Diabetes
Reversing the Sugar Trap: Natural Ways to Control Diabetes Effectively
- Home
- Diabetes
Diabetes
Homeopathy treatment for Diabetes
Diabetes mellitus is a chronic metabolic disorder that occurs when the body is unable to produce enough insulin or use it effectively, leading to elevated blood sugar levels (hyperglycemia). It can result from issues with insulin secretion, insulin action, or both, and requires long-term management to prevent complications.
Everything You Need to Know
Overview: Understanding Diabetes Mellitus
Diabetes mellitus is a chronic metabolic disorder in which the level of sugar (glucose) in the blood becomes abnormally high. This condition develops due to problems in insulin production, insulin action, or both. The term diabetes mellitus is used to distinguish it from diabetes insipidus, a rare condition that also causes increased urination but does not affect blood glucose levels.
Diabetes requires long-term monitoring and individualized management. Consultations are available at Spiritual Homeopathy Clinic, with multiple branches in Hyderabad, as well as online and international consultation options.
What Is Blood Sugar?
The food we consume mainly consists of three nutrients: carbohydrates, proteins, and fats. Carbohydrates are broken down into various forms of sugars—simple sugars such as glucose and fructose, and complex carbohydrates like starches found in rice, bread, and pasta.
During digestion, complex carbohydrates are converted into simple sugars. Once absorbed, most sugars are transformed into glucose, which serves as the body’s primary source of energy. Glucose circulates through the bloodstream and enters cells, where it is either used immediately or stored for future energy needs.
The Role of Insulin
Insulin is an essential hormone produced by the pancreas, located behind the stomach. After meals, rising blood glucose levels stimulate the release of insulin. This hormone enables glucose to move from the bloodstream into body cells.
Within the cells, glucose is used for energy or stored as glycogen or fat. In healthy individuals, blood glucose levels fluctuate modestly—typically increasing after meals and returning to normal within two hours. Normal fasting blood glucose levels usually range between 70 and 110 mg/dL (3.9 to 6.1 mmol/L), with slightly higher post-meal values seen in older adults.
What Happens in Diabetes?
In diabetes, this regulatory process is impaired. The body may produce insufficient insulin or the cells may not respond effectively to insulin, a condition known as insulin resistance. As a result:
Glucose accumulates in the bloodstream, causing elevated blood sugar levels (hyperglycemia)
Cells are unable to access adequate glucose, leading to fatigue and other symptoms
If not appropriately managed, this imbalance can contribute to persistent symptoms and long-term health complications. Early evaluation supports structured, individualized care and ongoing monitoring.
Causes of Type 2 Diabetes: What You Should Know
Type 2 diabetes develops due to a combination of genetic, lifestyle, and metabolic factors. Understanding these contributing causes is important for early identification and structured long-term management.
Insulin Resistance
One of the primary causes of type 2 diabetes is insulin resistance, a condition in which the body’s cells do not respond effectively to insulin. As a result, insulin is unable to move glucose efficiently from the bloodstream into the cells, leading to elevated blood sugar levels.
Central Obesity (Abdominal Obesity)
Excess fat around the abdomen, also referred to as central or abdominal obesity, is strongly associated with insulin resistance. Abdominal fat is metabolically active and releases substances known as adipokines, which can interfere with normal blood glucose regulation.
Genetic Factors and Family History
A family history of diabetes significantly increases the likelihood of developing type 2 diabetes. Individuals with one or more close relatives affected by diabetes may inherit a tendency toward insulin resistance or impaired glucose metabolism.
Childhood Obesity and Early Onset
The increasing prevalence of childhood obesity has contributed to a rise in type 2 diabetes among children and adolescents. Factors such as unhealthy dietary habits, reduced physical activity, and prolonged screen time play a major role in early-onset diabetes.
Studies indicate that more than 55% of individuals diagnosed with type 2 diabetes are overweight or obese, highlighting the importance of weight management in overall diabetes care.
Understanding these causes helps guide an individualized care approach that considers personal risk factors, lifestyle patterns, and metabolic health. Consultations are available at Spiritual Homeopathy Clinic, with in-clinic services across Hyderabad and options for online and international consultations.
