcare that focuses on understanding the individual as a whole, rather than addressing symptoms alone. It aims to support the body’s natural regulatory mechanisms and considers physical, emotional, and lifestyle factors in care planning.
Homeopathic care is commonly used in both acute and chronic conditions as part of a holistic, individualized approach to health management.
🌟 Spiritual Homeopathy Clinic: Care Through Individualized Approach
At Spiritual Homeopathy Clinic, care is centered on understanding each patient’s health concerns in a comprehensive manner. The focus is on individualized assessment, with attention to physical symptoms, emotional well-being, and overall health patterns.
Rather than addressing symptoms in isolation, the approach emphasizes identifying contributing factors that may influence health over time.
Consultations are available across multiple branches in Hyderabad, as well as through online and international consultation services.
💫 Approach at Spiritual Homeopathy Clinic
The clinical approach integrates classical homeopathic principles with detailed case evaluation. Key aspects include:
Individualized Care: Each patient is assessed based on personal health history, symptoms, and lifestyle factors.
Long-Term Management Perspective: Care plans are designed to support ongoing health monitoring and balance.
Professional Guidance: Consultations are conducted by qualified practitioners with clinical experience.
Mind–Body Consideration: Emotional and mental health factors are considered alongside physical symptoms.
🔍 Our Treatment Process
🩺 1. In-Depth Consultation
Each consultation involves a detailed discussion of medical history, current concerns, lifestyle patterns, and emotional factors. This helps in forming a clear understanding of the individual’s health status.
🔄 2. Individualized Care Planning
Based on assessment findings, a personalized care plan is developed, focusing on contributing factors and overall health regulation rather than isolated symptoms.
🔁 3. Follow-Up and Monitoring
Regular follow-ups allow for monitoring symptom patterns and overall response, supporting adjustments when clinically appropriate.
🧾 Patient-Centered Care Commitment
Spiritual Homeopathy Clinic emphasizes ethical practice, clinical responsibility, and patient education. Homeopathic care is offered as a complementary, individualized approach and does not replace emergency or specialist medical care when required.
For guidance or consultation, patients are encouraged to seek timely professional advice.
When to Consult
You should consult a healthcare professional if symptoms of Idiopathic Thrombocytopenic Purpura (ITP) become frequent, persistent, or begin to interfere with daily activities. Early evaluation helps assess platelet levels, identify contributing factors, and reduce the risk of bleeding-related complications.
Seek consultation if you experience:
Recurrent or unexplained bruising or purpura
Frequent nosebleeds or bleeding from the gums
Prolonged bleeding from minor cuts or injuries
Heavy or prolonged menstrual bleeding
Blood in urine or stools
Persistent fatigue or symptoms that worsen over time
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. Online and international consultations are also available for individuals unable to visit in person. A professional assessment supports an individualized care approach based on platelet status, symptoms, and overall health.
For appointments or guidance, contact 9069 176 176.
FAQ
1. What is Idiopathic Thrombocytopenic Purpura (ITP)?
Idiopathic Thrombocytopenic Purpura (also known as Immune Thrombocytopenic Purpura) is a condition in which the immune system mistakenly targets and destroys platelets, which are essential for normal blood clotting. This leads to a reduced platelet count and may result in easy bruising, bleeding, or purpura (red or purple skin spots).
2. What are the main symptoms of ITP?
Common symptoms may include:
Easy or unexplained bruising
Petechiae (small red or purple spots under the skin)
Frequent nosebleeds or bleeding gums
Fatigue or weakness
Heavy or prolonged menstrual bleeding in women
If symptoms are persistent or worsening, medical consultation is advised.
3. What causes ITP?
The exact cause of ITP is not fully understood. It is considered an autoimmune condition in which the body produces antibodies against platelets. It may sometimes be associated with infections, immune system imbalance, or other underlying health conditions.
4. Is ITP a genetic condition?
ITP is generally not considered a hereditary disorder. While rare familial patterns have been observed, most cases occur sporadically without a clear genetic link.
5. How is ITP diagnosed?
ITP is usually identified through blood investigations, especially a complete blood count showing low platelet levels. Additional tests may be done to exclude other causes of thrombocytopenia, based on clinical judgment.
6. What is the difference between acute and chronic ITP?
Acute ITP: More commonly seen in children, often following an infection, and usually resolves within a few months.
Chronic ITP: More common in adults and persists for longer than six months, often requiring long-term monitoring.
7. What treatment approaches are used for ITP?
Management depends on platelet levels, symptoms, and overall health. Conventional care focuses on reducing immune-related platelet destruction and monitoring bleeding risk. Complementary approaches such as homeopathy aim at individualized care and long-term management under professional guidance.
8. Can physical activity be done with ITP?
Gentle activities such as walking or yoga are generally encouraged. High-impact or contact activities that increase bleeding risk should be avoided. Exercise plans should be discussed with a healthcare professional.
9. Can diet help in managing ITP?
A balanced diet supports overall health and immune function. Nutrient-rich foods that support blood health may be beneficial. Dietary guidance may vary based on individual health status and should be personalized.
10. What are the possible complications of ITP?
If platelet levels drop significantly, there is an increased risk of bleeding, including internal bleeding. Regular monitoring and timely medical care help reduce these risks.
11. Is ITP a life-threatening condition?
Most individuals with ITP live stable, active lives with proper monitoring. Serious complications are uncommon but can occur if bleeding is severe, highlighting the importance of regular follow-up.
12. Can ITP go into remission?
Yes, remission can occur, particularly in children. In adults, ITP may enter periods of remission or remain manageable with appropriate long-term care and monitoring.
13. Are lifestyle changes important in ITP?
Yes. General recommendations include:
Avoiding substances that may increase bleeding risk
Attending regular follow-ups to monitor platelet levels
Managing stress through relaxation techniques, which may support immune balance