Types and Classification of Diabetes Mellitus
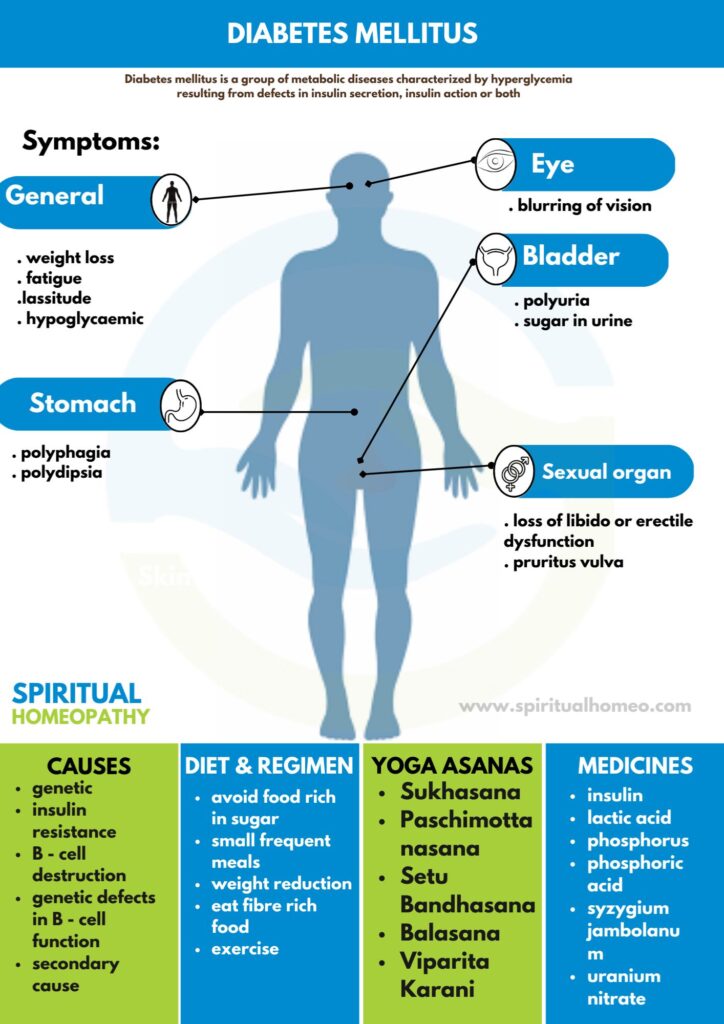
Diabetes mellitus is a group of metabolic disorders characterized by persistently elevated blood glucose levels (hyperglycemia) resulting from defects in insulin secretion, insulin action, or both. Understanding the different types of diabetes supports accurate diagnosis and appropriate long-term management.
1. Type 1 Diabetes Mellitus (T1DM)
Also known as Insulin-Dependent Diabetes Mellitus (IDDM), Type 1 diabetes occurs due to destruction of insulin-producing beta cells in the pancreas, leading to absolute insulin deficiency. It commonly develops during childhood or adolescence.
Autoimmune: The immune system mistakenly attacks pancreatic beta cells
Idiopathic: Cause is unknown and not linked to autoimmunity
2. Type 2 Diabetes Mellitus (T2DM)
Previously called Non-Insulin Dependent Diabetes Mellitus (NIDDM), this is the most common form of diabetes. It develops due to insulin resistance along with relative insulin deficiency. Although more common in adults, it is increasingly seen in younger individuals due to obesity and sedentary lifestyles.
3. Maturity-Onset Diabetes of the Young (MODY)
MODY is a rare, inherited form of diabetes caused by specific genetic mutations affecting pancreatic beta-cell function. It usually develops before the age of 25.
MODY 1: Mutation in HNF4α
MODY 2: Mutation in Glucokinase
MODY 3: Mutation in HNF1α
MODY 4–6: Mutations involving IPF1, NeuroD1, and related genes
4. Secondary Diabetes Mellitus
This form develops as a consequence of other medical conditions or external factors.
a. Pancreatic Diseases
Pancreatitis
Cystic fibrosis
Hemochromatosis
Pancreatic trauma or cancer
Fibrocalcific pancreatic diabetes (FCPD)
b. Endocrine Disorders
Cushing’s syndrome
Acromegaly
Hyperthyroidism
Pheochromocytoma
Glucagonoma
c. Drug-Induced Diabetes
Certain medications may interfere with glucose regulation, including:
Glucocorticoids
Thiazide diuretics
Phenytoin
Interferons
Beta-blockers
Thyroid hormones
d. Infections
Congenital rubella
Coxsackie B virus
Cytomegalovirus
e. Insulin Receptor Defects
Anti-insulin receptor antibodies
Lipoatrophic diabetes
f. Genetic Syndromes Associated with Diabetes
Down syndrome
Turner syndrome
Klinefelter syndrome
Prader-Willi syndrome
Wolfram syndrome
Friedreich’s ataxia
Laurence-Moon-Biedl syndrome
Myotonic dystrophy
Porphyria
5. Gestational Diabetes Mellitus (GDM)
Gestational diabetes develops during pregnancy due to hormonal changes that reduce insulin sensitivity. It increases the future risk of type 2 diabetes for both the mother and the child.
6. Impaired Glucose Tolerance (IGT) / Borderline Diabetes
IGT refers to blood glucose levels that are higher than normal but not high enough for a diabetes diagnosis. It may be:
Primary: Often associated with obesity or physical inactivity
Secondary: Related to liver disease, kidney disorders, chronic malnutrition, stress, or certain medications
Early identification and individualized care—including lifestyle guidance and supportive approaches such as homeopathy—may help manage glucose intolerance and reduce the risk of progression or complications.
Signs and Symptoms of Diabetes
The symptoms of diabetes may vary depending on age, duration, and type of diabetes. In adults, the onset is often gradual and may remain unnoticed for months or even years. In children, symptoms can appear suddenly and may progress more rapidly.
Common Warning Signs and Symptoms Include:
Increased urination (polyuria): Frequent urination, especially during the night.
Excessive thirst (polydipsia): Persistent thirst due to fluid loss caused by elevated blood glucose levels.
Increased hunger (polyphagia): Feeling hungry frequently, even after eating.
Unexplained weight loss: Weight loss despite normal or increased food intake, as the body is unable to use glucose effectively.
Fatigue and weakness: Reduced energy levels due to inadequate glucose entry into body cells.
Blurred vision: Elevated blood sugar may affect the eye lens, leading to temporary visual disturbances.
Frequent infections or delayed wound healing: Including skin infections, urinary tract infections, or recurrent yeast infections, particularly in women.
Itching or irritation: Such as pruritus vulvae in women or balanitis in men, often related to glucose in the urine.
Reduced libido or erectile dysfunction: Common in long-standing or poorly controlled diabetes due to nerve or vascular involvement.
Serious or Emergency Symptoms:
Abdominal pain: May indicate diabetic ketoacidosis (DKA), particularly in individuals with type 1 diabetes.
Convulsions or seizures: In children, sudden seizures should raise concern for hypoglycemia (low blood sugar).
Daytime seizures may suggest epilepsy
Night-time seizures are more commonly associated with hypoglycemic episodes in insulin-treated individuals
Note: Recurrent hypoglycemia in insulin users may lead to EEG changes, highlighting the importance of regular monitoring and professional supervision.
Diabetes Diet and Regimen: Key Principles for Blood Sugar Control
Managing diabetes through proper diet and lifestyle plays an important role in maintaining stable blood glucose levels and reducing the risk of complications. The following dietary and regimen principles support overall metabolic balance in individuals with diabetes.
1. Achieve Normal Blood Glucose and Lipid Levels
Maintaining blood glucose levels as close to normal ranges as possible helps reduce the risk of long-term complications such as cardiovascular disease and neuropathy.
Regular monitoring of glucose and lipid levels supports effective disease management and timely adjustments in care.
2. Prevent the Onset or Progression of Diabetes Complications
Keeping blood sugar levels under control may help slow the progression of complications, including kidney disease, vision disturbances, and nerve-related issues.
A balanced diet combined with healthy lifestyle practices supports long-term metabolic stability.
3. Support Growth and Development in Children and Adolescents
Maintaining appropriate blood glucose levels in children and adolescents with diabetes supports normal physical and cognitive development.
A nutritionally balanced diet is essential during growth years to meet developmental needs.
4. Maintain Reasonable Body Weight in Adults and Adolescents
Achieving and maintaining a healthy body weight may improve insulin sensitivity and assist in better blood sugar regulation.
Balanced nutrition with appropriate caloric intake supports sustainable weight management.
5. Nutritional Support for Pregnant Women
For pregnant women with diabetes, adequate nutrition is essential to support both maternal health and fetal development.
Structured meal planning helps maintain stable blood glucose levels during pregnancy and lactation.
6. Consistency in Meal Timing
Regular meal timing helps minimize sudden blood sugar fluctuations.
Eating at consistent intervals supports steady energy levels and metabolic balance throughout the day.
7. Small, Frequent Meals for Better Blood Sugar Control
Consuming smaller, frequent meals may help stabilize blood glucose levels and prevent excessive hunger.
This approach can assist in maintaining consistent energy levels and better dietary control.
8. Personalized Meal Plans for Better Compliance
Meal plans tailored to an individual’s lifestyle, dietary preferences, and health status support better long-term adherence.
Dietary guidance may vary from person to person and should be adjusted under professional supervision.
9. Weight Management for Obese Individuals with Type 2 Diabetes
In individuals with type 2 diabetes and obesity, gradual weight reduction may improve insulin responsiveness.
Balanced nutrition combined with appropriate physical activity supports effective weight management.
10. Focus on Balanced Carbohydrates
Choosing complex carbohydrates rich in fiber, such as whole grains, vegetables, and legumes, supports better blood sugar regulation.
Limiting refined carbohydrates and added sugars may help reduce sudden glucose spikes.
Conclusion
A balanced diet, consistent meal timing, and healthy weight management are central to diabetes care. Dietary recommendations should be individualized based on age, health status, and lifestyle. For personalized guidance, consultation is available at Spiritual Homeopathy Clinic, with services offered through multiple branches in Hyderabad, as well as online and international consultations.
🧘♂️ Yoga Asanas for Diabetes Management
Yoga can serve as a supportive lifestyle practice for individuals managing diabetes. Regular practice may help improve metabolic balance, digestion, and stress regulation. Yoga should be performed as a complementary approach and not as a replacement for medical care.
1. Bhujangasana (Cobra Pose)
Benefits: Stimulates abdominal organs, supports digestive function, and may assist in metabolic regulation.
How to Practice: Lie on your stomach, place hands under your shoulders, and gently lift the chest while keeping elbows close to the body.
2. Dhanurasana (Bow Pose)
Benefits: Helps activate abdominal organs and supports digestive and metabolic processes.
How to Practice: Lie on your stomach, bend the knees, hold the ankles, and gently lift the chest and legs together.
3. Paschimottanasana (Seated Forward Bend)
Benefits: Supports digestion, helps reduce abdominal tension, and promotes relaxation of the nervous system.
How to Practice: Sit with legs extended, inhale and raise the arms, then exhale and bend forward toward the feet.
4. Ardha Matsyendrasana (Seated Spinal Twist)
Benefits: Encourages gentle stimulation of abdominal organs and supports digestive health.
How to Practice: Sit with one leg bent and the other crossed over, twist the torso toward the raised knee, and hold comfortably.
5. Vajrasana (Thunderbolt Pose)
Benefits: Aids digestion and may help manage post-meal discomfort when practiced after eating.
How to Practice: Kneel on the floor and sit back on the heels, keeping the spine straight and hands resting on the thighs.
6. Sarvangasana (Shoulder Stand) (Advanced)
Benefits: Supports circulation and endocrine balance when performed correctly.
Note: This posture should be practiced only under professional guidance and avoided by individuals with neck issues, uncontrolled blood pressure, or other medical concerns.
7. Shavasana (Corpse Pose)
Benefits: Promotes relaxation, reduces stress levels, and supports overall hormonal balance.
How to Practice: Lie flat on your back, relax the body fully, and focus on slow, deep breathing.
Yoga practices should be adapted to individual health status and performed under appropriate guidance. Consultation is advised if symptoms are persistent or if there are existing medical conditions.
Why Choose Spiritual Homeopathy?
At Spiritual Homeopathy Clinic, care is provided using established homeopathic principles along with an understanding of physical and emotional health factors. Our team of qualified homeopathic doctors in Hyderabad focuses on structured, patient-centered care that aims to support overall health alongside symptom management.
Our Approach to Care
We follow a holistic care framework that considers physical symptoms, emotional well-being, and individual health patterns. The approach focuses on understanding contributing factors rather than addressing symptoms alone. Care is planned to support the body’s natural regulatory processes and promote balance over time, based on individual health needs.
Our Services
Personalized Consultations
Patients receive detailed consultations that include discussion of medical history, current symptoms, and lifestyle factors. Consultations are available at multiple branches in Hyderabad, as well as through online and international consultation, allowing continuity of care for individuals with diabetes who may not visit in person.
Homeopathic Care Approach
Homeopathic care is planned on an individualized basis, considering disease duration, associated conditions, and overall health status. The approach is commonly used as part of long-term management and is generally well-tolerated when followed under professional guidance.
Ongoing Follow-Up Care
Regular follow-up is an important part of care, especially for chronic conditions such as diabetes. Follow-up consultations help monitor symptom patterns, lifestyle adherence, and overall response, allowing care plans to be adjusted when needed.
Our Commitment to Health and Wellness
Spiritual Homeopathy Clinic remains focused on providing structured, responsible care through personalized consultations and ongoing guidance. Individuals seeking support for diabetes management or overall health maintenance can consult the clinic for professional evaluation and care planning.
When to Consult
You should consult a healthcare professional if diabetes-related symptoms become frequent, persistent, or begin to interfere with daily activities. Early evaluation helps in timely diagnosis, monitoring, and reducing the risk of long-term complications.
Seek consultation if you experience:
Frequent urination or excessive thirst
Unexplained weight loss or persistent fatigue
Increased hunger despite regular meals
Blurred vision or frequent headaches
Slow-healing wounds or recurrent infections
Tingling, numbness, or burning sensation in hands or feet
Symptoms that do not improve with dietary and lifestyle measures
At Spiritual Homeopathy Clinic, consultations are available at multiple branches in Hyderabad, including Kukatpally, Chandanagar, Dilsukhnagar, and Nallagandla. In-clinic, online, and international consultations are available for individuals who are unable to visit in person. A professional assessment supports an individualized care approach based on symptoms, blood sugar status, and overall health.
For appointments or guidance, contact 9069 176 176.
FAQ
1. What is Diabetes Mellitus?
Diabetes Mellitus is a group of metabolic disorders characterized by persistently high blood sugar levels (hyperglycemia). It occurs due to defects in insulin secretion, insulin action, or both. If not appropriately managed, diabetes may lead to short- and long-term health complications.
2. What Causes Diabetes Mellitus?
The causes of Diabetes Mellitus vary depending on the type and underlying health factors, including:
Destruction of pancreatic beta cells leading to absolute insulin deficiency
Genetic mutations affecting insulin production or regulation
Pancreatic disorders such as pancreatitis or cystic fibrosis
Endocrine disorders including acromegaly or hyperthyroidism
Drug-induced factors, such as prolonged use of certain medications
Certain viral or congenital infections
Insulin receptor defects
Genetic syndromes such as Down syndrome or Turner syndrome
Identifying these contributing factors supports an individualized care approach.
3. What are the Symptoms of Diabetes Mellitus?
Common symptoms of Diabetes Mellitus may include:
Polyuria (frequent urination), polydipsia (increased thirst), and polyphagia (increased hunger)
Unexplained weight loss, fatigue, and general weakness
Pruritus (itching) in women or balanitis in men
Reduced libido or erectile dysfunction
Blurred vision
Abdominal pain in cases associated with complications such as ketoacidosis
Medical consultation is advised if symptoms are frequent, progressive, or interfere with daily activities.
4. What are the Types of Diabetes Mellitus?
Type 1 Diabetes Mellitus: Insulin-dependent diabetes, commonly developing in childhood or adolescence
Type 2 Diabetes Mellitus: Non–insulin-dependent diabetes, more commonly seen in adults and associated with lifestyle factors
Maturity-Onset Diabetes of the Young (MODY): A genetically inherited form occurring at a younger age
Secondary Diabetes: Diabetes resulting from other medical conditions or long-term medication use
Gestational Diabetes Mellitus: Diabetes that develops during pregnancy
Impaired Glucose Tolerance (IGT): A borderline or pre-diabetic state with elevated blood glucose levels
5. When should someone with diabetes seek medical consultation?
Medical consultation is recommended if symptoms appear, blood sugar levels remain uncontrolled, or risk factors such as family history, obesity, or pregnancy are present. Early evaluation supports appropriate monitoring and long-term management.